Search for
Filter By
Rating
Price in $
Search Results 'Adult Learning Principles'
Showing results — Page 1 (max 300)
Sort by
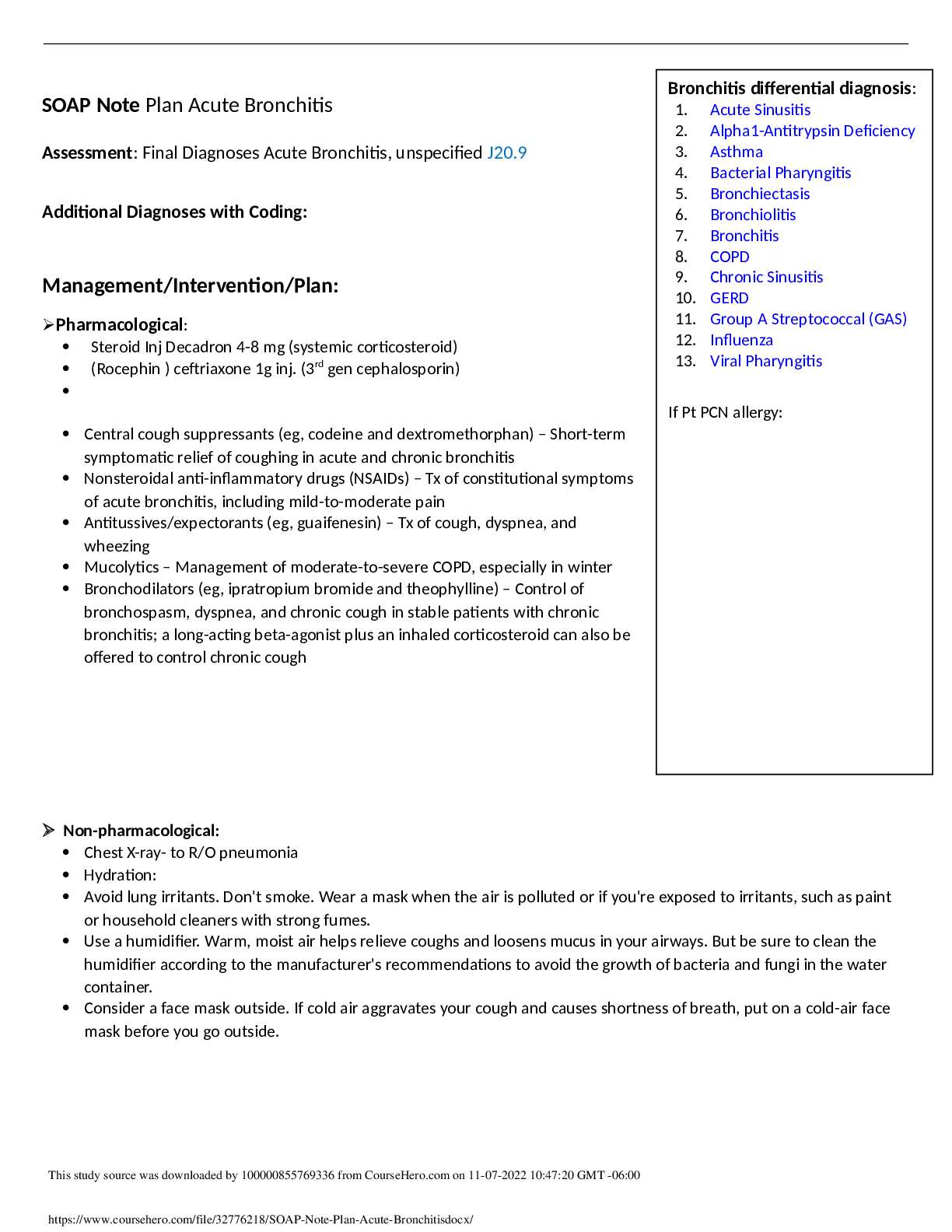
*NURSING > SOAP NOTE > Monroe College NURSING 812 Adult Assessment SOAP Note Plan Acute Bronchitis Assessment: Final Diagnoses Acute Bronchitis, unspecified J20.9 Additional Diagnoses with Coding: Management/Intervention/Plan:
*NURSING > SOAP NOTE > Monroe College NURSING 812 Adult Assessment Mrs. C., a 47-year-old Navajo woman, comes to the clinic with a burning sensation in her epigastric area extending into her sternum.
*NURSING > SOAP NOTE > NURSING 812 Adult Assessment Soap Note: Follow up BP visit Patient initials and age: MD, 47 Subjective Data: Chief complaint: Patient states he is, “following up on my high blood pressure.”
*NURSING > SOAP NOTE > NURSING 812 Adult Assessment Migraine SOAP Note Chief Complaint: “I am here for an evaluation of my headache.”
*NURSING > SOAP NOTE > Monroe College NURSING 812 Adult Assessment SOAP Note: Otitis Media Patient initial and age: C.M., 2 years old Gender: Male Race: White
*NURSING > SOAP NOTE > ADULT 620 Week 4 make up SOAP note clinical patient