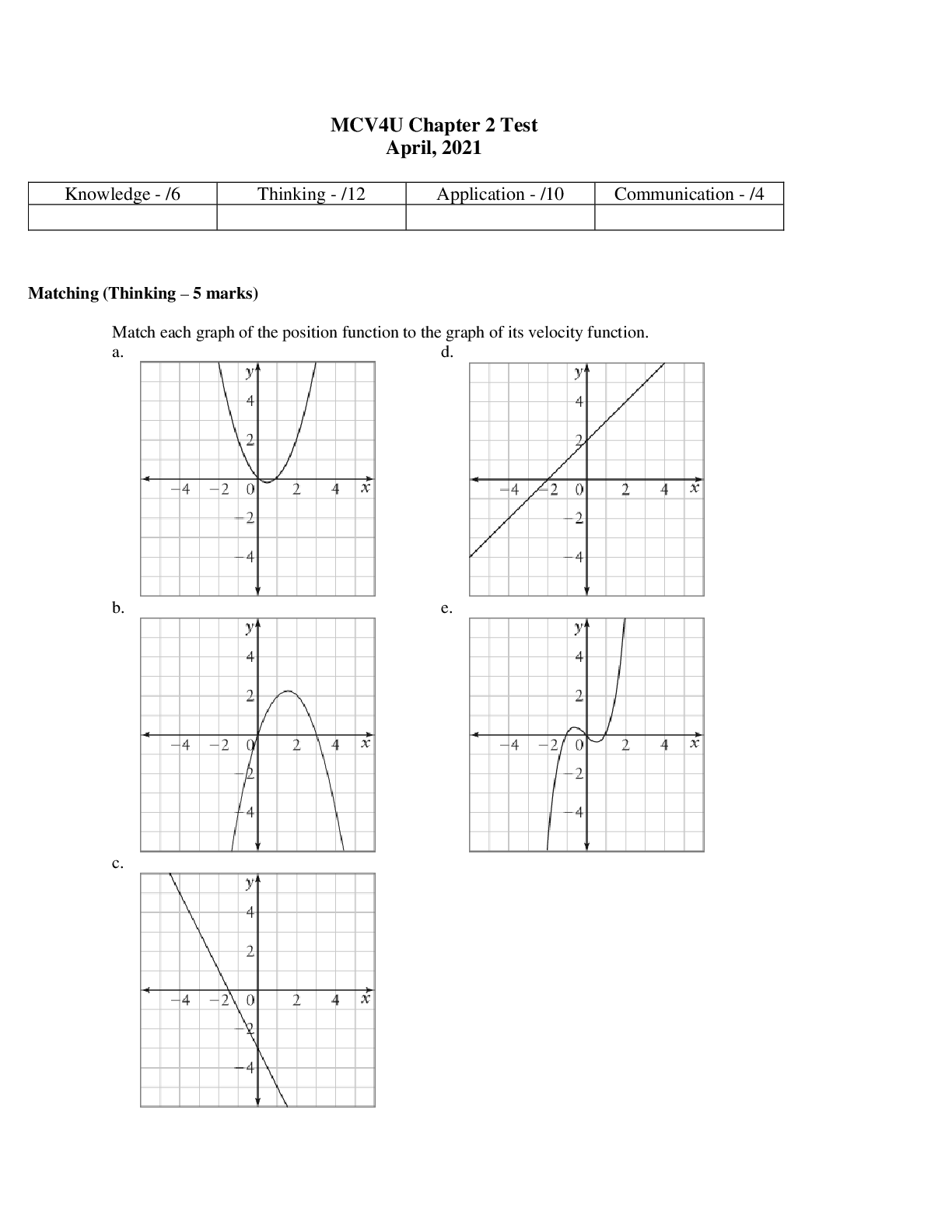
NURSING 3210 Exit HESI
Document Content and Description Below
NURSING 3210
Exit HESI
Leadership and Management
Legal Aspects of Nursing
o Often an NCLEX-RN® question asks who should explain a surgical procedure to the client. The
answer is the health care provider. Remember
...
NURSING 3210
Exit HESI
Leadership and Management
Legal Aspects of Nursing
o Often an NCLEX-RN® question asks who should explain a surgical procedure to the client. The
answer is the health care provider. Remember that it is the nurse’s responsibility to be sure that the
operative permit is signed and is on the chart. It is not the nurse’s responsibility to explain the
procedure to the client.
o Often questions are asked regarding the Good Samaritan Act, which is the means of protecting a
nurse when she or he is performing emergency care.
Good Samaritan Act: Protects health practitioners against malpractice claims for care
provided in emergency situations (e.g., the nurse gives aid at the scene to an automobile
accident victim).
o If the nurse carries out a health care provider’s prescription for which he or she is not prepared and
does not inform the health care provider of his or her lack of preparation, the nurse is solely liable
for any damages.
If the nurse informs the health care provider of his or her lack of preparation in carrying out
a prescription and carries out the prescription anyway, the nurse and the health care
provider are liable for any damages.
o Assignments are often tested on the NCLEX-RN. The Nurse Practice Acts of each state governs
policies related to making assignments. Usually, when determining who should be assigned to do a
sterile dressing change, for example, a licensed nurse should be chosen—that is, an RN or licensed
practical nurse (LPN) that has been checked off on this procedure.
o Restraints of any kind may constitute false imprisonment. Freedom from unlawful restraint is a
basic human right and is protected by law.
Apply restraints properly; check restraints frequently to see that they are not causing injury
and record such monitoring; remove restraints as soon as possible; use restraints only as a
last resort
o A patient must give written consent before health care providers can use or disclose personal
health information; health care providers must give patients notice about providers’
responsibilities regarding patient confidentiality; patients must have access to their medical
records; providers who restrict access must explain why and must offer patients a description of
the complaint process; patients have the right to request that changes be made in their medical
records to correct inaccuracies; health care providers must follow specific tracking procedures for
any disclosures made that ensure accountability for maintenance of patient confidentiality; patients
have the right to request that health care providers restrict the use and disclosure of their personal
health information, though the provider may decline to do so.
Leadership and Management
o Assertive communication starts with “I need” rather than with “You must.”
o Motivation comes from within an individual. A nurse leader can provide an environment that will
promote motivation through positive feedback, respect, and seeking input. Look for responses that
demonstrate these behaviors.
o Effective leadership involves assertive management skills (i.e. democratic/participative). Look for
responses that demonstrate that the nurse is using assertive communication skills.
o Delegating to the right person requires that the nurse be aware of the qualifications of the
delegator: appropriate education, training, skills, experience, and demonstrated and documented
competence.
Five Rights of Delegation (as defined by the National Council of State Boards of Nursing)
Right task: Is this a task that can be delegated by a nurse?
Right circumstance: Considering the setting and available resources, should
delegation take place? Right person: Is the task being delegated by the right person to the right person?
Right direction/communication: Is the nurse providing a clear, concise description
of the task, including limits and expectations?
Right supervision: Once the task has been delegated, is appropriate supervision
maintained.
UAPs generally do not perform invasive or sterile procedures.
The RN is accountable for adhering to the three basic aspects of supervision when
delegating to other health care personnel, such as LPNs, graduate nurses, inexperienced
nurses, student nurses, and UAPs.
Remember the nursing process: Assessments, analysis, diagnosis, planning, and evaluation
(any activity requiring nursing judgment) may not be delegated to UAP. Delegated activities
fall within the implementation phase of the nursing process.
Priorities often center on which client should be assessed first by the nurse. Ask yourself:
Which client is the most critically ill? Which client is most likely to experience a significant
change in condition? Which client requires assessment by an RN?
Delegation is as follows:
Inserting a Foley catheter is a sterile invasive procedure and should not be
delegated to a UAP
Measuring and recording intake and output falls within the implementation phase of
the nursing process and does not require nursing judgment. However, evaluation of
the intake and output (I&O) must be done by the nurse.
Client teaching requires the abilities of a nurse and should not be delegated. The
UAP may be instructed to report anything unusual that is observed and any
symptoms reported by the client, but this does not replace assessment by the nurse.
Assessment must be performed by the nurse and should not be delegated. The UAP
may be instructed to report anything unusual that is observed, or any symptoms
reported by the client, but this does not replace assessment by the nurse.
o The nurse manager must analyze all the desired outcomes involved when assigning rooms for
clients or assigning client care responsibilities. A client with an infection should not be assigned to
share a room with a surgical or immunocompromised client. A nurse’s client care management
should be based on the nurse’s abilities, the individual client’s needs, and the needs of the entire
group of assigned clients. Safety and infection control are high priorities.
o Change causes anxiety. An effective nurse change agent uses problem-solving skills to recognize
factors such as anxiety that contribute to resistance to change and uses decision-making and
interpersonal skills to overcome that resistance. Interventions that demonstrate these skills include
seeking input, showing respect, valuing opinions, and building trust.
Disaster Nursing
o It is important to remember that in disaster and bioterrorism management, the nurse must
consider both the individual and the community.
Advanced Clinical Concepts
Respiratory Failure
o ARDS is an unexpected, catastrophic pulmonary complication occurring in a person with no
previous pulmonary problems. Clients are critically ill and are managed in an intensive care setting.
The mortality rate is high (50%).
o Interventions to prevent complications of clients on mechanical ventilation with ARDS:
Elevate head of bed (HOB) to at least 30 degrees.
Assist with daily awakening (“sedation vacation”).
Implement a comprehensive oral hygiene program.
Implement a comprehensive mobilization program.
o Suction only when secretions are present.
o Before drawing a sample for ABGs from the radial artery, perform the Allen test to assess collateral
circulation.
Make the client’s hand blanch by obliterating both the radial and the ulnar pulses. Thenrelease the pressure over the ulnar artery only. If flow through the ulnar artery is good,
flushing will be seen immediately.
The Allen test is then positive, and the radial artery can be used for puncture. If the Allen
test is negative, repeat on the other arm.
If this test is also negative, seek another site for arterial puncture.
The Allen test ensures collateral circulation to the hand if thrombosis of the radial artery
should follow the puncture.
o Cardinal signs of Acute Respiratory Failure in children are Restlessness, Tachypnea, Tachycardia,
and Diaphoresis.
o PCO2 >45 or PO2 <60 on 50% O2 signifies respiratory failure.
o A child in severe distress should be on 100% O2.
Shock and DIC
o Early signs of shock are agitation and restlessness resulting from cerebral hypoxia.
o Severe shock leads to widespread cellular injury and impairs the integrity of the capillary
membranes. Fluid and osmotic proteins seep into the extravascular spaces, further reducing cardiac
output.
o A vicious circle of decreased perfusion to all cellular level activities ensues. All organs are damaged,
and if perfusion problems persist, the damage can be permanent.
o All types of shock can lead to systemic inflammatory response syndrome (SIRS) and result in
multiple organ dysfunction syndrome (MODS).
o If cardiogenic shock exists in the presence of pulmonary edema (i.e., from pump failure), position
client to reduce venous return (High Fowler position with legs down) to decrease further venous
return to the left ventricle.
o All vasopressor and vasodilator drugs are potent and dangerous and require that the client be
titrated prudently.
o You are caring for a woman who was in a severe automobile accident several days earlier. She has
several fractures and internal injuries. The exploratory laparotomy was successful in controlling
the bleeding. However, today you find that this client is bleeding from her incision, is short of
breath, and has a weak, thready pulse, cold and clammy skin, and hematuria.
What do you think is wrong with the client, and what would you expect to do about it?
These are typical signs and symptoms of DIC crisis. Expect to administer IV heparin
to block the formation of thrombin (Coumadin does not do this). However, the client
described is already past the coagulation phase and into the hemorrhagic phase. Her
care would include administration of clotting factors, along with palliative treatment
of the symptoms as they arise. (Her prognosis is poor.)
Resuscitation
o NCLEX-RN® questions on cardiopulmonary resuscitation (CPR) often deal with prioritization of
actions.
Question: What actions are required for each of the following situations?
A 24-year-old motorcycle accident victim with a ruptured artery of the leg who is
pulseless and apneic
A 36-year-old first-time pregnant woman who arrests during labor
A 17-year-old with no pulse or respirations who is trapped in an overturned car that
is starting to burn
A 40-year-old businessman who arrests 2 days after a cervical laminectomy
o When to seek emergency medical services (EMS):
The American Heart Association recommends that those with known angina pectoris
activate an emergency medical system if chest pain does NOT go away immediately with
rest or is NOT relieved in 5 minutes after taking nitroglycerin or if additional symptoms
such as nausea and sweating are also present with the chest pain.
A person with previously unrecognized coronary disease experiencing chest pain persisting
for 2 minutes or longer should seek emergency medical treatment.
o Initiate CPR with BLS guidelines immediately; then move on to advanced cardiac life support
(ACLS) guidelines.
o When significant arterial acidosis is noted, try to reduce PCO2 by increasing ventilation, which willcorrect arterial, venous, and tissue acidosis.
Bicarbonate may exacerbate acidosis by producing CO2. ACLS guidelines recommend that
bicarbonate not be used unless hyperkalemia, tricyclic antidepressant overdose, or preexisting metabolic acidosis is documented.
o In the pulseless arrest algorithm, the search for and treatment of possible contributing factors
should include checking for hypovolemia, hypoxia, hydrogen ion acidosis, hypokalemia and
hyperkalemia, hypoglycemia, hypothermia, toxins, tamponade (cardiac), tension pneumothorax,
thrombosis (cardiac, pulmonary), and trauma.
Fluid and Electrolyte Balance
o Changes in osmolarity cause shifts in fluid. The osmolarity of the extracellular fluid (ECF) is almost
entirely due to sodium. The osmolarity of intracellular fluid (ICF) is related to many particles, with
potassium being the primary electrolyte. The pressures in the ECF and the ICF are almost identical.
If either ECF or ICF changes in concentration, fluid shifts from the area of lesser concentration to
the area of greater concentration.
o Dextrose 10% is a hyperosmolar solution and should be administered IV.
o Normal saline is an isotonic solution and is used for irrigations, such as bladder irrigations or IV
flush lines with intermittent IV medication.
o Use only isotonic (neutral) solutions in irrigations, infusions, etc., unless the specific aim is to shift
fluid to intracellular or extracellular spaces.
o Potassium imbalances are potentially life-threatening; they must be corrected immediately. A low
magnesium level often accompanies a low K+, especially with the use of diuretics.
o Fluid Volume Deficit: Dehydration
Elevated blood urea nitrogen (BUN): The BUN measures the amount of urea nitrogen in the
blood. Urea is formed in the liver as the end product of protein metabolism. The BUN is
directly related to the metabolic function of the liver and the excretory function of the
kidneys.
Creatinine, as with BUN, is excreted entirely by the kidneys and is therefore directly
proportional to renal excretory function. However, unlike BUN, the creatinine level is
affected very little by dehydration, malnutrition, or hepatic function. The daily production of
creatinine depends on muscle mass, which fluctuates very little. Therefore, it is a better test
of renal function than is the BUN. Creatinine is generally used in conjunction with the BUN
test, and they are normally in a 1:20 ratio.
Serum osmolality measures the concentration of particles in a solution. It refers to the fact
that the same amount of solute is present, but the amount of solvent (fluid) is decreased.
Therefore, the blood can be considered “more concentrated.”
Urine osmolality and specific gravity increase.
o Check the IV tubing container to determine the drip factor because drip factors vary. The most
common drip factors are 10, 12, 15, and 60 drops per milliliter. A microdrip = 60 drops per
milliliter.
o Flushing a saline lock efficiently requires approximately 1.5 times the amount of fluid the tubing
will hold. Remember to use sterile technique to prevent complications, such as infiltration, emboli,
and infection.
o The acronym ROME can help you remember: respiratory, opposite, metabolic, equal.
Electrocardiogram (ECG/EKG)
o Review the order of blood flow through the heart:
Unoxygenated blood flows from the superior and inferior vena cava into the right atrium,
then to the right ventricle. It flows out of the heart through the pulmonary artery, to the
lungs for oxygenation. The pulmonary vein delivers oxygenated blood back to the left
atrium, then to the left ventricle (largest, strongest chamber), and out the aorta.
o Review the three structures that control the one-way flow of blood through the heart:
Atrioventricular valves
Tricuspid (right side)
Mitral (left side)
Semilunar valves
Pulmonic (in pulmonary artery) Aortic (in aorta)
Chordae tendineae
Papillary muscles
o The T wave represents repolarization of the ventricle, so this is a critical time in the heartbeat. This
action represents a resting and regrouping stage so that the next heartbeat can occur. If
defibrillation occurs during this phase, the heart can be thrust into a life-threatening dysrhythmia.
(NO DEFIBRILLATION DURING T-WAVE)
o Methods of Estimating Heart Rate Using an Electrocardiogram Tracing
Measure the interval between consecutive QRS complexes, determine the number of small
squares, and divide 1500 by that number. This method is used only when the heart rhythm
is regular.
Measure the interval between consecutive QRS complexes, determine the number of large
squares, and divide 300 by that number. This method is used only when the heart rhythm is
regular.
Determine the number of RR intervals within 6 seconds and multiply by 10. The ECG paper
is conveniently marked at the top with slashes that represent 3-second intervals. This
method can be used when the rhythm is irregular. If the rhythm is extremely irregular, an
interval of 30 to 60 seconds should be used.
Count the number of big blocks between the same point in any two successive QRS
complexes (usually R wave to R wave) and divide into 300 because there are 300 big blocks
in 1 minute. It is easiest to use a QRS that falls on a dark line. If little blocks are left over
when counting big blocks, count each little block as 0.2, add this to the number of big blocks,
and then divide by 300.
The memory method relies on memorization of the following sequence: 300, 150, 100, 75,
60, 50, 43, 37, 33, and 30. Find a QRS complex that falls on the dark line representing 0.2
second or a big block, and count backward to the next QRS complex. Each dark line is a
memorized number. This is the method most widely used in hospitals for calculating heart
rates for regular rhythms.
o Observe the client for tolerance of the current rhythm. This information is the most important data
the nurse can collect on a client with an arrhythmia.
o NCLEX-RN questions are likely to relate to early recognition of abnormalities and associated
nursing actions. Remember to monitor the client as well as the machine! If the ECG monitor shows a
severe dysrhythmia but the client is sitting up quietly watching television without any sign of
distress, assess to determine if the leads are attached properly.
Perioperative Care
o Marking the operative site is required for procedures involving right/left distinctions, multiple
structures (fingers, toes), and levels (spinal procedures). Site marking should be done with the
involvement of the client.
o Wound dehiscence is separation of the wound edges; it is more likely to occur with vertical
incisions. It usually occurs after the early postoperative period, when the client’s own granulation
tissue is “taking over” the wound, after absorption of the sutures has begun. Evisceration of the
wound is protrusion of intestinal contents (in an abdominal wound) and is more likely in clients
who are older, diabetic, obese, or malnourished and have prolonged paralytic ileus.
o NCLEX-RN items may focus on the nurse’s role in terms of the entire perioperative process.
Example: A 43-year-old mother of two teenage daughters enters the hospital to have her
gallbladder removed in a same-day surgery using an endoscope instead of an incision. What
nursing needs will dominate each phase of her short hospital stay?
Preparation phase: education about postoperative care, including NPO, assistance
with meeting family needs
Operative phase: assessment, management of the operative suite
Postanesthesia phase: pain management, postanesthesia precautions
Postoperative phase: prevention of complications, assessment for pain
management, and teaching about dietary restrictions and activity levels
o NCLEX-RN items may focus on delivery of safe effective care. Time Out, Surgical Care Improvement Project (SCIP) protocol implementation, and HandOff communication are all best practices implemented to prevent serious medical error
during the perioperative period.
Time Out occurs before making the incision and the entire surgical team pauses as
the surgical site listed on the consent is read aloud. The entire team confirms that
this information is correct.
SCIP protocols are best practices for safety and quality that are implemented during
the preoperative period and followed up on during the postoperative period. The
focus of the SCIP protocol is on prevention of infection, prevention of serious cardiac
events, and prevention of venous thromboembolism.
The Hand-Off communication is the transfer of relevant patient information during
the perioperative period, which is standardized and must include an opportunity to
ask and to respond to questions.
HIV Infection
o HIV clients with tuberculosis require respiratory isolation. Tuberculosis is the only real risk to nonpregnant caregivers that is not related to a break in standard precautions (e.g., needle sticks).
o Standard Precautions
Wash hands, even if gloves have been worn to give care.
Wear exam gloves for touching blood or body fluids or any non-intact body surface.
Wear gowns during any procedure that might generate splashes (e.g., changing clients with
diarrhea).
Use masks and eye protection during activity that might disperse droplets (e.g., suctioning).
Do not recap needles; dispose of in puncture-resistant containers.
Use mouthpiece for resuscitation efforts.
o Caregivers who are pregnant may choose not to care for a client with cytomegalovirus (CMV).
o Pediatric HIV is often evidenced by lymphoid interstitial pneumonitis, pulmonary lymphoid
hyperplasia, and opportunistic infections.
o The focus of NCLEX-RN questions is likely to be assessment of early signs of the disease and
management of complications associated with HIV.
Pain
o For narcotic-induced respiratory depression, naloxone (Narcan) may be administered as prescribed
by the health care provider.
o Use noninvasive methods for pain management when possible:
Relaxation exercises
Distraction
Imagery
Biofeedback
Interpersonal skills
Physical care: altering positions, touch, hot and cold applications
o Narcotic analgesics are preferred for pain relief because they bind to the various opiate receptor
sites in the CNS. Morphine is often the preferred narcotic (remember, it causes respiratory
depression). Another agonist is methadone.
o Narcotic antagonists block the attachment of narcotics such as naloxone (Narcan) to the receptors.
Once Narcan has been given, additional narcotics cannot be given until the Narcan effects have
passed.
Death and Grief
o Do not take away the coping style used in a crisis state.
o Denial is a very useful and needed tool for some at the initial stage. Support, do not challenge,
unless it hinders or blocks treatment, endangering the patient
Medical-Surgical
Respiratory
o Fever can cause dehydration because of excessive fluid loss due to diaphoresis. Increased
temperature also increases metabolism and the demand for O2.o Clients at High Risk for Pneumonia
Altered level of consciousness
Depressed or absent gag and cough reflexes
Susceptible to aspirating oropharyngeal secretions, including alcoholics, anesthetized
individuals
Brain injury
Drug overdose
Stroke victims
Immunocompromised
o Bronchial breath sounds are heard over areas of density or consolidation. Sound waves are easily
transmitted over consolidated tissue.
o Hydration
Thins out the mucus trapped in the bronchioles and alveoli, facilitating expectoration
Is essential for client experiencing fever
Is important because 300 to 400 mL of fluid is lost daily by the lungs through evaporation
o Irritability and restlessness are early signs of cerebral hypoxia; the client’s brain is not receiving
enough O2.
o Pneumonia Preventives
Older adults: Flu shots; pneumonia immunizations; avoiding sources of infection and indoor
pollutants (dust, smoke, and aerosols); no smoking
Immunosuppressed and debilitated persons: Flu shots, pneumonia immunizations, infection
avoidance, sensible nutrition, adequate intake, balance of rest and activity
Comatose and immobile persons: Elevation of head of bed to feed and for 1 hour after
feeding; frequently turning
Patients with functional or anatomic asplenia: Flu and pneumonia immunizations
o Exposure to tobacco smoke is the primary cause of COPD in the United States.
o Compensation occurs over time in clients with chronic lung disease, and ABGs are altered.
o As COPD worsens, the amount of O2 in the blood decreases (hypoxemia) and the amount of carbon
dioxide (CO2) in the blood increases (hypercapnia), causing chronic respiratory acidosis (increased
arterial carbon dioxide [Paco2]), which results in metabolic alkalosis (increased arterial
bicarbonate) as compensation.
o Not all clients with COPD are CO2 retainers, even when hypoxemia is present, because CO2 diffuses
more easily across lung membranes than O2.
o In advanced emphysema, due to the alveoli being affected, hypercarbia is a problem, rather than in
bronchitis, where the airways are affected.
o It is imperative that baseline data be obtained for the client.
o Productive cough and comfort can be facilitated by semi-Fowler or high-Fowler position, which
lessens pressure on the diaphragm by abdominal organs. Gastric distention becomes a priority in
these clients because it elevates the diaphragm and inhibits full lung expansion.
o Normal ABG Values
pH: 7.35 to 7.45
PCO2: 35-45 mm Hg
PO2: 80-100 mm Hg
HCO3-: 21-28 mEq/L
o Pink puffer: Barrel chest is indicative of emphysema and is caused by use of accessory muscles to
breathe. The person works harder to breathe, but the amount of O2 taken in is adequate to
oxygenate the tissues.
o Blue bloater: Insufficient oxygenation occurs with chronic bronchitis and leads to generalized
cyanosis and often right-sided heart failure (cor pulmonale).
o Cells of the body depend on O2 to carry out their functions. Inadequate arterial oxygenation is
manifested by cyanosis and slow capillary refill (<3 seconds). A chronic sign is clubbing of the
fingernails, and a late sign is clubbing of the fingers.
o Nursing Skills: Respiratory Client
Suctioning (Tracheal)
Suction when adventitious breath sounds are heard, when secretions are present atendotracheal tube, and when gurgling sounds are noted.
Use aseptic/sterile technique throughout procedure.
Wear mask and goggles.
Advance catheter until resistance is felt.
Apply suction only when withdrawing catheter (gently rotate catheter when
withdrawing).
Never suction for more than 10 to 15 seconds, and pass the catheter only three or
fewer times.
Oxygenate with 100% O2 for 1 to 2 minutes before and after suctioning to prevent
hypoxia.
Ventilator Setting Maintenance
Verify that alarms are on.
Maintain settings and check often to ensure that they are specifically set as
prescribed by health care provider.
Verify functioning of ventilator at least every 4 hours.
Oxygen Administration
Nasal cannula: low O2 flow for low O2 concentrations (good for COPD)
Simple face mask: low flow, but effectively delivers high O2 concentrations; cannot
deliver <40% O2
Non-rebreather mask: low flow, but delivers highest O2 concentrations (60% to
90%)
Partial rebreather mask: low-flow O2 reservoir bag attached; can deliver high O2
concentrations
Venturi mask: high-flow system; can deliver exact O2 concentration
Pulse Oximetry
Easy measurement of O2 saturation
Should be >90%, ideally above 95%
Noninvasive, fastens to finger, toe, or earlobe
No nail polish
Must have good peripheral perfusion to be accurate
Tracheostomy Care
Aseptic technique (remove inner cannula only from stoma)
Clean nondisposable inner cannula with H2O2; rinse with sterile saline
4 × 4 gauze dressing is butterfly-folded
Respiratory Isolation Technique
Mask is required for anyone entering room.
Private room is required with negative air pressure.
Client must wear mask if leaving room.
Proper Use of an Inhaler
Have client exhale completely.
Grip mouthpiece (in mouth) only if client has a spacer; otherwise, keep the mouth
open to bring in volume of air with misted medication. While inhaling slowly, push
down firmly on the inhaler to release the medication.
Use bronchodilator inhaler before steroid inhaler.
Wait at least 1 minute between puffs (inhaled doses).
After steroid inhaler use, patient must perform oral care to prevent fungal
infections.
o Health Promotion
Eating consumes energy needed for breathing. Offer mechanically soft diets, which do not
require as much chewing and digestion. Assist with feeding if needed.
Prevent secondary infections; avoid crowds, contact with persons who have infectious
diseases, and respiratory irritants (tobacco smoke).
Teach client to report any change in characteristics of sputum.
Encourage client to hydrate well (3 L/day) and decrease caffeine due to diuretic effect. Obtain immunizations when needed (flu and pneumonia).
o When asked to prioritize nursing actions, use the ABC rule:
Airway first
Then breathing
Then circulation
**In CPR circumstances, follow the CAB guidelines.
o Look and listen! If breath sounds are clear but the client is cyanotic and lethargic, adequate
oxygenation is not occurring.
o The key to respiratory status is assessment of breath sounds as well as visualization of the client.
Breath sounds are better described, not named; e.g., sounds should be described as crackles,
wheezes, or high-pitched whistling sounds rather than rales, rhonchi, etc., which may not mean the
same thing to each clinical professional.
o Watch for NCLEX-RN® questions that deal with O2 delivery. In adults, O2 must bubble through some
type of water solution so it can be humidified if given at >4 L/min or delivered directly to the
trachea. If given at 1 to 4 L/min or by mask or nasal prongs, the oropharynx and nasal pharynx
provide adequate humidification.
o With cancer of the larynx, the tongue and mouth often appear white, gray, dark brown, or black and
may appear patchy.
o Tracheostomy care involves cleaning the inner cannula, suctioning, and applying clean dressings.
o Air entering the lungs is humidified along the nasobronchial tree. This natural humidifying pathway
is gone for the client who has had a laryngectomy. If the air is not humidified before entering the
lungs, secretions tend to thicken and become crusty.
o A laryngectomy tube has a larger lumen and is shorter than the tracheostomy tube. Observe the
client for any signs of bleeding or occlusion, which are the greatest immediate postoperative risks
(first 24 hours).
o Fear of choking is very real for laryngectomy clients. They cannot cough as they could earlier
because the glottis is gone. Teach the glottal stop technique to remove secretions (take a deep
breath, momentarily occlude the tracheostomy tube, cough, and simultaneously remove the finger
from the tube).
o Tuberculosis (TB) Skin Test
A positive TB skin test in a healthy client is exhibited by an induration 10 mm or greater in
diameter 48 to 72 hours after the skin test.
Anyone who has received a bacillus Calmette-Guérin (BCG) vaccine will have a positive skin
test and must be evaluated with an initial chest radiograph. A health history with signs and
symptoms form may be filled out annually until signs and symptoms arise; then another
radiograph is required. Chest x-rays are required on new employment; employer may
require an x-ray every 5 years.
o Teaching is very important with the client with TB. Drug therapy is usually long term (6 months or
longer). It is essential that the client take the medications as prescribed for the entire time. Skipping
doses or prematurely terminating the drug therapy can result in a public health hazard.
Teaching Points
Rifampin: Reduces effectiveness of oral contraceptives; client should use other birth
control methods during treatment; gives body fluids orange tinge; stains soft contact
lenses
Isoniazid (INH): Increased phenytoin (Dilantin) levels
Ethambutol: Vision check before starting therapy and monthly thereafter; may have
to take for 1 to 2 years
Teach rationale for combination drug therapy to increase compliance. Resistance
develops more slowly if several anti-TB drugs given, instead of just one drug at a
time.
o Some tumors are so large that they fill entire lobes of the lung. When removed, large spaces are left.
Chest tubes are not usually used with these clients because it is helpful if the mediastinal cavity,
where the lung used to be, fills up with fluid. This fluid helps to prevent the shift of the remaining
chest organs to fill the empty space.
o Chest Tubes If the chest tube becomes disconnected, do not clamp! Immediately place the end of the tube
in a container of sterile saline or water until a new drainage system can be connected.
If the chest tube is accidentally removed from the client, the nurse should cover with a dry
sterile dressing. If an air leak is noted, tape the dressing on three sides only; this allows air
to escape and prevents the formation of a tension pneumothorax. Notify the health care
provider.
Fluctuations (tidaling) in the fluid will occur if there is no external suction. These fluctuating
movements are a good indicator that the system is intact; they should move upward with
each inspiration and downward with each expiration. If fluctuations cease, check for kinked
tubing, accumulation of fluid in the tubing, occlusions, or change in the client’s position,
because expanding lung tissue may be occluding the tube opening. Remember, when
external suction is applied, the fluctuations cease.
o Various pathophysiologic conditions can be related to the nursing diagnosis Ineffective breathing
patterns.
Inability of air sacs to fill and empty properly (emphysema, cystic fibrosis)
Obstruction of the air passages (carcinoma, asthma, chronic bronchitis)
Accumulation of fluid in the air sacs (pneumonia)
Respiratory muscle fatigue (COPD, pneumonia)
Renal
o Normally, kidneys excrete approximately 1 mL of urine per kg of body weight per hour.
o For adults, total daily urine output ranges between 1500 and 2000 mL depending on the amount
and type of fluid intake, amount of perspiration, environmental or ambient temperature, and the
presence of vomiting or diarrhea.
o Electrolytes are profoundly affected by kidney problems (a favorite NCLEX-RN topic). There must
be a balance between extracellular fluid and intracellular fluid to maintain homeostasis. A change in
the number of ions or in the amount of fluid will cause a shift in one direction or the other. Sodium
and chloride are the primary extracellular ions. Potassium and phosphate are the primary
intracellular ions.
o In some cases, persons in ARF may not experience the oliguric phase but may progress directly to
the diuretic phase, during which the urine output may be as much as 10 L per day.
o Body weight is a good indicator of fluid retention and renal status. Obtain accurate weights of all
clients with renal failure; obtain weight on the same scale at the same time every day.
o Fluid Volume Alterations
Excess Fluid
Dyspnea
Tachycardia
JVD
Peripheral edema
Pulmonary edema
Weight gain
Fluid-Deficient Symptoms
Decreased urine output
Reduction in body weight
Decreased skin turgor
Dry mucous membranes
Hypotension
Tachycardia
Weight loss
o Watch for signs of hyperkalemia: dizziness, weakness, cardiac irregularities, muscle cramps,
diarrhea, and nausea.
o Potassium has a critical safe range (3.5 to 5.0 mEq/L) because it affects the heart, and any
imbalance must be corrected by medications or dietary modification. Limit high-potassium foods
(bananas, orange juice, cantaloupe, strawberries, avocados, spinach, fish) and salt substitutes,
which are high in potassium.
o Clients with renal failure retain sodium. With water retention, the sodium becomes diluted andserum levels may appear near normal. With excessive water retention, the sodium levels appear
decreased (dilution). Limit fluid and sodium intake in ARF clients.
o During oliguric phase, minimize protein breakdown and prevent rise in BUN by limiting protein
intake. When the BUN and creatinine return to normal, ARF is determined to be resolved.
o Accumulation of waste products from protein metabolism is the primary cause of uremia. Protein
must be restricted in CRF clients. However, if protein intake is inadequate, a negative nitrogen
balance occurs, causing muscle wasting. The glomerular filtration rate (GFR) is most often used as
an indicator of the level of protein consumption.
o The major difference between dialysate for hemodialysis and peritoneal dialysis is the amount of
glucose. Peritoneal dialysis dialysate is much higher in glucose. For this reason, if the dialysate is
left in the peritoneal cavity too long, hyperglycemia may occur.
o Dialysis Covered by Medicare
All persons in the United States are eligible for Medicare as of their first day of dialysis
under special ESRD funding.
Medicare card will indicate ESRD.
Transplantation is covered by Medicare procedure; coverage terminates 6 months
postoperative if dialysis is no longer required.
o Protein intake is restricted until blood chemistry shows ability to handle the protein catabolites,
urea and creatinine. Ensure high calorie intake so protein is spared for its own work; give hard
candy, jelly beans, or flavored carbohydrate powders.
o As kidneys fail, medications must often be adjusted. Of particular importance is digoxin toxicity
because digitalis preparations are excreted by the kidneys. Signs of toxicity in adults include
nausea, vomiting, anorexia, visual disturbances, restlessness, headache, cardiac dysrhythmias, and
pulse <60 bpm.
o The key to resolving UTIs with most antibiotics is to keep the blood level of the antibiotic constant.
It is important to tell the client to take the antibiotics around the clock and not to skip doses so that
a consistent blood level can be maintained for optimal effectiveness.
o Location of the pain can help to determine the location of the stone.
Flank pain usually means the stone is in the kidney or upper ureter. If the pain radiates to
the abdomen or scrotum, the stone is likely to be in the ureter or bladder.
Excruciating spastic-type pain is called colic.
During kidney stone attacks, it is preferable to administer pain medications at regularly
scheduled intervals rather than PRN to prevent spasm and optimize comfort.
o Percutaneous nephrostomy: A needle or catheter is inserted through the skin into the calyx of the
kidney. The stone may be dissolved by percutaneous irrigation with a liquid that dissolves the stone
or by ultrasonic sound waves (lithotripsy) that can be directed through the needle or catheter to
break up the stone, which then can be eliminated through the urinary tract.
o Bladder spasms frequently occur after TURP. Inform the client that the presence of the oversized
balloon on the catheter (30 to 45 mL inflated) will cause a continuous feeling of needing to void.
The client should not try to void around the catheter because this can precipitate bladder spasms.
Medications to reduce or prevent spasms should be given.
o Instillation of hypertonic or hypotonic solution into a body cavity will cause a shift in cellular fluid.
Use only sterile saline for bladder irrigation after TURP because the irrigation must be isotonic to
prevent fluid and electrolyte imbalance.
o Inform the client prior to discharge that some bleeding is expected after TURP. Large amounts of
blood or frank bright bleeding should be reported. However, it is normal for the client to pass small
amounts of blood as well as small clots during the healing process. He should rest quietly and
continue drinking large amounts of fluid.
Cardiovascular
o What is the relationship of the kidneys to the cardiovascular system?
The kidneys filter about 1 L of blood per minute.
If cardiac output is decreased, the amount of blood going through the kidneys is decreased;
urinary output is decreased. Therefore, a decreased urinary output may be a sign of cardiac
problems.
When the kidneys produce and excrete 0.5 mL of urine/kg of body weight or average 30mL/hr output, the blood supply is considered to be minimally adequate to perfuse the vital
organs.
o Angina is caused by myocardial ischemia. Which cardiac medications would be appropriate for
acute angina?
Digoxin: not appropriate; increases the strength and contractility of the heart muscle; the
problem in angina is that the muscle is not receiving enough O2. Digoxin will not help.
Nitroglycerin: appropriate; causes dilatation of the coronary arteries, allowing more O2 to
get to the heart muscle.
Atropine: not appropriate; increases heart rate by blocking vagal stimulation, which
suppresses the heart rate; does not address the lack of O2 to the heart muscle.
Propranolol (Inderal): not appropriate for acute angina attack; however, is appropriate for
long-term management of stable angina because it acts as a beta blocker to control
vasoconstriction.
o Remember MONA when administering medications and treatments in the patient with myocardial
infarction. MONA: morphine, oxygen, nitroglycerin, aspirin.
o Blood pressure is created by the difference in the pressure of the blood as it leaves the heart and
the resistance it meets flowing out to the tissues. Therefore, any factor that alters cardiac output or
peripheral vascular resistance will alter blood pressure. Diet and exercise, smoking cessation,
weight control, and stress management can control many factors that influence the resistance blood
meets as it flows from the heart.
o Remember the risk factors for HTN: heredity, race, age, alcohol abuse, increased salt intake, obesity,
and use of oral contraceptives.
o The number one cause of a stroke in hypertensive clients is noncompliance with medication
regimen. HTN is often symptomless, and antihypertensive medications are expensive and have side
effects. Studies have shown that the more clients know about their antihypertensive medications,
the more likely they are to take them; teaching is important!
o Decreased blood flow results in diminished sensation in the lower extremities. Any heat source can
cause severe burns before the client realizes the damage is being done.
o A client is admitted with severe chest pain and states that he feels a terrible tearing sensation in his
chest. He is diagnosed with a dissecting aortic aneurysm. What assessments should the nurse
obtain in the first few hours?
Vital signs every hour
Neurologic vital signs
Respiratory status
Urinary output
Peripheral pulses
o During aortic aneurysm repair, the large arteries are clamped for a period of time, and kidney
damage can result. Monitor daily BUN and creatinine levels. Normal BUN is 10 to 20 mg/dL, and
normal creatinine is 0.6 to 1.2 mg/dL. The ratio of BUN to creatinine is 20:1. When this ratio
increases or decreases, suspect renal problems.
o Heparin prevents conversion of fibrinogen to fibrin and prothrombin to thrombin, thereby
inhibiting clot formation. Because the clotting mechanism is prolonged, do not cause tissue trauma,
which may lead to bleeding when giving heparin subcutaneously. Do not massage area or aspirate;
give in the abdomen between the pelvic bones, 2 inches from umbilicus; rotate sites.
o Anticoagulants
Heparin
Antagonist: protamine sulfate
Lab: PTT or aPTT determines efficacy
Keep 1.5 to 2.5 times normal control
Warfarin (Coumadin)
Antagonist: vitamin K
Lab: PT determines efficacy
Keep 1.5 to 2.5 times normal control
INR (international normalized ratio): desirable therapeutic level usually 2:3
(reflects how long it takes a blood sample to clot)o A Holter monitor offers continuous observation of the client’s heart rate. To make assessment of the
rhythm strips most meaningful, teach the client to keep a record of:
Medication times and doses
Chest pain episodes: type and duration
Valsalva maneuver (straining at stool, sneezing, coughing)
Sexual activity
Exercise and other activities
o Cardioversion is the delivery of synchronized electrical shocks to the myocardium.
o Difference in synchronous and asynchronous pacemakers:
Synchronous, or demand: Pacemaker fires only when the client’s heart rate falls below a
rate set on the generator.
Asynchronous, or fixed: Pacemaker fires at a constant rate.
o Restricting sodium reduces salt and water retention, thereby reducing vascular volume and
preload.
o Digitalis
Side effects of digitalis are increased when the client is hypokalemic.
Digitalis has a negative chronotropic effect (i.e., it slows the heart rate). Hold the digitalis if
the pulse rate is <60 or >120 bpm (<90 bpm in an infant) or has markedly changed rhythm.
Bradycardia, tachycardia, and dysrhythmias may be signs of digitalis toxicity; these signs
include nausea, vomiting, and headache in adults.
If withheld, consult with physician.
o Infective endocarditis damage to heart valves occurs with the growth of vegetative lesions on valve
leaflets. These lesions pose a risk for embolization, erosion, or perforation of the valve leaflets or
abscesses within adjacent myocardial tissue. Valvular stenosis or regurgitation (insufficiency), most
commonly of the mitral valve, can occur, depending on the type of damage inflicted by the lesions,
and can lead to symptoms of left- or right-sided heart failure.
o Pericarditis
The presence of a friction rub is an indication of pericarditis (inflammation of the lining of
the heart). ST-segment elevation and T-wave inversion are also signs of pericarditis.
o Acute and Subacute Infective Endocarditis
There are two types of infective endocarditis: acute, which often affects individuals with
previously normal hearts and healthy valves and carries a high mortality rate; and subacute,
which typically affects individuals with preexisting conditions, such as rheumatic heart
disease, mitral valve prolapse, or immunosuppression. Intravenous drug abusers are at risk
for both acute and subacute bacterial endocarditis. When this population develops subacute
infective endocarditis, the valves on the right side of the heart (tricuspid and pulmonic) are
typically affected because of the introduction of common pathogens that colonize the skin
(Staphylococcus epidermis or Candida sp.) into the venous system.
o In mitral valve stenosis, blood is regurgitated back into the left atrium from the left ventricle. In the
early period, there may be no symptoms, but as the disease progresses, the client will exhibit
excessive fatigue, dyspnea on exertion, orthopnea, dry cough, hemoptysis, or pulmonary edema.
There will be a rumbling apical diastolic murmur, and atrial fibrillation is common.
Gastrointestinal
o A Fowler or semi-Fowler position is beneficial in reducing the amount of regurgitation as well as in
preventing the encroachment of the stomach tissue upward through the opening in the diaphragm.
o Stress can cause or exacerbate ulcers. Teach stress-reduction methods, and encourage those with a
family history of ulcers to obtain medical surveillance for ulcer formation.
o Clinical manifestations of GI bleeding:
Pallor: conjunctival, mucous membranes, nail beds
Dark, tarry stools
Bright red or coffee-ground emesis
Abdominal mass or bruit
Decreased BP, rapid pulse, cool extremities (shock), increased respirations
o The GI tract usually accounts for only 100 to 200 mL of fluid loss per day, although it filters up to 8
L per day. Large fluid losses can occur if vomiting or diarrhea exists.o Opiate drugs tend to depress gastric motility. However, they should be given with caution, Nurse
should assess for abdominal distention; abdominal pain; abdominal rigidity; signs and symptoms of
shock-increased HR; decreased BP, indicating possible perforation/GI bleed.
o Diverticulosis is the presence of pouches in the wall of the intestine. There is usually no discomfort,
and the problem goes unnoticed unless seen on radiologic examination (usually prompted by some
other condition). Diverticulitis is an inflammation of the diverticula (pouches), which can lead to
perforation of the bowel.
o A client admitted with complaints of severe lower abdominal pain, cramping, and diarrhea is
diagnosed as having diverticulitis. What are the nutritional needs of this client throughout
recovery?
Acute phase: NPO, graduating to liquids
Recovery phase: no fiber or foods that irritate the bowel
Maintenance phase: high-fiber diet with bulk-forming laxatives to prevent pooling of foods
in the pouches where they can become inflamed; avoidance of small, poorly digested foods
such as popcorn, nuts, seeds, etc.
o Bowel Obstructions
Mechanical: Due to disorders outside the bowel (hernia, adhesions) caused by disorders
within the bowel (tumors, diverticulitis) or by blockage of the lumen in the intestine
(intussusception, gallstone)
Nonmechanical: Due to paralytic ileus, which does not involve any actual physical
obstruction but results from inability of the bowel itself to function
o A client admitted with complaints of constipation, thready stools, and rectal bleeding over the past
few months is diagnosed with a rectal mass. What are the nursing priorities for this client?
NPO
NG tube (possibly an intestinal tube such as a Miller-Abbott)
IV fluids
Surgical preparations of bowel (if obstruction is complete)
Foods and fluids are restricted for 8 to 10 hours before surgery if possible.
If the patient has a bowel obstruction or perforation, bowel cleansing is contraindicated.
Oral erythromycin and neomycin are given to further decrease the amount of colonic and
rectal bacteria.
If possible, all clients who require surgery for obstruction undergo NG intubation and
suction before surgery. However, in cases of complete obstruction, surgery should proceed
without delay
Teaching (preoperative nutrition, etc.)
o Diet recommended by the American Cancer Society to prevent bowel cancer:
Eat more cruciferous vegetables (those from the cabbage family, such as broccoli,
cauliflower, Brussels sprouts, cabbage, and kale).
Increase fiber intake.
Maintain average body weight.
Eat less animal fat.
o American Cancer Society recommendations for early detection of colon cancer:
A digital rectal examination (DRE) every year after 40.
A stool blood test every year after 50.
A colonoscopy or sigmoidoscopy examination every 10 years after the age of 50 in averagerisk clients, or more often based on the advice of a physician.
o An early sign of colon cancer is rectal bleeding. Encourage patients 50 years of age or older and
those with increased risk factors to be screened yearly with fecal occult blood testing. Routine
colonoscopy at 50 is also recommended.
o Clinical Manifestations of Jaundice
Yellow skin, sclera, or mucous membranes (bilirubin in skin)
Dark-colored urine (bilirubin in urine)
Chalky or clay-colored stools (absence of bilirubin in stools)
o Fetor hepaticus is a distinctive breath odor of chronic liver disease. It is characterized by a fruity or
musty odor that results from the damaged liver’s inability to metabolize and detoxify mercaptan,which is produced by the bacterial degradation of methionine, a sulfurous amino acid.
o For treatment of ascites, paracentesis and peritoneovenous shunts (LeVeen and Denver shunts)
may be indicated.
o Esophageal varices may rupture and cause hemorrhage. Immediate management includes insertion
of an esophagogastric balloon tamponade (a Blakemore-Sengstaken or Minnesota tube). Other
therapies include vasopressors, vitamin K, coagulation factors, and blood transfusions.
o Ammonia is not broken down as usual in the damaged liver; therefore, the serum ammonia level
rises.
o Damaged liver: the metabolism of drugs is slowed down so they remain in the system longer
(patient at risk for toxicity).
o Provide an Environment Conducive to Eating
For clients who are anorexic or nauseated:
Remove strong odors immediately; they can be offensive and increase nausea.
Encourage client to sit up for meals; this can decrease the propensity to vomit.
Serve small, frequent meals.
Give antiemetic prior to eating.
o Liver tissue is destroyed by hepatitis. Rest and adequate nutrition are necessary for regeneration of
the liver tissue being destroyed by the disease. Many drugs are metabolized in the liver, so drug
therapy must be scrutinized carefully. Caution the client that recovery takes many months, and
previously taken medications and/or over-the-counter drugs should not be resumed without the
health care provider’s directions.
o Acute pancreatic pain is located retroperitoneally. Any enlargement of the pancreas causes the
peritoneum to stretch tightly. Therefore, sitting up or leaning forward reduces the pain.
o Following an ERCP, the client may feel sick. The scope is placed in the gallbladder, and the stones
are crushed and left to pass on their own. These clients may be prone to pancreatitis.
o Nonsurgical management of a client with cholecystitis includes:
Low-fat diet
Medications for pain and clotting if required
Decompression of the stomach via NG tube
Endocrine
o Thyroid storm is a life-threatening event that occurs with uncontrolled hyperthyroidism due to
Graves disease. Other causes include childbirth, congestive heart failure (CHF), diabetic
ketoacidosis, infection, pulmonary embolism, emotional distress, trauma, and surgery. Symptoms
include fever, tachycardia, agitation, anxiety, and HTN. Primary nursing interventions include
maintaining an airway and adequate aeration.
o Propylthiouracil (PTU) and methimazole (Tapazole) are antithyroid drugs used to treat thyroid
storm. Propranolol (Inderal) may be given to decrease excessive sympathetic stimulation.
o Postoperative thyroidectomy: Be prepared for the possibility of laryngeal edema. Put a
tracheostomy set at the bedside along with O2 and a suction machine; calcium gluconate should be
easily accessible.
o Normal serum calcium is 9.0 to 10.5 mEq/L. The best indicator of parathyroid problems is a
decrease in the client’s calcium compared to the preoperative value.
o If two or more parathyroid glands have been removed, the chance of tetany increases dramatically:
Monitor serum calcium levels (9.0 to 10.5 mg/dL is normal range).
Check for tingling of toes and fingers and around the mouth.
Check Chvostek sign (twitching of lip after a tap over the parotid gland means it is positive).
Check Trousseau sign (carpopedal spasm after BP cuff is inflated above systolic pressure
means it is positive).
o Myxedema coma can be precipitated by acute illness, withdrawal of thyroid medication, anesthesia,
use of sedatives, or hypoventilation (with the potential for respiratory acidosis and CO2 narcosis).
The airway must be kept patent and ventilator support used as indicated.
o Many people take steroids for a variety of conditions. NCLEX-RN questions often focus on the need
to teach clients the importance of following the prescribed regimen precisely. They should be
cautioned against stopping the medications suddenly and should be informed that it is necessary to
taper off the dosage when taking steroids.o Addison crisis is a medical emergency. It is brought on by sudden withdrawal of steroids or a
stressful event (trauma, severe infection) or exposure to cold, overexertion, or decrease in salt
intake.
Vascular collapse: Hypotension and tachycardia occur; administer IV fluids at a rapid rate
until stabilized.
Hypoglycemia: Administer IV glucose.
Essential to reversing the crisis: Administer parenteral hydrocortisone.
Aldosterone replacement: Administer fludrocortisone acetate (Florinef) PO (available only
as oral preparation) with simultaneous administration of salt (sodium chloride) if client has
a sodium deficit.
o Teach clients to take steroids with meals to prevent gastric irritation. They should never skip doses.
If they have nausea or vomiting for more than 12 to 24 hours, they should contact the physician.
o Why do clients with diabetes have trouble with wound healing? High blood glucose contributes to
damage of the smallest vessels, the capillaries. This damage causes permanent capillary scarring,
which inhibits the normal activity of the capillary. This phenomenon causes disruption of capillary
elasticity and promotes problems such as diabetic retinopathy, poor healing of breaks in the skin,
and cardiovascular abnormalities.
o Glycosylated Hgb (HbA1c):
Indicates glucose control over previous 90-120 days (life of red blood cells [RBCs])
Is a valuable measurement of diabetes control
Informs diagnosis of diabetes and prediabetes
o The body’s response to illness and stress is to produce glucose. Therefore, any illness results in
hyperglycemia.
o If in doubt whether a client is hyperglycemic or hypoglycemic, treat for hypoglycemia.
o Self-monitoring of blood glucose (SMBG):
Uses techniques that are specific to each meter
Frequency of monitoring based on treatment regimen, change in meals, illness, and exercise
regimen
Requires recording results and reporting results to health care provider at time of visit
Results of monitoring used to assess the efficacy of therapy and to guide adjustments in
medical nutrition therapy, exercise, and medications to achieve the best possible blood
glucose control
o Insulin is prescribed in basal/bolus and correction factor therapy. The goal of insulin therapy is to
mimic the body’s normal basal/bolus secretion of insulin. Basal insulin (Long-acting and
intermediate-acting insulin) suppresses glucose production between meals and overnight. Bolus
insulin or mealtime limits hyperglycemia after meals. Correction factor is the amount of insulin
needed to correct hyperglycemia, usually given pre-meal.
Musculoskeletal
o A client comes to the clinic complaining of morning stiffness, weight loss, and swelling of both
hands and wrists. Rheumatoid arthritis is suspected. Which methods of assessment might the nurse
use, and which methods would the nurse not use? Use inspection, palpation, and strength testing.
Do not assess range of motion (ROM); this activity promotes pain because ROM is limited.
o In the joint, the normal cartilage becomes soft, fissures and pitting occur, and the cartilage thins.
Spurs form and inflammation sets in. The result is deformity marked by immobility, pain, and
muscle spasm. The prescribed treatment regimen is corticosteroids for the inflammation; splinting,
immobilization, and rest for the joint deformity; and NSAIDs for the pain.
o Synovial tissues line the bones of the joints. Inflammation of this lining causes destruction of tissue
and bone. Early detection of rheumatoid arthritis can decrease the amount of bone and joint
destruction. Often the disease goes into remission. Decreasing the amount of bone and joint
destruction reduces the amount of disability.
o What activity recommendations should the nurse provide a client with rheumatoid arthritis?
Do not exercise painful, swollen joints.
Do not exercise any joint to the point of pain.
Perform exercises slowly and smoothly; avoid jerky movements.
o NCLEX-RN questions often focus on the fact that avoiding sunlight is key in the management oflupus erythematosus; this is what differentiates it from other connective-tissue diseases.
o Postmenopausal, thin white women are at highest risk for development of osteoporosis. Encourage
exercise, a diet high in calcium, and supplemental calcium. Tums are an excellent source of calcium,
but they are also high in sodium, so hypertensive or edematous individuals should seek another
source of supplemental calcium.
o The main cause of fractures in older adults, especially in women, is osteoporosis. The main fracture
sites seem to be hip, vertebral bodies, and Colles fracture of the forearm.
o What type of fracture is more difficult to heal: an extracapsular fracture (below the neck of the
femur) or an intracapsular fracture (in the neck of the femur)?
The blood supply enters the femur below the neck of the femur. Therefore, an intracapsular
fracture heals with greater difficulty, and there is a greater likelihood that necrosis will
occur because the fracture is cut off from the blood supply.
o NCLEX-RN questions focus on safety precautions. Improper use of assistive devices can be very
risky. When using a nonwheeled walker, the client should lift and move the walker forward and
then take a step into it. The client should avoid scooting the walker or shuffling forward into it;
these movements take more energy and provide less stability than does a single movement.
o The risk for the development of a fat embolism, a syndrome in which fat globules migrate into the
bloodstream and combine with platelets to form emboli, is greatest in the first 36 hours after a
fracture. It is more common in clients with multiple fractures, fractures of long bones, and fractures
of the pelvis. The initial symptom of a fat embolism is confusion due to hypoxemia (check blood
gases for PO2). Assess for respiratory distress, restlessness, irritability, fever, and petechiae. If an
embolus is suspected, notify physician stat, draw blood gases, administer O2, and assist with
endotracheal intubation.
o In clients with hip fractures, thromboembolism is the most common complication. Prevention
includes passive ROM exercises, use of elastic stocking, elevation of the foot of the bed 25 degrees
to increase venous return, and low-dose heparin therapy.
o Clients with fractures, edema, or casts on the extremities need frequent neurovascular assessment
distal to the injury. Skin color, temperature, sensation, capillary refill, mobility, pain, and pulses
should be assessed.
o Assess the 5 Ps of neurovascular functioning: pain, paresthesia, pulse, pallor, and paralysis.
o Orthopedic wounds have a tendency to ooze more than other wounds. A suction drainage device
usually accompanies the client to the postoperative floor. Check drainage often.
o NCLEX-RN questions about joint replacement focus on complications. A big problem after joint
replacement is infection.
o Fractures of bone predispose the client to anemia, especially if long bones are involved. Check
hematocrit every 3 to 4 days to monitor erythropoiesis.
o After hip replacement, instruct the client not to lift the leg upward from a lying position or to
elevate the knee when sitting. This upward motion can pop the prosthesis out of the socket.
o Immobile clients are prone to complications: skin integrity problems, formation of urinary calculi
(client’s milk intake may be limited), and venous thrombosis (client may be on prophylactic
anticoagulants).
o The residual limb (stump) should be elevated on one pillow. If the residual limb (stump) is elevated
too high, the elevation can cause a contracture.
Neurosensory
o Glaucoma is often painless and symptom-free. It is usually picked up as part of a regular eye
examination.
o Eye drops are used to cause pupil constriction because movement of the muscles to constrict the
pupil also allows aqueous humor to flow out, thereby decreasing the pressure in the eye.
Pilocarpine is commonly used. Caution client that vision may be blurred for 1 to 2 hours after
administration of pilocarpine and that adaptation to dark environments is difficult because of
pupillary constriction (the desired effect of the drug)
o There is an increased incidence of glaucoma in older adult populations. Older clients are prone to
problems associated with constipation. Therefore, the nurse should assess these clients for
constipation and postoperative complications associated with constipation and should implement a
plan of care directed at prevention of and, if necessary, treatment for constipation.o The lens of the eye is responsible for projecting light onto the retina so that images can be
discerned. Without the lens, which becomes opaque with cataracts, light cannot be filtered and
vision is blurred.
o When the cataract is removed, the lens is gone, making prevention of falls important. When the lens
is replaced with an implant, vision is better.
o The ear consists of three parts: the external ear, the middle ear, and the inner ear. Inner ear
disorders, or disorders of the sensory fibers going to the CNS, often are neurogenic in nature and
may not be helped with a hearing aid. External and middle ear problems (conductive) may result
from infection, trauma, or wax buildup. These types of disorders are treated more successfully with
hearing aids.
o NCLEX-RN questions often focus on communicating with older adults who are hearing impaired.
Speak in a low-pitched voice, slowly and distinctly.
Stand in front of the person, with the light source behind the client.
Use visual aids if available.
o Use of the Glasgow Coma Scale eliminates ambiguous terms to describe neurologic status, such as
lethargic, stuporous, or obtunded.
o Almost every diagnosis in the NANDA format is applicable because severely neurologically
impaired persons require total care.
o Unconscious Client
Gastric Gavage
Check bowel sounds, and begin feeding when GI peristalsis returns.
Place client in high-Fowler position.
Place towel over chest.
Check gastric tube placement.
Connect gastrostomy tube to funnel or large syringe.
Check gastric residual to assess absorption and client tolerance; return residual.
Pour feeding into tilted funnel, and unclamp tubing to allow feeding to flow by
gravity.
Regulate flow by raising or lowering container. Feeding too quickly causes diarrhea,
gastric distention, pain. Feeding too slowly causes possible obstruction of flow.
After feeding, irrigate tube with (tepid) water and clamp tube.
Apply small dressing over tube opening; coil tube and attach to dressing. May cover
with an abdominal binder.
Keep HOB elevated 30 degrees or more during feeding and for at least one hour
after feeding.
Bowel Management Program
Get bowel history from reliable source.
Establish specific time for evacuation. Regularity is essential.
An unconscious client can evacuate the bowel after the last tube feeding of day,
because the gastrocolic and duodenocolic reflexes are active after “meal.”
Stimulate anorectal reflex by insertion of glycerin suppository 15 to 30 minutes
before scheduled evacuation time. May need stronger suppository, such as bisacodyl
(Dulcolax).
Ensure adequate fiber in tube feedings and adequate fluid intake of 2 to 4 L/day.
May apply a rectal pouch to contain fecal material (ostomy bag with seal over anal
opening).
o A client with an altered state of consciousness is fed via enteral routes because the likelihood of
aspiration is high with oral feedings. Residual feeding is the amount of previous feeding still in the
stomach. The presence of 100 mL of residual in an adult usually indicates poor gastric emptying,
and the feeding should be withheld.
o Paralytic ileus is common in comatose clients. A gastric tube aids in gastric decompression.
o Any client on bed rest or immobilized must have ROM exercises often and very frequent position
changes. Do not leave the client in any one position for longer than 2 hours. Any position that
decreases venous return, such as sitting with dependent extremities for long periods, is dangerous.
o If temperature elevates, take quick measures to decrease it, because fever increases cerebralmetabolism and can increase cerebral edema.
o Safety features for immobilized clients:
Prevent skin breakdown by frequent turning.
Maintain adequate nutrition.
Prevent aspiration with slow, small feedings or NG feedings.
Monitor neurologic signs to detect the first signs that ICP may be increasing.
Provide ROM exercises to prevent deformities.
Prevent respiratory complications; frequent turning and positioning provide optimal
drainage.
o Restlessness may indicate a return to consciousness but can also indicate anoxia, distended
bladder, covert bleeding, or increasing cerebral anoxia. Do not oversedate, and report any
symptoms of restlessness.
o The forces of impact influence the type of head injury. They include acceleration injury, which is
caused by the head being in motion, and deceleration injury, which occurs when the head stops
suddenly. Helmets are a great preventive measure for motorcyclists and bicyclist
o Even subtle behavior changes, such as restlessness, irritability, or confusion, may indicate increased
ICP.
o CSF leakage carries the risk for meningitis and indicates a deteriorating condition. Because of CSF
leakage, the usual signs of increased ICP may not occur.
o With head injury patients try not to use restraints; they only increase restlessness. Avoid
narcotics because they mask the level of responsiveness.
o Physical assessment should concentrate on respiratory status, especially in clients with injury at C3
to C5, because the cervical plexus innervates the diaphragm.
o It is imperative to reverse spinal shock as quickly as possible. Permanent paralysis can occur if a
spinal cord is compressed for 12 to 24 hours.
o A common cause of death after spinal cord injury is urinary tract infection. Bacteria grow best in
alkaline media, so keeping urine dilute and acidic is prophylactic against infection. Also, keeping the
bladder emptied assists in avoiding bacterial growth in urine that has stagnated in the bladder.
o Benign tumors continue to grow and take up space in the confined area of the cranium, causing
neural and vascular compromise in the brain, increased ICP, and necrosis of brain tissue. Even
benign tumors must be treated because they may have malignant effects.
o Craniotomy preoperative medications:
Corticosteroids to reduce swelling
Agents and osmotic diuretics to reduce secretions (atropine, glycopyrrolate [Robinul])
Agents to reduce seizures (phenytoin)
Prophylactic antibiotics
o Symptoms involving motor function usually begin in the upper extremities with weakness
progressing to spastic paralysis. Bowel and bladder dysfunction occurs in 90% of cases. MS is more
common in women. Progression is not “orderly.”
o Drug therapy for MS clients: ACTH, cortisone, cyclophosphamide (Cytoxan), and other
immunosuppressive drugs. Nursing implications for administration of these drugs should focus on
the prevention of infection.
o In clients with myasthenia gravis, be alert for changes in respiratory status; the most severe
involvement may result in respiratory failure.
o Bed rest often relieves symptoms. Bladder and respiratory infections are often a recurring problem.
There is a need for health-promotion teachings.
o Myasthenic crisis is associated with a positive edrophonium (Tensilon) test, whereas a cholinergic
crisis is associated with a negative test.
o NCLEX-RN questions often focus on the features of Parkinson disease: tremors (a coarse tremor of
fingers and thumb on one hand that disappears during sleep and purposeful activity; also called
“pill rolling”), rigidity, hypertonicity, and stooped posture. Focus: safety!
o An important aspect of treatment for Parkinson disease is drug therapy. The pathophysiology
involves an imbalance between acetylcholine and dopamine, so symptoms can be controlled by
administering a dopamine precursor (levodopa).
o CNS involvement related to cause of stroke: Hemorrhagic: Caused by a slow or fast hemorrhage into the brain tissue; often related to
HTN
Embolic: Caused by a clot that has broken away from a vessel and has lodged in one of the
arteries of the brain, blocking the blood supply. It is often related to atherosclerosis (so it
may occur again).
o Atrial flutter and fibrillation produce a high incidence of thrombus formation following
dysrhythmia caused by turbulence of blood flow through all valves and heart chambers.
o A woman who had a stroke 2 days earlier has left-sided paralysis. She has begun to regain some
movement in her left side. What can the nurse tell the family about the client’s recovery period?
“The quicker movement is recovered, the better the prognosis is for full or improved recovery. She
will need patience and understanding from her family as she tries to cope with the stroke. Mood
swings can be expected during the recovery period, and bouts of depression and tearfulness are
likely.”
o Words that describe losses in strokes:
Apraxia: inability to perform purposeful movements in the absence of motor problems
Dysarthria: difficulty articulating
Dysphasia: impairment of speech and verbal comprehension
Aphasia: loss of the ability to speak
Agraphia: loss of the ability to write
Alexia: loss of the ability to read
Dysphagia: dysfunctional swallowing
o Steroids are administered after a stroke to decrease cerebral edema and retard permanent
disability. H2 inhibitors are administered to prevent peptic ulcers.
Hematology and Oncology
o Physical symptoms occur as a compensatory mechanism when the body is trying to make up for a
deficit somewhere in the system. For instance, cardiac output increases when Hgb levels drop
below 7 g/dL.
o Administration of Iron
Do’s
Use Z-track method of administration.
Use air bubble to avoid withdrawing medication into subcutaneous tissue.
Don'ts
Do not use deltoid muscle.
Do not massage injection site.
o Use only normal saline to flush IV tubing or to run with blood. Never add medications to blood
products. Two registered nurses should simultaneously check the physician’s prescription, the
client’s identity, and the blood bag label.
o Administration of Antineoplastic Chemotherapeutic Agents
Follow OSHA guidelines for administration as well as for decontamination of nondisposable
areas and equipment and of self.
Obtain complete and detailed instructions about administration (routine knowledge of
procedures for IV administration is not sufficient).
These drugs are toxic to cancer cells and normal cells in both the client and the caregivers
who are infusing the drugs.
Nurses who are pregnant or are considering becoming pregnant should notify supervisor
(many agencies discourage or prohibit such caregivers from administering these drugs).
Wear gloves when handling drugs.
Check the drug with another nurse against the health care provider’s prescription and the
client’s record to ensure that it is the correct medication.
If IV catheter line is used for infusion, verify line placement and patency with another nurse
and aspirate a blood return.
If a vesicant (caustic) drug is administered peripherally, stay with the client throughout
administration and check IV placement and patency frequently by aspirating a blood return.
If a peripheral site is used for infusion, use a new site daily.
Dispose of all IV equipment in the specially provided waste receptacle so that personnelhandling trash do not come into contact with vesicant drugs.
o Many health care delivery systems require the nurse to be credentialed in order to administer
parental chemotherapy. The practical nurse (PN) should recognize complications of chemotherapy
related to administration, safety, side effects, and nursing assessment parameters and should
report these to the registered nurse and health care provider.
o A 24-year-old is admitted with large areas of ecchymosis on both upper and lower extremities. She
is diagnosed with acute myelogenous leukemia. What are the expected laboratory findings for this
client, and what is the expected treatment?
Lab: Decreased Hgb, decreased Hct, decreased platelet count, altered WBC (usually quite
high)
Treatment: Prevention of infection; prevention and control of bleeding; high-protein, highcalorie diet; assistance with ADL; drug therapy
o Infection in the immunosuppressed person may not be manifested with an elevated temperature.
Therefore, it is imperative that the nurse perform a total and thorough assessment of the client
frequently.
o Use and Care of IV Lines and Catheters (Central Lines, PICC lines)
Stays in place for extended periods of time
Used for clients who require immunosuppressive therapy or are receiving long-term IV
therapy
Exit sites include:
At the upper chest
Femoral area
Antecubital area
To prevent an air embolus when a central line is open to air, position client in
Trendelenburg position or have client perform a Valsalva maneuver if there is no slide
clamp on the line.
Maintain a patent IV site by flushing with heparin or saline. (The amount of heparin used
depends on size of lumen, length of tubing, whether reservoir exists [e.g., Port-A-Cath].)
Immediately after insertion of a central line, the nurse should auscultate breath sounds.
After insertion of a central line, a chest radiograph must be taken to determine correct
placement and detect pneumothorax (observe for unequal expansion of chest wall).
o Most oncologic drugs cause immunosuppression. Prevention of secondary infections is vital! Advise
client to stay away from persons with known infections such as colds. In the hospital, place client in
a private room, and maintain an environment as sterile and as clean as possible. These persons
should not eat raw vegetables or fruits—only cooked foods—so as to destroy any bacteria.
o Hodgkin disease is one of the most curable of all adult malignancies. Emotional support is vital.
Career development is often interrupted for treatment. Chemotherapy renders many male clients
sterile. May bank sperm prior to treatment, if desired.
Reproductive
o Menorrhagia (profuse or prolonged menstrual bleeding) is the most important factor relating to
benign uterine tumors. Assess for signs of anemia.
o What is the anatomic significance of a prolapsed uterus? When the uterus is displaced, it impinges
on other structures in the lower abdomen. The bladder, rectum, and small intestine can protrude
through the vaginal wall.
o Laser therapy or cryosurgery is used to treat cervical cancer when the lesion is small and localized.
Invasive cancer is treated with radiation, conization, hysterectomy, or pelvic exenteration (a drastic
surgical procedure where the uterus, ovaries, fallopian tubes, vagina, rectum, and bladder are
removed in an attempt to stop metastasis). Chemotherapy is not useful for this type of cancer.
o American College of Obstetricians and Gynecologists (ACOG) 2009 recommendations: Pap smears
should begin at age 21 and women younger than 30 should be screened every 2 years; women 30
and older may be screened every 3 years after they have had three consecutive negative cervical
cytology tests. Women ages 65 to 70 may stop Pap smears if they have three consecutive normal
tests in a row and no abnormal Pap smears in the last 10 years. Women with high risk factors may
need more frequent screenings.
o The major emphasis in nursing management of cancers of the reproductive tract is early detection.o The importance of teaching female clients how to conduct a breast self-examination cannot be
overemphasized. Early detection is related to positive outcomes.
o The presence or absence of hormone receptors is paramount in selecting clients for adjuvant
therapy.
o Men whose testes have not descended into the scrotum or whose testes descended after age 6 are
at high risk for developing testicular cancer. The most common symptom is the appearance of a
small, hard lump about the size of a pea on the front or side of the testicle. Testicular selfexamination (TSE) should be done regularly at the same time every month by all males after age 14.
It should be done after a shower by gently palpating the testes and cord to look for a small lump.
Swelling may also be a sign of testicular cancer.
o STDs in infants and children usually indicate sexual abuse and should be reported. The nurse is
legally responsible to report suspected cases of child abuse.
o Chlamydia is the most commonly reported communicable disease in the United States.
o Pelvic inflammatory disease (PID) involves one or more of the pelvic structures. The infection can
cause adhesions and eventually result in sterility. Manage the pain associated with PID with
analgesics and warm sitz baths. Bed rest in a semi-Fowler position may increase comfort and
promote drainage. Antibiotic treatment is necessary to reduce inflammation and pain.
o A client comes into the clinic with a chancre on his penis. What is the usual treatment? IM dose of
penicillin (such as benzathine penicillin G, 2.4 million units). Obtain a sexual history, including the
names of his sex partners, so that they can receive treatment.
Burns
o ABCs of Assessment
Airway
Breathing
Circulation
o Massive volumes of IV fluids are given. It is not uncommon to give over 1000 mL/hr during various
phases of burn care. Hemodynamic monitoring must be closely observed to be sure the client is
supported with fluids but is not overloaded.
o Infection is a life-threatening risk for those with burns.
o Dressing changes are very painful! Medicate client prior to procedure!
o Preexisting conditions that might influence burn recovery are age, chronic illness (diabetes, cardiac
problems, etc.), physical disabilities, disease, medications used routinely, and drug or alcohol abuse.
o Severity of Burns
Superficial partial-thickness, first degree: pink to red skin (e.g., sunburn), slight edema, and
pain relieved by cooling
Deep partial-thickness, second degree: destruction of epidermis and upper layers of dermis;
white or red, very edematous, sensitive to touch and cold air, hair does not pull out easily
Full-thickness, third degree: total destruction of dermis and epidermis; reddened areas do
not blanch with pressure; not painful; inelastic; waxy white skin to brown, leathery eschar
o Stages of Burns
Stage I (emergent phase): Replacement of fluids is titrated to urine output.
Stage II (acute phase): Patent infusion site is maintained in case supplemental IV fluids are
needed; saline lock is helpful; colloids may be used.
Stage III (rehabilitation phase): No extra fluids are needed, but high-protein drinks are
recommended.
o Pain Management in Burn Patient
Administer pain medication, especially prior to dressing wound. Teach distraction and
relaxation techniques. Teach use of guided imagery.
o On admission of burn patient Provide a patent airway because intubation may be necessary.
Determine baseline data. Initiate fluid and electrolyte therapy. Administer pain medication.
Determine depth and extent of burn. Administer tetanus toxoid. Insert NG tube.
o Nutrition in burn patient
High-calorie, high-protein, high-carbohydrate diet; medications with juice or milk; no “free”
water; tube feeding at night. Maintain accurate, daily calorie counts. Weigh client daily.
o Methods of Extinguishing Thermal: Remove clothing, immerse in tepid water.
Chemical: Flush with water or saline (unless dry chemical DO NOT FLUSH, pat/wipe off).
Electrical: Separate client from electrical source.
o Signs of Inhalation Burn Singed nasal hairs, circumoral burns; sooty or bloody sputum,
hoarseness, and pulmonary signs, including asymmetry of respirations, rales, or wheezing
o Autograft = using client’s own skin for grafts
o No “free” water in burned patient Water may interfere with electrolyte balance. Client needs to
ingest food products with highest biologic value.
Pediatric
Growth and Development
o Theories of Growth and Development
Erikson: 8 Stages of Psychosocial Development: Trust vs. Mistrust, Autonomy vs. Shame
and Doubt, Initiative vs. Guilt, Industry vs. Inferiority, Identity vs. Role Confusion, Intimacy
vs. Isolation, Generativity vs. Stagnation, and Integrity vs. Despair.
Piaget: 4 Stages of Cognitive Development: Sensorimotor Period, Preoperational Thought,
Concrete Operation, and Formal Operation.
Kohlberg Moral Development: Naiveté and Egocentrism, Punishment-Obedience
Orientation, Instrumental Hedonism and Concrete Reciprocity, Good Boy or Good Girl
Orientation, Law and Order Orientation, Social Contract Orientation, Personal Principle
Orientation, Universal Principle Orientation.
o Frequently tested content areas on the NCLEX-RN® examination:
When does birth length double? Answer: by 4 years.
When does the child sit unsupported? Answer: 8 months.
When does a child achieve 50% of adult height? Answer: 2 years.
When does a child throw a ball overhand? Answer: 18 months.
When does a child speak two- to three-word sentences? Answer: 2 years.
When does a child use scissors? Answer: 4 years.
When does a child tie his or her shoes? Answer: 5 years.
Be aware that a girl’s growth spurt during adolescence begins earlier than a boy’s (as early
as 10 years of age).
Temper tantrums are common in the toddler (i.e., they are considered normal or average
behavior).
Be aware that adolescence is a time when the child forms his or her identity and that
rebellion against family values is common for this age group.
o Knowledge of normal growth and development is used to evaluate interventions and therapy. For
example, what behavior would indicate that thyroid hormone therapy for a 4-month-old is
effective? You must know which milestones are accomplished by a 4-month-old. One correct
answer would be: Has steady head control, which is an expected milestone for a 4-month-old and
indicates that replacement therapy is adequate for growth.
o Use facts and principles related to growth and development in planning teaching interventions. For
example: What task could a 5-year-old boy with diabetes expect to accomplish by himself? One
correct answer would be to let him choose the injection sites. This is possible for a preschooler to
do and gives the child some sense of control.
o School-age children are in Erikson’s stage of industry, meaning they like to do and accomplish
things. Peers are also becoming important for children of this age.
o Tanner Stages of Pubertal Development
Girls: Breast changes, Rapid increase in height and weight, Growth of pubic hair,
Appearance of axillary hair, Menstruation, Abrupt deceleration of linear growth.
Boys: Enlargement of testicles, Growth of pubic hair, axillary hair, facial hair and body hair,
Rapid increase in height, Changes in larynx and voice, Nocturnal emissions, Abrupt
deceleration of linear growth.
o Age groups’ concepts of bodily injury:
Infants: After 6 months, their cognitive development allows them to remember pain. Toddlers: They fear intrusive procedures.
Preschoolers: They fear body mutilation.
School-age children: They fear loss of control of their bodies.
Adolescents: Their major concern is change in body image.
o Accidents are a major cause of death in children and adolescents. Teach parents and children
developmentally appropriate safety and accident-prevention techniques.
Pain Assessment
o Children as young as 3 years of age are able to report the location and degree of pain they are
experiencing.
o Observe for nonverbal signs of pain, such as grimacing, irritability, restlessness, and difficulty in
sleeping or feeding.
o A pain rating scale appropriate for the child’s age and developmental level should be used.
CRIES can be used with infants 32 to 60 weeks of gestational age.
Pain Rating Scale (PRS) can be used with children 1 to 36 months of age.
FACES Pain Rating Scale and the Poker Chip Scale can be used by children of preschool age
and older.
Numeric Pain Scale can be used by children 9 years of age and older.
The Oucher Pain Scale is a scale used for children 3 to 12 years of age with culturally
specific photographs showing different levels of pain and discomfort.
Documentation of a child’s self-report of pain is essential to effectively treating the child’s
pain.
A nonverbal child can be assessed using the FLACC pain assessment tool. This tool has the
nurse evaluate the child’s facial expression, leg movement, activity, cry, and consolability.
Health Promotion
o Pertinent history should be obtained prior to administering certain immunizations because
reactions to previous immunizations or current health conditions may contraindicate current
immunizations:
DTaP: History of reactions, seizures, neurologic symptoms after previous vaccine, or
systematic allergic reactions
MMR: History of anaphylactic reaction to eggs or neomycin
o Subcutaneous injection, rather than intradermal injection, invalidates the Mantoux test.
o The common cold is not a contraindication for immunization.
o Following immunization, what teaching should the nurse provide to the parents?
Irritability, fever (<102° F), redness, and soreness at injection site for 2 to 3 days are normal
side effects of DTaP and IPV administration.
Call health care provider if seizures, high fever, or high-pitched crying occurs.
A warm washcloth on the thigh injection site and “bicycling” the legs with each diaper
change decreases soreness.
Acetaminophen (Tylenol) is administered orally every 4 to 6 hours (10 to 15 mg/kg).
o Pertussis fatalities continue to occur in nonimmunized infants in the United States.
o Contraindications to live virus immunization immunocompromised child or child is living with
an immunocompromised individual
o S&S of Iron Deficiency: Anemia; pale conjunctiva; pale skin color; atrophy of papillae on tongue;
brittle, ridged, or spoon-shaped nails; and thyroid edema
Communicable Diseases of Childhood
o Children with German measles pose a serious threat to their unborn siblings. The nurse should
counsel all expectant mothers, especially those with young children, to be aware of the serious
consequences of exposure to German measles during pregnancy.
o Classic S&S of Measles: Photophobia, confluent rash that begins on the face and spreads downward,
and Koplik spots on the buccal mucosa
o Common childhood problems are encountered by nurses caring for children in the community or
hospital settings. The child’s age directly influences the severity and management of these
problems.
o Pediculosis is an infestation of lice on humans. The most common form is head lice, which affects
the scalp and hair. Head lice appear as small white flakes along the shaft of the hair. Treatment isdirected toward killing the adult lice, combing out the nits and using a hair product containing
permethrin or pyrethrin. Anything that is in direct contact with the infestation has to be treated to
decrease spread of the lice.
Diarrhea
o Add potassium to IV fluids only with adequate urine output.
o Teach home care of child with diarrhea:
Provide child with oral rehydration solution such as Pedialyte or Lytren.
Child may temporarily need lactose-free diet.
Children should not receive antidiarrheals (e.g., Imodium A-D).
Do not give child grape juice, orange juice, apple juice, cola, or ginger ale. These solutions
have high osmolality.
o S&S of dehydration: Poor skin turgor, absence of tears, dry mucous membranes, weight loss,
depressed fontanel, and decreased urinary output
o Lab findings with dehydration: Loss of bicarbonate/decreased serum pH, loss of sodium
(hyponatremia), loss of potassium (hypokalemia), elevated Hct, and elevated BUN
Burns
o In childhood, a partial-thickness burn is considered a major burn if it involves more than 25% of
body surface.
o A full-thickness burn is considered major if it involves more than 10% of body surface.
o Assess burns in children by using the Lund-Browder chart, which takes into account the changing
proportions of the child’s body
o Fluid needs should be calculated from the time of the burn.
o Adequacy of fluid replacement is determined by evaluating urinary output.
Urinary output for infants and children should be 1 to 2 mL/kg/hr.
Specific gravity should be less than 1.025.
Poisonings
o Use of syrup of ipecac is no longer recommended by the American Academy of Pediatrics. Teach
parents that it is not recommended to induce vomiting in any way because it may cause more
damage.
o More lead is absorbed on an empty stomach. Hot water can contain higher levels of lead because it
dissolves lead more quickly than cold water, so use only cold water for consumption (drinking,
cooking, and especially for making infant formula).
o Child proof the home teach to lock all cabinets, to safely store all toxic household items in locked
cabinets, and to examine the house from the child’s point of view
o With a child who has ingested a poison the nurse should FIRST assess the child’s respiratory,
cardiac, and neurologic status
o Early S&S of Lead Poisoning Anemia, acute cramping, abdominal pain, vomiting, constipation,
anorexia, headache, lethargy, hyperactivity, aggression, impulsiveness, decreased interest in play,
irritability, short attention span
Respiratory Disorders
o When calculating a pediatric dosage, the nurse must often change the child’s weight from pounds to
kilograms.
2.2 lb = 1 kg (divide pounds by 2.2).
If the child’s weight is in pounds, convert the pounds directly to kilograms.
If the child’s weight is in pounds and ounces, convert the ounces to the nearest tenth
of a pound and add this to the total pounds. Then convert the total pounds to
kilograms to the nearest tenth.
Weight expressed in kilograms should always be a smaller number than the weight
expressed in pounds.
o Respiratory Client
Administration of Oxygen
Oxygen hood: Used for infants.
Nasal prongs: Provide low to moderate concentrations of oxygen.
Tents: Provide mist and oxygen. Monitor child’s temperature. Keep edges tucked in.
Keep child dry. Measurement of Oxygenation
Pulse oximetry measures oxygen saturation (SaO2) of arterial hemoglobin
noninvasively via a sensor that is usually attached to the finger or toe or, in an
infant, to sole of foot.
Nurse should be aware of the alarm parameters signaling decreased SaO2 (usually
<95%).
Blood gas evaluation is usually monitored in respiratory clients through arterial
sampling.
Norms: PO2: 80 to 100 mm Hg; PCO2: 35 to 45 mm Hg for children (not infants and
newborns)
o With Cystic Fibrosisc Teach dietary recommendations: pancreatic enzyme replacement, fatsoluble vitamins, high in calories, high in protein, moderate to high in fat (more calories per
volume), and moderate to low in carbohydrates (to avoid an increase in CO2 drive).
A child needs 150% of the usual calorie intake for normal growth and development.
o Do not examine the throat of a child with epiglottitis (i.e., do not put a tongue blade or any object
into the throat) because of the risk of obstructing the airway completely.
o In planning and providing nursing care, a patent airway is always the priority of care, regardless of
age!
o Respiratory disorders are the primary reason most children and their families seek medical care.
Therefore, these disorders are frequently tested on the NCLEX-RN. Knowing the normal parameters
of respiratory rates and the key signs of respiratory distress in children is essential!
o The nurse should be sure prothrombin time (PT) and partial thromboplastin time (PTT) have been
determined prior to a tonsillectomy. More important, the nurse should ask whether there has been
a history of bleeding, prolonged or excessive, and whether there is a history of any bleeding
disorders in the family.
o Child with asthma Expiratory wheezing, rales, tight cough, and signs of altered blood gases
o S&S of Respiratory Distress: Restlessness, tachycardia, tachypnea, diaphoresis, flaring nostrils,
retractions, and grunting
o Care of child in a mist tent: Monitor child’s temperature, keep tent edges tucked in, keep clothing
dry, assess respiratory status, look at child inside tent.
o A child with epiglottis you will see them sitting upright, with chin out and tongue protruding
(“tripod position”)
o Post-op tonsillectomy complications: Hemorrhage; frequent swallowing, vomiting fresh blood, and
clearing throat
Cardiovascular
o Polycythemia is common in children with cyanotic defects.
o The heart rate of a child increases with crying or fever.
o Infants may require tube feeding to conserve energy. Infants being tube-fed need to continue to
satisfy sucking needs.
o Basic differences between cyanotic and acyanotic defects:
Acyanotic: Has abnormal circulation; however, all blood entering the systemic circulation is
oxygenated.
Congestive heart failure is more often associated with acyanotic defects.
Cyanotic: Has abnormal circulation with unoxygenated blood entering the systemic
circulation.
o Tetralogy of Fallot (acyanotic defect)
Will see: VSD, overriding aorta, pulmonary stenosis, and right ventricular hypertrophy
Position during TET spell: knee-to-chest or squatting (**DO THIS FIRST)
o CHF is a common complication of congenital heart disease. It reflects the increased workload of the
heart caused by shunts or obstructions. The two objectives in treating CHF are to reduce the
workload of the heart and increase cardiac output.
o Managing Digoxin
Administration
Prior to administering digoxin, nurse must take child’s apical pulse for 1 minute to
assess for bradycardia. Hold dose if pulse is below normal heart rate for child’s age. Therapeutic blood levels of digoxin are 0.8 to 2.0 ng/mL (nanograms per milliliter).
Families should be taught safe home administration of digoxin:
o Administer on a regular basis; do not skip or make up for missed doses.
o Give 1 hour before or 2 hours after meals. Do not mix with formula or food.
o Take child’s pulse prior to administration, and know when to call the
caregiver.
o Keep in safe place (e.g., a locked cabinet).
Toxicity
Nurse must be acutely aware of the signs of digoxin toxicity. A small child or infant
cannot describe feeling bad or nauseated.
o Common S&S of toxicity: Diarrhea, fatigue, weakness, nausea, and vomiting;
the nurse should check for bradycardia prior to administration.
Vomiting is a common early sign of toxicity. This symptom is often overlooked
because infants commonly “spit up.”
Other GI symptoms include anorexia, diarrhea, and abdominal pain.
Neurologic signs include fatigue, muscle weakness, and drowsiness.
Hypokalemia can increase digoxin toxicity.
o When frequent weighings are required, weigh client on the same scale at the same time of day so
that accurate comparisons can be made.
o Nursing interventions to reduce the workload of the heart Give small, frequent feedings or
gavage feedings. Plan frequent rest periods. Maintain a neutral thermal environment. Organize
activities to disturb child only as indicated.
o Risks of cardiac catheterization: arrhythmia, bleeding, perforation, phlebitis, and obstruction of the
arterial entry site
o Rheumatic Fever
Cardiac complications associated with rheumatic fever: aortic and mitral valve stenosis
Tx: penicillin, erythromycin, and aspirin
Neuromuscular Disorders
o The nursing goal in caring for a child with Down syndrome is to help the child reach his or her
optimal level of functioning.
o Feed infant or child with cerebral palsy using nursing interventions aimed at preventing aspiration.
Position child upright, and support the lower jaw.
o Spina Bifida: keep infant in prone position; protect the sac with moist, sterile dressing
o Hydrocephalus (commonly associated with Spina Bifida)
The signs of increased intracranial pressure (ICP) are the opposite of those of shock:
Shock: increased pulse, decreased blood pressure
Increased ICP: decreased pulse, increased blood pressure
Baseline data on the child’s usual behavior and level of development are essential so
changes associated with increased ICP can be detected early.
Do not pump shunt unless specifically prescribed. The shunt is made up of delicate valves,
and pumping changes the pressures within the ventricles.
o Medication noncompliance is the most common cause of increased seizure activity
o Do not use tongue blade, padded or not, during a seizure. It can cause traumatic damage to oral
cavity.
o Monitor hydration status and IV therapy carefully. With meningitis, there may be inappropriate
ADH secretions causing fluid retention (cerebral edema) and dilutional hyponatremia.
o Headache on awakening is the most common presenting symptom of brain tumors.
o Most postoperative clients with infratentorial tumors are prescribed to lie flat or turn to either side.
A large tumor may require that the child not be turned to the operative side.
o Suctioning, coughing, straining, and turning cause increased ICP.
o What are the physical features of a child with Down syndrome?
Simian creases in palms, hypotonia, protruding tongue, and upward-outward slant of eyes
o Describe scissoring.
A common characteristic of spastic cerebral palsy in infants; legs are extended and crossed
over each other, feet are plantar flexedo What are two nursing priorities for a newborn with myelomeningocele?
Prevention of infection of the sac and monitoring for hydrocephalus (measure head
circumference, check fontanel, assess neurologic functioning)
o List the signs and symptoms of increased ICP in older children.
Irritability, change in LOC, motor dysfunction, headache, vomiting, unequal pupil response,
and seizures
o What teaching should parents of a newly shunted child receive?
Information about signs of infection and increased ICP; understanding that shunt should not
be pumped and that child will need revisions with growth; guidance concerning growth and
development
o State the three main goals in providing nursing care for a child experiencing a seizure.
Maintain patent airway, protect from injury, and observe carefully.
o What are the side effects of Dilantin?
Gingival hyperplasia, dermatitis, ataxia, GI distress
o Describe the signs and symptoms of a child with meningitis.
Fever, irritability, vomiting, neck stiffness, opisthotonos, positive Kernig sign, positive
Brudzinski sign; infant may not show all classic signs even though very ill
o What antibiotics are usually prescribed for bacterial meningitis?
Ampicillin, ceftriaxone, or chloramphenicol
o How is a child usually positioned after brain tumor surgery?
Flat or on either side
o Describe the function of an osmotic diuretic.
Osmotic diuretics remove water from the CNS to reduce cerebral edema.
o What nursing interventions increase intracranial pressure?
Suctioning and positioning, turning
o Describe the mechanism of inheritance of Duchenne muscular dystrophy.
Duchenne muscular dystrophy is inherited as an X-linked recessive trait.
o What is the Gowers sign?
Gowers sign is an indicator of muscular dystrophy; to stand, the child has to “walk” hands
up legs.
Renal Disorders
o Acute Glomerulonephritis
Follows streptococcal infection
Edema: Mild, usually around eyes
BP: Elevated
Urine: Dark, tea-colored (hematuria), slight or moderate proteinuria
Blood: Normal serum protein, positive ASO titer
Diet: low-sodium diet with no added salt
o Nephrotic Syndrome
Usually idiopathic
Edema: Severe, generalized
BP: Normal
Urine: Dark, frothy yellow, Massive proteinuria (b/c glomeruli permeability)
Blood: Decreased serum protein, Negative ASO titer
Diet: high-protein, low-salt diet
o Decreased urinary output is the first sign of renal failure.
o Surgical correction for hypospadias is usually done before preschool years to allow for the
achievement of sexual identity, to avoid castration anxiety, and to facilitate toilet training.
o Safe monitoring of Prednisone
Long-term prednisone should be given every other day.
Signs of edema, mood changes, and GI distress should be noted and reported.
The drug should be tapered, not discontinued suddenly.
o Preventing UTIs: Avoid bubble baths; void frequently; drink adequate fluids, especially acidic fluids
such as apple or cranberry juice; and clean genital area from front to back.
o Vesicoureteral reflex: a malfunction of the valves at the end of the ureters, allowing urine to refluxout of the bladder into the ureters and possibly into the kidneys
o Priorities for Wilms Tumor: Protect the child from injury to the encapsulated tumor (NO abdominal
palpation). Prepare the family and child for surgery.
GI Disorders
o Typical parent and family reactions to a child with an obvious malformation such as cleft lip or
palate are guilt, disappointment, grief, sense of loss, and anger.
o Children with cleft lip or palate and those with pyloric stenosis both have a nursing diagnosis of
“Alteration in nutrition; less than body requirements.”
Cleft lip or palate is related to decreased ability to suck.
Pyloric stenosis is related to frequent vomiting.
o Nutritional needs and fluid and electrolyte balance are key problems for children with GI disorders.
The younger the children, the more vulnerable they are to fluid and electrolyte imbalances and the
greater is the need for the caloric intake required for growth.
o Take axillary temperature in children with congenital megacolon.
o Feeding for cleft lip/palate: Use lamb’s nipple or prosthesis. Feed child upright, with frequent
bubbling.
o Esophageal Atresia with TEF
S&S: Choking, coughing, cyanosis, and excess salivation
Interventions: Maintain NPO immediately, and suction secretions.
o Post-op nursing care for infant with pyloric stenosis
Maintain IV hydration, and provide small, frequent oral feedings of glucose or electrolyte
solutions or both within 4 to 6 hours. Gradually increase to full-strength formula. Position
infant on right side in semi-Fowler position after feeding.
o Using a barium enema to treat intussusception A barium enema reduces the telescoping of the
intestine through hydrostatic pressure without surgical intervention.
o Pre-operative nursing care for a child with Hirschsprung Disease: Check vital signs and take axillary
temperatures. Provide bowel-cleansing program, and teach about colostomy. Observe for bowel
perforation; measure abdominal girth.
o Signs of anorectal malformation: A newborn who does not pass meconium within 24 hours;
meconium appearing through a fistula or in the urine; an unusual-appearing anal dimple
o Priorities for child undergoing abdominal surgery: Maintain fluid balance (I&O, nasogastric suction,
monitor electrolytes); monitor vital signs; care for drains, if present; assess bowel function; prevent
infection of incisional area and other postoperative complications; and support child and family
with appropriate teaching.
Hematologic Disorders
o Remember the Hgb norms:
Newborn: 14 to 24 g/dL
Infant: 10 to 17 g/dL
Child: 9.5 to 15.5 g/dL
o Iron
Teach family about administration of oral iron:
Give on empty stomach (as tolerated, for better absorption).
Give with citrus juices (vitamin C) for increased absorption.
Use dropper or straw to avoid discoloring teeth.
Teach that stools will become tarry.
Teach that iron can be fatal in severe overdose; keep away from other children.
Do not give with any dairy products.
Describe the information families should be given when a child is receiving oral iron
preparations.
Give oral iron on an empty stomach and with vitamin C. Use straws to avoid
discoloring teeth. Tarry stools are normal. Increase dietary sources of iron.
List dietary sources of iron.
Meat, green leafy vegetables, fish, liver, whole grains, legumes
o Inherited bleeding disorders (hemophilia and sickle cell anemia) are often used to test knowledge
of genetic transmission patterns. Remember: Autosomal recessive: Both parents must be heterozygous, or carriers of the recessive trait,
for the disease to be expressed in their offspring. With each pregnancy, there is a one in four
chance that the infant will have the disease. However, all children of such parents can get
the disease—not just 25% of them. This is the transmission pattern of sickle cell anemia,
cystic fibrosis, and phenylketonuria (PKU).
X-linked recessive trait: The trait is carried on the X chromosome; therefore, it usually
affects male offspring, as in hemophilia. With each pregnancy of a woman who is a carrier,
there is a 25% chance of having a child with hemophilia. If the child is male, he has a 50%
chance of having hemophilia. If the child is female, she has a 50% chance of being a carrier.
o Sickle Cell
Hydration is very important in the treatment of sickle cell disease because it promotes
hemodilution and circulation of red cells through the blood vessels.
Important terms
Heterozygous gene (HgbAS)—sickle cell trait
Homozygous gene (HbSS)—sickle cell disease
Abnormal hemoglobin (HgbS)—disease and trait
Supplemental iron is not given to clients with sickle cell anemia. The anemia is not caused
by iron deficiency. Folic acid is given orally to stimulate RBC synthesis.
A vaso-occlusive crisis is caused by the clumping of red blood cells, which blocks small
blood vessels; therefore, the cells cannot get through the capillaries, causing pain and tissue
and organ ischemia. Lowered oxygen tension affects HgbS, which causes sickling of the cells.
To prevent sickling: Keep child well hydrated. Avoid known sources of infections. Avoid
high altitudes. Avoid strenuous exercise.
o Acute Lymphocytic Leukemia
Have epinephrine and oxygen readily available to treat anaphylaxis when administering lasparaginase.
Prednisone is frequently used in combination with antineoplastic drugs to reduce the
mitosis of lymphocytes.
Allopurinol, a xanthine oxidase inhibitor, is also administered to prevent renal damage
caused by uric acid buildup and cellular lysis.
Nursing interventions for a child with leukemia are based off of what physiologic problems?
Anemia (decreased erythrocytes); infection (neutropenia); bleeding thrombocytopenia
(decreased platelets)
o Hemophilia: an X-linked recessive chromosomal disorder transmitted by the mother and expressed
in male children.
Metabolic and Endocrine Disorders
o Hypothyroidism
An infant with hypothyroidism is often described as a good, quiet baby by the parents.
Early detection of hypothyroidism and PKU is essential for preventing cognitive impairment
in infants. Knowledge of normal growth and development patterns is important because a
lack of attainment can be used to detect the presence of a disease and to evaluate the
treatment’s effects.
Diagnosed by screening for a low T-4 and a high TSH
Symptoms: Large, protruding tongue; coarse hair; lethargy; sleepiness; and constipation
Left untreated Mental retardation and growth failure
o PKU
NutraSweet (aspartame) contains phenylalanine and should not, therefore, be given to a
child with PKU.
Metabolic effects of PKU: CNS damage, mental retardation, and decreased melanin
Formulas given to PKU babies: Lofenalac and Phenex-1
Foods high in phenylalanine content: Meat, milk, dairy products, and eggs
o Diabetes
Diabetes mellitus (DM) in children was typically diagnosed as insulin-dependent diabetes
(type 1) until recently. A marked increase in type 2 DM has occurred recently in the United
States, particularly among Native American, African American, and Hispanic children andadolescents. Adolescence frequently causes difficulty in management because growth is
rapid, and the need to be like peers makes compliance difficult. Remember to consider the
child’s age, cognitive level of development, and psychosocial development when answering
NCLEX-RN questions.
When a child is in ketoacidosis, administer regular insulin IV in normal saline as prescribed.
There has been an increase in the number of children diagnosed with type 2 diabetes. The
increasing rate of obesity in children is thought to be a contributing factor. Other
contributing factors include lack of physical activity and a family history of type 2 diabetes.
S&S of DM: Polydipsia, polyphagia, and polyuria
Hypoglycemia: tremors, sweating, headache, hunger, nausea, lethargy, confusion, slurred
speech, anxiety, tingling around mouth, nightmares.
Hyperglycemia: polydipsia, polyuria, polyphagia, blurred vision, weakness, weight loss, and
syncope
Nursing care for a child with Ketoacidosis Provide care for an unconscious child,
administer regular insulin IV in normal saline, monitor blood gas values, and maintain strict
I&O.
Developmental factors that impact the school-age child with diabetes Need to be like
peers; assuming responsibility for own care; modification of diet; snacks and exercise in
school
During exercise, insulin uptake is increased and the risk for hypoglycemia occurs.
Skeletal Disorders
o Fractures in older children are common because they fall during play and are involved in motor
vehicle accidents.
Spiral fractures (caused by twisting) and fractures in infants may be related to child abuse.
Fractures involving the epiphyseal plate (growth plate) can have serious consequences in
terms of the growth of the affected limb.
o Skin traction for fracture reduction should not be removed unless health care provider prescribes
its removal.
o Pin sites can be source of infection. Monitor for signs of infection. Cleanse and dress pin sites as
prescribed.
o Skeletal disorders affect the infant’s or child’s physical mobility, and typical NCLEX-RN questions
focus on appropriate toys and activities for the child who is confined to bed rest and who is
immobilized.
o Children do not like injections and will deny pain to avoid “shots.”
o A brace does not correct the spine’s curve in a child with scoliosis; it only stops or slows the
progression.
o Log Rolling
Usually requires two or more persons, depending on the size of the client.
Client is carefully moved on a draw sheet to the side of the bed away from which they are to
be turned (moved to the left if they are to face to the right).
Client is then turned in a simultaneous motion (log-rolled), maintaining the spine in a
straight position.
Pillows are arranged for support and comfort, and they assist the client to maintain
alignment.
o Corticosteroids are used in the short term in low doses during exacerbations. Long-term use is
avoided because of side effects and their adverse effects on growth.
o Compartment Syndrome = Damage to nerves and vasculature of an extremity due to compression
S&S: cold extremity, severe pain, inability to move the extremity, and poor capillary refill
o Fractures of the epiphyseal plate (growth plate) may affect the growth of the limb.
o Skeletal traction is maintained by pins or wires applied to the distal fragment of the fracture.
o Child in Spica Cast: Check child’s circulation. Keep cast dry. Do not place anything under cast.
Prevent cast soilage during toileting or diapering. Do not turn child using an abductor bar.
o S&S of Congenital Hip Dysplasia: Unequal skin folds of the buttocks, Ortolani sign, limited abduction
of the affected hip, and unequal leg lengths
o Scoliosis screening: Ask the child to bend forward from the hips, with arms hanging free. Examinethe child for a curve in the spine, a rib hump, and hip asymmetry.
o Teaching to child with scoliosis in a brace: The child should be instructed to wear the brace 23
hours per day; wear a T-shirt under brace; check skin for irritation; perform back and abdominal
exercises; and modify clothing. The child should be encouraged to maintain normal activities as
able.
o Child with juvenile RA: Prescribed exercise to maintain mobility; splinting of affected joints; and
teaching about medication management and side effects of drugs.
Maternity
Anatomy and Physiology of Reproduction
o The menstrual phase varies in length in most women.
o Between ovulation and the beginning of the next menstrual cycle, there are usually exactly 14 days.
In other words, ovulation occurs 14 days before the next menstrual period.
o Sperm live approximately 3 days (48 to 72 hours), and eggs live about 24 hours. A couple must
avoid unprotected intercourse for several days before the anticipated ovulation and for 3 days after
ovulation to prevent pregnancy.
o Signs of ovulation: Abundant, thin, clear cervical mucus; spinnbarkeit (egg-white stretchiness) of
cervical mucus; open cervical os; slight drop in basal body temperature and then 0.5° to 1° F rise;
ferning under the microscope
Antepartum Nursing Care
o Because some women experience implantation bleeding or spotting, they do not know they are
pregnant.
o Pregnancy divided into three 13-week trimesters:
First trimester: from the first day of LMP through 13 weeks
Nursing interventions
o Teach prevention of nausea.
Suggest eating dry crackers before getting out of bed in the morning.
Suggest eating small, frequent meals; avoiding fatty foods; and
avoiding skipping meals.
o Teach safety.
Avoid hot tubs, saunas, and steam rooms throughout pregnancy
(increases risk for neural tube defects in first trimester; hypotension
may cause fainting).
o Prepare client for pregnancy.
Discuss attitudes toward pregnancy.
Discuss value of early pregnancy classes that focus on what to expect
during pregnancy.
Provide information about childbirth preparation classes.
Include father and family in preparation for childbirth (expectant
fathers experience many of the same feelings and conflicts
experienced by the expectant mother).
o Teach prevention of urinary tract infections.
Encourage adequate fluid intake (3 L/day).
Instruct to void frequently (every 2 hours while awake).
Encourage to void before and after intercourse.
Teach to wipe from front to back.
o Discuss nutrition and exercise.
Increase caloric intake by 300 calories per day.
Stress the value of regular exercise.
o Discuss possible effects of pregnancy on sexual relationship. Recognize
father’s role as he labors to incorporate the parental role into his selfidentity.
Second trimester: 14 weeks through 26 weeks
Nursing Interventionso Explain the screening test, and obtain blood sample for maternal serum
alpha-fetoprotein (MSAFP) between 15 and 22 weeks of gestation, ideally
between 16 and 18 weeks of gestation.
Elevated levels are associated with open neural tube defects and
multiple gestations.
Low levels are associated with Down syndrome. Abnormal levels are
followed by second-trimester ultrasonography for more in-depth
investigation.
o Explain the multiple-marker, or triple-screen, blood test, and obtain a
specimen for screening between 16 and 18 weeks of gestation to measure
the MSAFP, human chorionic gonadotropin (hCG), and unconjugated estriol,
the levels of which are combined to yield one value.
Low levels may be associated with Down syndrome and other
chromosomal abnormalities.
o Teach comfort measures.
Encourage to remain active.
Encourage to sit with feet elevated when possible.
Teach to avoid pressure on lower thighs.
Teach that use of support stockings may be helpful.
Teach to dorsiflex foot to relieve leg cramps.
Suggest applying heat to muscles affected by cramps.
Suggest that cool-air vaporizer or saline nasal spray may help with
nasal stuffiness.
o Teach measures to avoid constipation.
Encourage to eat raw fruits, vegetables, cereals with bran.
Encourage to drink 3 L of fluid per day.
Encourage to exercise frequently.
o Explain and obtain a blood sample for a glucose challenge that is usually
done between 24 and 28 weeks’ gestation.
o At between 24 and 32 weeks’ gestation, two or three ultrasound
measurements may be taken 2 weeks apart to compare against standard
fetal growth curves.
Third trimester: 27 weeks to 40 weeks
Nursing interventions
o Teach treatment of hemorrhoids.
Suggest sitz baths.
Suggest topical anesthetic agents.
Suggest taking stool softeners as prescribed.
o Teach comfort measures.
Encourage woman to elevate legs when sitting.
Suggest that woman assume side-lying position when resting.
o Teach measures to avoid heartburn.
Teach woman to eat small, frequent meals.
Teach avoidance of fatty foods.
Encourage woman to avoid lying down after meals.
Teach that antacids may be prescribed.
Teach woman to avoid sodium bicarbonate.
o Prepare woman for delivery and parenthood.
Discuss mother’s, father’s, and family’s expectations of labor and
delivery.
Discuss mother’s, father’s, and family’s expectations about caring for
infant.
Encourage woman to start childbirth-preparation classes.
o Teach measures to decrease edema.
Encourage woman to elevate legs one or two times per day forapproximately 1 hour.
o Teach comfort measures.
Encourage woman to wear well-fitting supportive bra.
Encourage woman to maintain proper posture.
Teach woman to use semi-Fowler position at night for dyspnea.
o Prepare woman for childbirth.
Review signs of labor.
Discuss plans for other children (if any).
Discuss plans for transportation to agency.
Assess father’s (family member’s) role during childbirth.
o Teach safety measures.
Teach to wear low-heeled shoes or flats.
Instruct to avoid heavy lifting.
Encourage sleeping on side to relieve bladder pressure and urinating
frequently.
o Encourage preparation for delivery.
Teach woman to do pelvic tilt exercises.
Encourage packing a suitcase.
Encourage couple to tour labor and delivery area.
Discuss postpartum circumstances: circumcision, rooming-in,
possibility of postpartum blues, birth control, need for adequate rest,
father’s role.
o Maternal position that provides optimum fetal and placental perfusion during pregnancy: The kneechest position, but the ideal position of comfort for the mother, which supports fetal, maternal, and
placental perfusion, is the side-lying position (removes pressure from the abdominal vessels [vena
cava, aorta]).
o Look for signs of maternal–fetal bonding during pregnancy; for example, talking to fetus in utero,
massaging abdomen, and nicknaming fetus are all healthy psychosocial activities.
Normal psychosocial response to pregnancy during 2nd trimester = Ambivalence wanes and
acceptance of pregnancy occurs; pregnancy becomes “real”; signs of maternal–fetal bonding
occur.
o Normal weight gain during pregnancy: Total gain should average 25 to 35 lb. Gain should be
consistent throughout pregnancy. An average of 1 lb/week should be gained in the second and third
trimesters.
o For many women, battering (emotional or physical abuse) begins during pregnancy. A nurse who is
familiar with local resources and knows how to determine the safety of the client should assess
women for abuse in private, away from the male partner.
o Practice determining gravidity and parity. A woman who is 6 weeks pregnant has the following
maternal history:
She has a healthy 2-year-old daughter.
She had a miscarriage at 10 weeks.
She had an elective abortion at 6 weeks, 5 years earlier.
With this pregnancy, she is a gravida 4, para 1 (only 1 delivery after 20 weeks’ gestation).
GTPAL is 4-1-0-2-1
o Practice calculating EDB. If the first day of a woman’s last normal menstrual period was October 17,
what is her EDB, using the Nägele rule? July 24. Count back 3 months and add 7 days (always give
February 28 days).
o At approximately 28 to 32 weeks’ gestation, a plasma volume increase of 25% to 40% occurs,
resulting in normal hemodilution of pregnancy and Hct values of 32% to 42%. High Hct values may
look good, but in reality they represent a gestational hypertension disorder and a depleted vascular
space.
o Hgb and Hct data can be used to evaluate nutritional status. Example: A 22-year-old primigravida at
12 weeks’ gestation has an Hgb of 9.6 g/dL and an Hct of 31%. She has gained 3 pounds during the
first trimester. A weight gain of 2 to 4 pounds during the first trimester is recommended, and this
client is anemic. Supplemental iron and a diet higher in iron are needed. Foods high in iron:
Fish and red meats
Cereals and yellow vegetables
Green leafy vegetables and citrus fruits
Egg yolks and dried fruits
o As pregnancy advances, the uterus presses on abdominal vessels (vena cava and aorta). Teach the
woman that a left side-lying position relieves supine hypotension and increases perfusion to uterus,
placenta, and fetus.
o Fetal well-being is determined by assessing fundal height, fetal heart tones and rate, fetal
movement, and uterine activity (contractions). Changes in FHR are the first and most important
indicators of compromised blood flow to the fetus, and these changes require action! Remember,
the normal FHR is 110 to 160 bpm.
FHR can be detected at 10-12 weeks by Doppler ultrasound.
o Prenatal visit schedule for woman with low-risk pregnancy: Once every 4 weeks until 28 weeks;
every 2 weeks from 28 to 36 weeks; then once a week until delivery
o Teach clients to report immediately any of the following danger signs. Early intervention can
optimize maternal and fetal outcome. Possible indications of preeclampsia and eclampsia are:
Visual disturbances
Swelling of face, fingers, or sacrum
Severe, continuous headache
Persistent vomiting
Epigastric pain
Infection. Signs include:
Chills
Temperature over 100.4° F
Dysuria
Pain in abdomen
Fluid discharge or bleeding from vagina (anything other than normal leukorrhea)
o Most providers prescribe prenatal vitamins to ensure that the client receives an adequate intake of
vitamins. However, only the health care provider can prescribe prenatal vitamins. It is the nurse’s
responsibility to teach about proper diet and about taking prescribed vitamins as the health care
provider has prescribed them.
o It is recommended that pregnant women consume the equivalent of 3 cups of milk or yogurt per
day. This will ensure that the daily calcium needs are met and help to alleviate the occurrence of leg
cramps.
Fetal and Maternal Assessment Techniques
o Maternal variables associated with a high-risk pregnancy: Age (under 17 or over 34 years of age);
parity (over 5); <3 months between pregnancies; diagnosis of preeclampsia, diabetes mellitus, or
cardiac disease
o In some states, screening for neural tube defects by testing either maternal serum alpha-fetoprotein
(AFP) levels or amniotic fluid AFP levels is mandated by state law. This screening test is highly
associated with both false positives and false negatives.
o An early sonogram rather than a later one best determines gestational age.
o Nursing Care during Ultrasound
Instruct the woman to drink 3 to 4 glasses of water prior to coming for examination and not
to urinate. When the fetus is very small (in the first and second trimesters), the client’s
bladder must be full during the examination in order for the uterus to be supported for
imaging. (A full bladder is not needed if ultrasound is done transvaginally instead of
abdominally.)
Position the woman with pillows under neck and knees to keep pressure off bladder; late in
the third trimester, place wedge under right hip to displace uterus to the left.
o Serial ultrasounds are needed to determine IUGR.
o BPP determines fetal well being.
o Chorionic Villi Sampling: Can be done between 8 and 12 weeks’ gestation, with results returned
within 1 week, which allows for decision about termination while still in first trimester.o When an amniocentesis is done in early pregnancy, the bladder must be full to help support the
uterus and to help push the uterus up in the abdomen for easy access. When an amniocentesis is
done in late pregnancy, the bladder must be empty so it will not be punctured.
Common complications of amniocentesis: infection, spontaneous abortion, and fetal injury
o Serum or amniotic AFP levels are drawn prenatally to determine whether AFP levels are elevated,
which may indicate the presence of neural tube defects; or whether they are low, which may
indicate trisomy 21.
o FHR Monitoring
Accelerations are caused by a burst of sympathetic activity; they are reassuring and require
no treatment.
Early decelerations are caused by head compression; they are benign and alert the nurse to
monitor for labor progress and fetal descent.
Early decelerations, caused by head compression and fetal descent, usually occur
between 4 and 7 cm and in the second stage of labor. Check for labor progress if
early decelerations are noted.
Variable decelerations are caused by cord compression; change of position should be tried
first.
Variable decelerations: It occurs in 40% of all labors and is caused mainly by cord
compression but can also indicate rapid fetal descent. It is characterized by an
abrupt transitory decrease in the FHR that is variable in duration, depth of fall, and
timing relative to the contraction cycle.
Nursing interventions should include changing maternal position, discontinuing
oxytocin (Pitocin) infusion, administering oxygen, and notifying the health care
provider.
If cord prolapse is detected, the examiner should position the mother to relieve
pressure on the cord (i.e., knee-chest position) or push the presenting part off the
cord until immediate cesarean delivery can be accomplished.
Late decelerations are caused by UPI and should be treated by placing client on her side and
administering oxygen.
Late decelerations indicate UPI (uterine placental insufficiency) and are associated
with conditions such as postmaturity, preeclampsia, diabetes mellitus, cardiac
disease, and abruptio placentae
Nursing interventions should include changing maternal position, discontinuing
oxytocin (Pitocin) infusion, administering oxygen, and notifying the health care
provider.
When deceleration patterns (late or variable) are associated with decreased or
absent variability and tachycardia, the situation is ominous (potentially disastrous)
and requires immediate intervention and fetal assessment.
Variability
Most important indicator of fetal autonomic nervous system integrity and health
Decreased or absent variability can be related to hypoxia, acidosis, drugs, fetal sleep
o Contraction Stress Test
The danger of nipple stimulation lies in controlling the “dose” of oxytocin delivered by the
posterior pituitary. The chance of hyperstimulation or tetany (contractions over 90 seconds
or contractions with less than 30 seconds in between) is increased.
An unhealthy fetus will develop nonreassuring FHR patterns in response to uterine
contractions; late decelerations are indicative of UPI.
o Nonstress Test
It is used to determine fetal well-being in high-risk pregnancy and is especially useful in
postmaturity (notes response of the fetus to its own movements).
A reactive non-stress test = FHR acceleration of 15 bpm for 15 seconds in response to fetal
movement
If no fetal movement for 30 minutes: Suspect fetus is sleeping if there is no fetal movement.
Stimulate fetus acoustically or physically or have mother move fetus around and begin test
again.o Percutaneous umbilical blood sampling (PUBS) can be done during pregnancy under ultrasound for
prenatal diagnosis and therapy. Hemoglobinopathies, clotting disorders, sepsis, and some genetic
testing can be done using this method.
o The most import determinant of fetal maturity for extrauterine survival is the lung maturity:lung
surfactant (L/S) ratio (2:1 or higher).
o Normal fetal scalp pH in labor is 7.25-7.35, and values below 7.2 indicate true acidosis.
Intrapartum Nursing Care
o Be able to differentiate true labor from false labor.
True Labor
Pain in lower back that radiates to abdomen
Pain accompanied by regular rhythmic contractions
Contractions that intensify with ambulation
Progressive cervical dilatation and effacement
False Labor
Discomfort localized in abdomen
No lower back pain
Contractions decrease in intensity or frequency with ambulation
o Leopold Maneuvers
Description: Abdominal palpations used to determine fetal presentation, lie, position, and
engagement
With client in supine position, place both cupped hands over fundus and palpate to
determine whether breech (soft, immovable, large) or vertex (hard, movable, small).
Place one hand firmly on side and palpate with other hand to determine presence of small
parts or fetal back. (FHR is heard best through fetal back.)
Facing client, grasp the area over the symphysis with the thumb and fingers and press to
determine the degree of descent of the presenting part. (A ballotable or floating head can be
rocked back and forth between the thumb and fingers.)
Facing the client’s feet, outline the fetal presenting part with the palmar surface of both
hands to determine the degree of descent and attitude of the fetus. (If cephalic prominence
is located on the same side as small parts, assume the head is flexed.)
o It is important to know the normal findings for a client in labor:
Normal FHR in labor: 110 to 160 bpm
Normal maternal BP: <140/90
Normal maternal pulse: <100 bpm
Normal maternal temperature: <100.4° F
Slight elevation in temperature may occur because of dehydration and the work of labor.
Anything higher indicates infection and must be reported immediately.
o If infant’s head is floating, watch for cord prolapse.
o Meconium-stained fluid is yellow-green or gold-yellow and may indicate fetal stress.
o Breathing techniques, such as deep chest, accelerated, and cued, are not prescribed by the stage and
phase of labor but by the discomfort level of the laboring woman. If coping is decreasing, switch to a
new technique.
o Hyperventilation results in respiratory alkalosis that is caused by blowing off too much CO2.
Symptoms include:
Dizziness
Tingling of fingers
Stiff mouth
Have woman breathe into her cupped hands or a paper bag in order to rebreathe CO2.
o Determine cervical dilatation before allowing client to push. Cervix should be completely dilated
(10 cm) before the client begins pushing. If pushing starts too early, the cervix can become
edematous and never fully dilate.
o Give the oxytocin (Pitocin) after the placenta is delivered because the drug will cause the uterus to
contract. If the oxytocic drug is administered before the placenta is delivered, it may result in a
retained placenta, which predisposes the client to hemorrhage and infection.
o Application of Perineal Pads After Delivery Place two on perineum.
Do not touch inside of pad.
Do apply from front to back, being careful not to drag pad across the anus.
o Methergine is not given to clients with hypertension because of its vasoconstrictive action. Pitocin
is given with caution to those with hypertension.
o Never give Methergine or Hemabate to a client while she is in labor or before delivery of the
placenta.
o Full bladder is one of the most common reasons for uterine atony or hemorrhage in the first 24
hours after delivery. If the nurse finds the fundus soft, boggy, and displaced above and to the right
of the umbilicus, what action should be taken first? First, perform fundal massage; then have the
client empty her bladder. Recheck fundus every 15 minutes for 1 hour, then every 30 minutes for 2
hours.
o If narcotic analgesics are given, raise side rails and place call light within reach. Instruct client not
to get out of bed or ambulate without assistance. Caution client about drowsiness as a side effect.
o A first-degree tear involves only the epidermis. A second-degree tear involves dermis, muscle, and
fascia. A third-degree tear extends into the anal sphincter. A fourth-degree tear extends up the
rectal mucosa. Tears cause pain and swelling. Avoid rectal manipulations.
o Do not wait until a 1-minute Apgar is assigned to begin resuscitation of the compromised neonate.
o Apgar scores of 6 or lower at 5 minutes require an additional Apgar assessment at 10 minutes
o IV administration of analgesics is preferred to IM administration for a client in labor because the
onset and peak occur more quickly and the duration of the drug is shorter. It is important to know
the following:
IV Administration
Onset: 5 minutes
Peak: 30 minutes
Duration: 1 hour
IM Administration
Onset: within 30 minutes
Peak: 1 to 3 hours after injection
Duration: 4 to 6 hours
o Tranquilizers (ataractics and phenothiazines), such as Phenergan and Vistaril, are used in labor as
analgesic-potentiating drugs to decrease the amount of narcotic needed and to decrease maternal
anxiety.
o Agonist narcotic drugs (morphine) produce narcosis and have a higher risk for causing maternal
and fetal respiratory depression. Antagonist drugs (Stadol, Nubain) have less respiratory
depression but must be used with caution in a mother with preexisting narcotic dependency
because withdrawal symptoms occur immediately.
o Pudendal block and subarachnoid (saddle) block are used only in the second stage of labor.
Peridural and epidural blocks may be used during all stages of labor.
o The first sign of a block’s effectiveness is usually warmth and tingling in the ball of the foot or the
big toe.
o Stop continuous infusion at end of stage I or during transition to increase effectiveness of pushing.
o Regional Block Anesthesia and Fetal Presentation
Internal rotation is harder to achieve when the pelvic floor is relaxed by anesthesia; this
results in a persistent occiput-posterior position of fetus.
Monitor fetal position. Remember, the mother cannot tell you she has back pain, which is
the cardinal sign of persistent posterior fetal position.
Regional blocks, especially epidural and caudal blocks, commonly result in assisted (forceps
or vacuum) delivery because of the inability to push effectively during the second stage.
o Five prodromal signs of labor the nurse might teach the client: Lightening, Braxton Hicks
contractions, increased bloody show, loss of mucous plug, burst of energy, and nesting behaviors.
o Two ways to determine whether the membranes have truly ruptured
Nitrazine testing: Paper turns dark blue or black
Demonstration of fluid ferning under microscope
o Clients should use breathing techniques according to their discomfort level and should changetechniques when one is no longer working for relaxation.
o Reasons to withhold anesthesia and analgesia until the midactive phase of stage I labor If
analgesia and anesthesia are given too early, they can retard labor; if given too late, they can cause
fetal distress.
o Hyperventilation often occurs in the laboring client Respiratory alkalosis occurs; it is caused by
blowing off CO2 and is relieved by breathing into a paper bag or cupped hands
o The maternal changes that characterize the transition phase of labor are irritability and
unwillingness to be touched, but does not want to be left alone; nausea, vomiting, and hiccupping
o Vaginal examinations should be done prior to analgesia and anesthesia to rule out cord prolapse, to
determine labor progress if it is questioned, and to determine when pushing can begin.
o Cervical effacement The taking up of the lower cervical segment into the upper segment; the
shortening of the cervix expressed in percentages from 0% to 100%, or complete effacement.
o FHR is best heard through the fetal back in vertex, OA positions
o Nursing actions for the second stage of labor Make sure cervix is completely dilated before
pushing is allowed. Assess FHR with each contraction. Teach woman to hold breath for no longer
than 10 seconds. Teach pushing technique.
o Signs of placental separation Gush of blood, lengthening of cord, and globular shape of uterus
o The postpartum dosage of oxytocin (Pitocin) be administered immediately after placenta is
delivered to prevent postpartum hemorrhage and atony.
o Symptoms of respiratory distress in the newborn Tachypnea, dusky color, flaring nares,
retractions, and grunting
o If meconium was passed in utero, the nurse must arrange for immediate endotracheal tube
observation to determine the presence of meconium below the vocal cords (prevents pneumonitis
and meconium aspiration syndrome).
o A good Apgar score = 7-10
o The purpose of eye prophylaxis in the newborn is to prevent ophthalmia neonatorum, which results
from exposure to gonorrhea in the vagina
o The danger associated with regional blocks is hypotension resulting from vasodilatation below the
block, which pools blood in the periphery, reducing venous return
o The major cause of maternal death when general anesthesia is administered is aspiration of gastric
contents
o PO medications are avoided in labor because gastric activity slows or stops in labor, decreasing
absorption from PO route; it may cause vomiting.
o The best way to administer IV drugs during labor is at beginning of contraction, push a little
medication in while uterine blood vessels are constricted, thereby reducing dose to fetus.
o It is dangerous to administer butorphanol (Stadol), an agonist/antagonist narcotic, when the client
is an undiagnosed drug abuser of narcotics, it can cause immediate withdrawal symptoms.
o Hypotension commonly occurs after the laboring client receives a regional block. One of the first
signs is nausea.
Actions the nurse should take when hypotension occurs in a laboring client.
Turn client to left side.
Administer O2 by mask at 10 L/min.
Increase speed of intravenous infusion (if it does not contain medication).
o The fourth stage of labor is defined as the first 1 to 4 hours after delivery of placenta
o To prevent postpartum hemorrhage, the nurse can massage the fundus (gently) and keep the
bladder emptied.
o To promote comfort for a third-degree episiotomy that extends into the anal sphincter Ice pack,
witch hazel compresses, and no rectal manipulation
o To enhance maternal–infant bonding during the fourth stage of labor, withhold eye prophylaxis for
up to 1 hour. Perform newborn admission and routine procedures in room with parents. Encourage
early initiation of breastfeeding. Darken room to encourage newborn to open eyes.
o To ease the discomfort of afterpains keep bladder empty, provide a warm blanket for abdomen,
administer analgesics prescribed by health care provider.
o The symptoms of a full bladder that might occur in the fourth stage of labor Fundus above
umbilicus, dextroverted (to the right side of abdomen), increased bleeding (uterine atony)o When a soft, boggy uterus is palpated, the nurse should first perform fundal massage.
o The symptoms of hypovolemic shock Pallor, clammy skin, tachycardia, lightheadedness, and
hypotension
o The nurse should check the fundus during the fourth stage of labor every l5 minutes for 1 hour;
every 30 minutes for 2 hours if normal
Normal Postpartum
o Normal leukocytosis of pregnancy averages 12,000 to 15,000 mm3. During the first 10 to 12 days
postdelivery, values of 25,000 mm3 are common. Elevated WBC and the normal elevated
Erythrocyte Sedimentation Rate (ESR) may confuse interpretation of acute postpartal infections.
For example, if the nurse assesses a client’s temperature to be 101° F on the client’s second
postpartum day, what assessments should be made before notifying the physician? Assess fundal
height and firmness; assess perineal integrity; check for signs and symptoms of thromboembolism;
assess pulse, respirations, and BP; assess client’s subjective description of symptoms (e.g., burning
on urination, pain in leg, excessive tenderness of uterus).
o Client and family teaching is a common subject of NCLEX-RN® questions. Remember that when
teaching the first step is to assess the clients’ (parents’) level of knowledge and to identify their
readiness to learn. Client teaching regarding lochia changes, perineal care, breastfeeding, and sore
nipples are subjects that are commonly tested.
o Normal PP Vital Signs
Temperature
May rise to 100.4° F due to dehydrating effects of labor. Any higher elevation may be
due to infection and must be reported.
Pulse
May decrease to 50 (normal puerperal bradycardia). Pulse >100 may indicate
excessive blood loss or infection.
Blood pressure
Should be normal. Suspect hypovolemia if it decreases, preeclampsia if it increases.
Respirations
Rarely change. If respirations increase significantly, suspect pulmonary embolism,
uterine atony, or hemorrhage.
o After the first postpartum day, the most common cause of uterine atony is retained placental
fragments. The nurse must check for the presence of fragments in lochial tissue.
o Women can tolerate blood loss, even slightly excessive blood loss, in the postpartal period because
of the 40% increase in plasma volume during pregnancy. In the postpartal period, a woman can
void up to 3000 mL/day to reduce the volume increase that occurred during pregnancy.
o Postpartum Teaching
Breast Self-Examination
Begin with inspection in a mirror. Place both hands at sides and observe; then look
again with hands overhead and bending forward. Assess for:
o Change in size and shape
o Dimpling, puckering, scaling, redness, swelling of any part of breast
Lie flat with right hand under head and pillow or towel under right shoulder.
Use left hand to palpate using concentric circles around right breast, feeling for
lumps, nodules, or thickening.
Repeat with left breast.
Episiotomy Care
Perineal care
Fill a squeeze bottle with warm water and, if prescribed, an ounce of povidoneiodine solution.
Lavage perineum with several squirts and blot dry instead of rubbing; avoid anal
area.
o Client should void within 4 hours of delivery. Monitor client closely for urine retention. Suspect
retention if voiding is frequent and <100 mL per voiding.
o Women often have a syncopal (fainting) spell on the first ambulation after delivery (usually related
to vasomotor changes, orthostatic hypotension). The astute nurse will check client’s Hgb and Hctfor anemia and BP, sitting and lying down, to ascertain orthostatic hypotension.
o Kegel exercises increase the integrity of the introitus and improve urine retention. Teach client to
alternate contraction and relaxation of the pubococcygeal muscles.
o Assess for thromboembolism: Examine legs of postpartum client daily for pain, warmth, and
tenderness or a swollen vein that is tender to the touch.
o Remember, RhoGAM is given to an Rh-negative mother who delivers an Rh-positive fetus and has a
negative direct Coombs test. If the mother has a positive Coombs test, there is no need to give
RhoGAM because the mother is already sensitized.
Because Rh immune globulins suppress the immune system, the client who receives both
RhoGAM and the rubella vaccine should be tested for rubella immunity at 3 months.
o “Postpartum blues” are usually normal, especially 5 to 7 days after delivery (unexplained
tearfulness, feeling down, and having a decreased appetite). Encourage use of support persons to
help with housework for first 2 postpartum weeks. Refer to community resources.
The Normal Newborn
o A detailed physical assessment is performed by the nurse or physician. Regardless of who performs
the physical assessment, the nurse must know normal versus abnormal variations in the newborn.
Observations must be recorded and the physician notified regarding abnormalities.
o Suction the mouth first and then the nose. Stimulating the nares can initiate inspiration, which
could cause aspiration of mucus in oral pharynx.
o It is difficult to differentiate between caput succedaneum (edema under the scalp) and
cephalohematoma (blood under the periosteum). The caput crosses suture lines and is usually
present at birth, whereas the cephalohematoma does not cross suture lines and manifests a few
hours after birth. The danger of cephalohematoma is increased hyperbilirubinemia due to excess
RBC breakdown.
o The umbilical cord should always be checked at birth. It should contain three vessels: one vein,
which carries oxygenated blood to the fetus, and two arteries, which carry unoxygenated blood
back to the placenta. This is the opposite of normal circulation in the adult. Cord abnormalities
usually indicate cardiovascular or renal anomalies.
o Postnatally, the fetal structures of foramen ovale, ductus arteriosus, and ductus venosus should
close. If they do not, cardiac and pulmonary compromise will develop.
o Infant neurologic reflexes are transient and, as such, disappear usually within the first year of life.
In the pediatric client, prolonged presence of these reflexes can indicate CNS defects. Anticipate
NCLEX-RN questions regarding normal newborn reflexes. Physical assessment questions focus on
normal characteristics of the newborn and the differentiation of conditions such as caput
succedaneum and cephalohematoma.
o Circumcision has become controversial because there is no real medical indication for the
procedure, and it does cause trauma and pain to the newborn. It was once thought to decrease the
incidence of penile and cervical cancer, but some researchers say this is unfounded.
o Hypothermia (heat loss) leads to depletion of glucose and, therefore, to the use of brown fat
(special fat deposits fetus develops in last trimester; they are important to thermoregulation) for
energy. This results in ketoacidosis and possible shock. Prevent by keeping neonate warm!
o Heelstick Procedure for Newborns
Wash hands and put on gloves.
Clean heel with alcohol and dry with a gauze pad.
Choose a site for puncture that avoids the plantar artery in the middle of the heel.
Use only the lateral surfaces of the heel.
Puncture deep enough to trigger a free flow of blood. Wipe away first drop with sterile
gauze pad.
Collect blood in appropriate tube, on card, or on glucose “stick.”
o Physiologic jaundice occurs at 2 to 3 days of life. If it occurs before 24 hours or persists beyond 7
days, it becomes pathologic. Typically, NCLEX-RN questions ask about the normal problem of
physiologic jaundice, which occurs 2 to 3 days after birth due to the immature liver’s normal
inability to keep up with RBC destruction and to bind bilirubin. Remember, unconjugated bilirubin
is the culprit.
o To evaluate exact urine output, weigh dry diaper before applying. Weigh the wet diaper after infanthas voided. Calculate and record each gram of added weight as 1 mL urine.
o Do not feed a newborn when the respiratory rate is over 60. Inform the physician and anticipate
gavage feedings in order to prevent further energy utilization and possible aspiration.
o A 7 lb 8 oz baby would need 50 calories × 7 lb = 350 calories plus 25 calories (½ lb or 8 oz) = 375
calories per day. Most infant formulas contain 20 calories per oz. Dividing 375 by 20 = 18.75 oz of
formula needed per day.
o Teach parents to take infant’s temperature, both axillary and rectal. Axillary is recommended, but
some pediatricians request a rectal (core) temperature.
Axillary: Place thermometer under infant’s arm and hold thermometer in place for 5
minutes.
Rectal: Use thermometer with blunt end. Insert thermometer ¼ to ½ inch and hold in place
for 5 minutes. Hold feet and legs firmly.
High-Risk Disorders
o Clients with prior traumatic delivery, history of D&C, and multiple abortions (spontaneous or
induced) and daughters of diethylstilbestrol (DES) mothers may experience miscarriage or preterm
labor related to incompetent cervix. The cervix may be surgically repaired prior to pregnancy, or
during gestation. A cerclage (a McDonald suture) is placed around the cervix to constrict the
internal os. The cerclage may be removed prior to labor if labor is planned or left in place if
cesarean birth is planned.
o If hCG levels do not diminish, choriocarcinoma may develop. Pregnancy may mask the signs and
symptoms of choriocarcinoma.
o Suspect ectopic pregnancy in any woman of childbearing age who presents at an emergency room,
clinic, or office with unilateral or bilateral abdominal pain. Most are misdiagnosed as appendicitis.
o A client who is at 32 weeks’ gestation calls the health care provider because she is experiencing
dark-red vaginal bleeding. She is admitted to the emergency department, where the nurse
determines the FHR to be 100 bpm. The client’s abdomen is rigid and boardlike, and she is
complaining of severe pain. What action should the nurse take first? First, the nurse must use her or
his knowledge base to differentiate between abruptio placentae (this client) and placenta previa
(painless bright-red bleeding occurring in the third trimester). The nurse should immediately notify
the health care provider, and no abdominal or vaginal manipulation or examinations should be
done. Administer O2 by face mask. Monitor for bleeding at IV sites and gums because of the
increased risk for DIC. Emergency cesarean section is required because uteroplacental perfusion to
the fetus is being compromised by early separation of the placenta from the uterus.
o Abruptio Placentae
Institute bed rest with no vaginal or rectal manipulation, and notify health care provider
immediately.
Monitor BP and pulse every 15 minutes; apply electric BP monitor if available.
Apply external uterine and fetal monitor.
Place client in side-lying position to increase uterine perfusion.
Closely monitor contractions and FHR.
Begin IV infusion with 16- to 18-gauge catheter
Review results for CBC, clotting studies, Rh factor, and type/crossmatch stat.
Watch for signs of developing DIC:
Bleeding gums or nose
Reduced lab values for platelets, fibrinogen, and prothrombin
Bleeding from injection sites, IV sites
Ecchymosis
Prepare for immediate emergency cesarean section.
Monitor blood loss; save pads and linens.
Provide constant nurse surveillance and allow presence of family if available.
Provide emotional support; teach regarding usual management and expected outcomes of
abruption.
o Placenta Previa
Use bed rest to extend the period of gestation until fetal lung maturity is achieved
(determined by an L/S ratio of at least 2:1); then delivery is accomplished. If determined during labor, institute bed rest immediately and notify physician.
Monitor BP and pulse every 15 minutes.
Start IV to administer fluids.
Obtain blood specimen for CBC, clotting studies, Rh factor, and type/crossmatch.
Monitor contractions and FHR; place external monitor on client immediately.
Place in side-lying position.
Continue monitoring blood loss; save pads and linen.
Prepare client for ultrasound diagnosis.
Prepare client and family for possible cesarean birth if placenta previa is complete.
Provide emotional support and appropriate teaching regarding usual management and
outcomes of placenta previa.
o Disseminated intravascular coagulation (DIC) is a syndrome of abnormal clotting that is systematic
and pathologic. Large amounts of clotting factors, especially fibrinogen, are depleted, causing
widespread external and internal bleeding. DIC is related to fetal demise, infection and sepsis,
pregnancy-induced hypertension (preeclampsia), and abruptio placentae. (DIC is discussed in
greater detail in Advanced Clinical Concepts).
o Clients with abruptio placentae or placenta previa (actual or suspected) should undergo no
abdominal or vaginal manipulation.
No Leopold maneuvers
No vaginal examination
No rectal examinations, enemas, or suppositories
No internal monitoring
o Tetracycline is contraindicated in pregnancy because it darkens the teeth of the newborn.
o Podophyllin, which is usually used to treat HPV, is contraindicated in pregnancy because it is
associated with fetal death, preterm labor, and cervical carcinoma. Quadrivalent human
papillomavirus (types 6, 11, 16, 18) recombinant vaccine (Gardasil) is available to nonpregnant
females 9 years and older to prevent HPV.
o Toxoplasmosis is usually related to exposure to cats, gardening (where cat feces may be found), or
eating raw meat.
o Rubella is teratogenic to the fetus during the first trimester, causing congenital heart disease,
congenital cataracts, or both. All women should have their titers checked during pregnancy. If a
woman’s titers are low, she should receive the vaccine after delivery and be instructed not to get
pregnant within 3 months. Breastfeeding mothers may take the vaccine.
o Acyclovir (used to treat herpes simplex) is not recommended during pregnancy.
o Although metronidazole (Flagyl) is the treatment of choice for some vaginal infections, its use is
contraindicated in the first trimester of pregnancy, and its use during the second trimester is
controversial.
o Medications usually recommended for a nonpregnant client with an STD may be contraindicated
for the pregnant client because of effects on the fetus.
o The outcome of adolescent pregnancy depends on prenatal care. Nutrition is a key factor because
the adolescent’s physiologic needs for growth are already higher, and the additional stress of
pregnancy only increases those needs.
o Dystocia frequently requires the use of oxytocin for augmentation or induction of labor. Uterine
tetany is a harmful complication, and careful monitoring is required. The desired effect is
contractions every 2 to 3 minutes, with duration of contractions no longer than 90 seconds.
Continuously monitor FHR and uterine resting tone. If tetany occurs, turn off oxytocin (Pitocin),
turn client to a side-lying position, and administer O2 by face mask. Check output (should be at least
100 mL/4 hr). Oxytocin’s most important side effect is its antidiuretic (ADH) effect, which can cause
water intoxication. Using IV fluids containing electrolytes decreases the risk for water intoxication.
o Although the toxic side effects of magnesium sulfate are well known and watched for, it is just as
important to get serum blood levels of magnesium sulfate above 4 mg/dL in order to prevent
convulsions and to reach therapeutic range.
o Hold next dose of magnesium sulfate and notify health care provider if any toxic symptoms occur
(<12 respirations/min, urine output <100 mL/4 hr, absent DTRs, magnesium sulfate serum levels
>8 mg/dL).o When administering magnesium sulfate, always have antidote available (calcium gluconate,).
o Tachycardia is the major side effect of tocolytic drugs, which are beta-adrenergic agents, such as
terbutaline (Brethine); they are used to stop preterm labor. Teach the client to take her pulse prior
to administration and to withhold medication if pulse is not within the prescribed parameters
(usually withheld if pulse is >120-140). If administration is via a continuous pump, teach client to
monitor pulse periodically.
o Nursing Protocol for Administration of Oxytocin
Determine any contraindications to use of oxytocin.
Known cephalopelvic disproportion (CPD)
Fetal stress
Placenta previa
Prior classical incision into uterus
Active genital herpes infection
Floating fetus
Unripe cervix
Add oxytocin (Pitocin, Syntocinon) to IV fluid.
Piggyback at the lowest port on the primary IV line.
Using the lowest port ensures that very little Pitocin will be in the primary line if an
emergency requires discontinuation of the drug.
Begin infusion slowly and increase at 20- to 30-minute increments until contractions occur
every 2 to 3 minutes, are 40 to 60 seconds in duration, and are firm.
The goal of oxytocin administration is to produce acceptable uterine contractions.
Use external or internal fetal monitoring, continuously monitor the following:
FHR
Uterine resting tone
Contraction frequency, duration, and strength
o Women with previous uterine scars are prone to uterine rupture, especially if oxytocin or forceps
are used. If a woman complains of a sharp pain accompanied by the abrupt cessation of
contractions, suspect uterine rupture, a medical emergency. Immediate surgical delivery is indicated
to save the fetus and the mother.
o The uterus is most sensitive to becoming tetanic at the beginning of the infusion. The client must
always be attended and contractions monitored. Contractions should last no longer than 90 seconds
to prevent fetal hypoxia.
o The major goal of nursing care for a client with preeclampsia is to maintain uteroplacental
perfusion and prevent seizures. This requires the administration of magnesium sulfate. Withhold
administration of magnesium sulfate if signs of toxicity exist: respirations <12/min, absence of
DTRs, or urine output <30 mL/hr.
o Rarely are antihypertensive drugs used in the preeclamptic client. They are given only in the event
of diastolic BP above 110 mm Hg (danger of stroke). The drug of choice is hydralazine HCl
(Apresoline).
o Although delivery is often described as the “cure” for preeclampsia, the client can convulse up to 48
hours after delivery.
o Nursing care during labor and delivery for the client with cardiac disease is focused on prevention
of cardiac embarrassment, maintenance of uterine perfusion, and alleviation of anxiety.
o Should these clients experience preterm labor, the use of beta-adrenergic agents such as terbutaline
(Brethine) and ritodrine HCl (Yutopar) is contraindicated because of the risk for myocardial
ischemia.
o Normal diuresis, which occurs in the postpartum period, can pose serious problems to the new
mother with cardiac disease because of the increased cardiac output.
o Coumadin may not be taken during pregnancy due to its ability to cross the placenta and affect the
fetus. Heparin is the drug of choice; it does not cross the placental membrane.
o Research has found that infection by Helicobacter pylori (the bacterium that causes stomach ulcers)
is another possible causative factor in hyperemesis. Other pregnancy and nonpregnancy risk
factors for hyperemesis gravidarum include first pregnancy, multiple fetuses, age under 24, history
of this condition in other pregnancies, obesity, and high-fat diets.o In severe cases of hyperemesis gravidarum, the health care provider may prescribe antihistamines,
vitamin B6, or phenothiazines to relieve nausea. The provider may also prescribe metoclopramide
(Reglan) to increase the rate at which the stomach moves food into the intestines or antacids to
absorb stomach acid and help prevent acid reflux.
o Women who suffer from hyperemesis gravidarum are often deficient in thiamin, riboflavin, vitamin
B6, vitamin A, and retinol-binding proteins.
o Glucose Screen
Client does not have to fast for this test; 50 g of glucose is given and blood is drawn after 1
hour. If the blood glucose is greater than 140 mg/dL, a 3-hour glucose tolerance test (GTT)
is done.
o A higher incidence of fetal anomalies occurs in pregnant women with diabetes. Therefore, fetal
surveillance is very important:
Ultrasound examination
Alpha-fetoprotein (to determine neural tube anomalies)
Nonstress and contraction stress tests
o Oral hypoglycemics are not taken during pregnancy because of the potential teratogenic effects on
the fetus. Insulin is used for therapeutic management.
o When a pregnant woman is admitted with a diagnosis of diabetes mellitus:
She is more prone to preeclampsia, hemorrhage, and infection.
Most diabetic pregnancies are allowed to progress to term (38 to 40 weeks’ gestation) as
long as metabolic control is maintained and fetal growth is within standards.
o It is useful to discontinue long-acting insulin administration on the day before delivery is planned
because insulin requirements are less during labor and drop precipitously after delivery.
o Estrogen-containing birth control pills affect glucose metabolism by increasing resistance to
insulin. Use of an intrauterine device may be associated with an increased risk for infection in these
already vulnerable women.
o If a woman is medicated, the responsible adult accompanying her must sign the necessary consent
forms. State laws differ as to the acceptability of a friend signing the consent form rather than a
relative.
o Babies delivered abdominally miss out on the vaginal squeeze and are born with more fluid in their
lungs, predisposing them to transient tachypnea (TTN) and respiratory distress.
o The preferable low-transverse uterine incision usually results in less postoperative pain, less
bleeding, and fewer incidents of ruptured uterus. The classical vertical incision of the uterus may
involve part of the fundus, resulting in more postoperative pain, more bleeding, and an increased
chance for uterine rupture.
o Due to the exploration and cleansing of the uterus just after delivery of the placenta, the amount of
lochia may be scant in the recovery room. However, pooling in the vagina and uterus while on bed
rest may result in blood running down the client’s leg when she first ambulates. Cesarean birth
clients have the same lochial changes, placental site healing, and aseptic needs as do vaginal birth
clients.
o A laparotomy of any kind, including cesarean birth, predisposes the client to postoperative
paralytic ileus. When the bowel is manipulated during surgery, it ceases peristalsis, and this
condition may persist. Symptoms include absent bowel sounds, abdominal distention, tympany on
percussion, nausea and vomiting, and of course, obstipation (intractable constipation). Early
ambulation is an effective nursing intervention.
Postpartum High-Risk Disorders
o A nurse must be especially supportive of a postpartum client with infection because it usually
implies isolation from newborn until organism is identified and treatment begun. Arrange phone
calls to nursery and window viewing. Involve family, spouse, and significant others in teaching, and
encourage other family members to continue neonatal attachment activities.
o The most common iatrogenic cause of a UTI is urinary catheterization. Encourage clients to void
frequently and not ignore the urge. IV antibiotics are usually administered to clients with
pyelonephritis.
o Remember, the risk for postpartum infections is higher in clients who experienced problems during
pregnancy (e.g., anemia, diabetes) and who experienced trauma during labor and delivery.o In most cases, a mother who is on antibiotic therapy can continue to breastfeed unless the health
care provider thinks the neonate is at risk for sepsis by maternal contact. Sulfa drugs are used
cautiously in lactating mothers because they can be transferred to the infant in breast milk.
o Many times mastitis can be confused with a blocked milk sinus, which is treated by nursing closer
to the lump and by rotating the baby on the breast. Breastfeeding is not contraindicated for women
with mastitis unless pus is in the breast milk or the antibiotic of choice is harmful to the infant. If
either of these occurs, milk production can still be fostered by manual expression.
o During medical emergencies such as bleeding episodes, clients need calm, direct explanations and
assurance that all is being done that can be done. If possible, allow support person at bedside.
o Risk factors for hemorrhage include dystocia, prolonged labor, overdistended uterus, abruptio
placentae, and infection.
o What immediate nursing actions should be taken when a postpartum hemorrhage is detected?
Perform fundal massage.
Notify the health care provider if the fundus does not become firm with massage.
Count pads to estimate blood loss.
Assess and record vital signs.
Increase IV fluids (additional IV line may be indicated).
Administer oxytocin infusion as prescribed.
Newborn High-Risk Disorders
o “Jitteriness” is a clinical manifestation of hypoglycemia and hypocalcemia. Laboratory analysis is
indicated to differentiate between the two causes.
o To avoid metabolic problems brought on by cold stress, the first step and number one priority in
managing the newborn is to prevent loss of body heat; that is followed by the ABCs. Neonates
produce heat by nonshivering thermogenesis, which involves the burning of brown fat. The neonate
is easily stressed by hypothermia and develops acidosis as a result of hypoxia. Prevent chilling
(keep under radiant warmer or in isolette). If an infant is cold, the first signs exhibited are
prolonged acrocyanosis, skin mottling, tachycardia, and tachypnea. If an infant is cold-stressed,
warm slowly over 2 to 4 hours because rapid warming may produce apnea. A neonate needs
glucose; he or she has little glycogen storage and needs to be fed.
o The lower the score on the Silverman-Anderson Index of Respiratory Distress, the better the
respiratory status of the neonate. A score of 10 indicates that a newborn is in severe respiratory
distress. This is the exact opposite of the method used for Apgar scoring.
o Watch a newborn’s Hct. It is difficult to oxygenate either an anemic newborn (lack of oxygencarrying capacity) or a newborn with polycythemia (Hct >80%, thick, sluggish circulation).
o The PO2 should be maintained between 50 and 90 mm Hg. PO2 <50 signifies hypoxia; PO2 >90
signifies oxygen toxicity problems.
o Antibiotic dosage is based on the neonate’s weight in kilograms. Peak and trough drug levels are
drawn to evaluate whether therapeutic drug levels have been achieved. Closely monitor the
neonate for adverse effects of all drugs.
o Sepsis can be indicated by both a temperature increase and a temperature decrease.
o Gavage Feeding: Newborn Client
Gather equipment: sterile feeding tube (5 to 8 Fr); calibrated syringe for formula;
stethoscope; sterile syringe without needle; paper tape; formula; and medications, if
prescribed.
Position newborn with head slightly elevated and towel under shoulders.
Measure distance from bridge of the infant’s nose to the earlobe and then to a point halfway
between the xiphoid process and the umbilicus.
Pass tube along back of tongue, advancing as newborn swallows.
Test placement:
Inject 0.5 mL air using a sterile syringe while simultaneously listening for air
“bubble” into stomach with stethoscope over epigastrium.
Aspirate a small amount of stomach contents and check pH to verify gastric contents
(<3).
Aspirate and measure any residual stomach contents and reduce volume of feeding by
amount of residual obtained (if health care provider so prescribes). Attach large feeding syringe to tube with plunger removed; pour in warmed formula or
breast milk and allow to flow by gravity. Hold 6 to 8 inches above newborn’s head for slow
feeding: 20 minutes or 1 mL/min.
Stop flow at neck of syringe by pinching tubing.
Clear tubing with small amount of sterile water (1 to 2 mL).
Pinch tubing and withdraw quickly to avoid administering the feeding nasopharyngeally.
Infant may be burped.
Position infant on right side to minimize possibility of regurgitation and aspiration.
Postpone any treatments for 1 hour so feeding is retained.
Record amount of residual, the type and amount of the feeding, the time the feeding
was started and the time the feeding ended, and the newborn’s response to the
feeding.
o Total Parenteral Nutrition
Solutions are administered via a central intravenous access site or a peripherally inserted
central venous catheter (PICC).
Potential complications associated with total parenteral nutrition (TPN) include
hyperglycemia, electrolyte imbalance, infection, and dehydration.
o Emotional Aspects Related to Care of High-Risk Neonates
Without adequate attention to the emotional and developmental needs of the sick neonate,
the following may occur:
Failure to thrive (slow or absent growth)
Avoidance of eye contact with people
Absent or weak crying; infant is trying to say, “I give up.”
A baby who has been overstimulated with procedures or activities will need time out from
interaction.
Sick neonates need developmentally appropriate stimulation and may need the services of
occupational and physical therapists for developmental assessment and intervention.
Nurses may cuddle, swaddle, sing to, and offer pacifiers to infant and may put mobiles and
decals in crib if baby is not on minimal-stimulation protocol to prevent IVH.
o Drugs used to treat neonatal infections can be ototoxic and nephrotoxic. Close monitoring of
therapeutic levels and observation for side effects are required.
o Renal immaturity in a preterm infant makes the monitoring of the administration of IV fluids and
drug therapy crucial. Closely monitor BUN and creatinine levels when administering the -mycin
antibiotics to treat infections in a neonate.
o To assess for skin jaundice, apply pressure with thumb over bony prominences to blanch skin. After
thumb is removed, the area will look yellow before normal skin color reappears. The best areas for
assessment are the nose, forehead, and sternum. In dark-skinned infants, observe conjunctival sac
and oral mucosa.
o Lab tests measure total and direct (conjugated, excretable, non–fat-soluble) bilirubin levels. The
dangerous bilirubin is the unconjugated, indirect (fat-soluble) type, which is measured by
subtracting the direct from the total bilirubin.
o Maintenance of hydration is crucial for all infants. A preterm infant is already at risk for fluid and
electrolyte imbalances caused by increased body surface area resulting from extended body
positioning and larger body area in relation to body weight. Phototherapy treatment for
hyperbilirubinemia increases the risk for dehydration.
Psychiatric
Therapeutic Communication and Treatment Modalities
o The purpose of therapeutic interaction with clients is to allow them the autonomy to make choices
when appropriate. Keep statements value-free, advice-free, and reassurance-free. Remember, just
the facts! No opinions!
o What action should the nurse take in a psychiatric situation when the client describes a physical
problem? Assess, assess, assess! If a client in the psychiatric unit with paranoid schizophrenia
complains of chest pain, take his or her BP. If the obstetrical client who has delivered a dead fetuscomplains of perineal pain, look at the perineal area (she may have a hematoma). Just because the
focus of the client’s situation is on his or her psychological needs, it does not mean that the nurse
can ignore physiologic needs.
o Basic communication principles can be applied to all clients:
Establish trust.
Demonstrate a nonjudgmental attitude.
Offer self; be empathetic, not sympathetic.
Use active listening.
Accept and support client’s feelings.
Clarify and validate client’s statements.
Use matter-of-fact approach.
o Remember, a nurse’s nonverbal communication may be more important than the verbal
communication.
o A question concerning nurse–client confidentiality appears often on the NCLEX-RN. For the nurse to
tell a client that he or she will not tell anyone about their discussion puts the nurse in a difficult
position. Some information must be shared with other team members for the client’s safety (e.g.,
suicide plan) and optimal therapy.
o Nausea is a common complaint after ECT. Vomiting by an unconscious client can lead to aspiration.
Because post-ECT clients are unconscious, the nurse must observe closely for the possibility of
aspiration: maintain a patent airway!
Preparing client for ECT Give accurate, nonjudgmental information about the treatment.
Explore client’s concerns. Check emergency equipment. Be sure suction equipment and O2
are available.
Nursing interventions during/after ECT Maintain patent airway. Check vital signs every
15 minutes until client is alert. Remain with client following treatment until client is
conscious. Reorient if client is confused.
Anxiety Disorders
o Common physiologic responses to anxiety include increased heart rate and blood pressure; rapid,
shallow respirations; dry mouth and tight feeling in throat; tremors and muscle tension; anorexia;
urinary frequency; and palmar sweating.
o Anxiety is very contagious and is easily transferred from client to nurse and from nurse to client.
First, the nurse must assess his or her own level of anxiety and remain calm. A calm nurse helps the
client to gain control, decrease anxiety, and increase feelings of security.
o When a client describes a phobia or expresses an unreasonable fear, the nurse should acknowledge
the feeling (fear) and refrain from exposing the client to the identified fear. After trust is
established, a desensitization process may be prescribed. Desensitization is the nursing
intervention for phobia disorders. The nurse should:
Assist client to recognize the factors associated with feared stimuli that precipitate a phobic
response.
Teach and practice with client alternative adaptive coping strategies, such as the use of
thought substitution (replacing a fearful thought with a pleasant thought) and relaxation
techniques. (Role-playing is useful when the client is in a calm state.)
Expose client progressively to feared stimuli, offering support with the nurse’s presence.
Provide positive reinforcement whenever a decrease in phobic reaction occurs.
Note: In all likelihood, the desensitization process will be overseen by a mental health
practitioner (nurse practitioner), or psychologist.
o The nurse should place an anxious client where there are reduced environmental stimuli (a quiet
area of the unit, away from the nurses’ station).
o The best time for interaction with a client is at the completion of the performed ritual. The client’s
anxiety is lowest at this time; therefore, it is an optimal time for learning.
o Compulsive acts are used in response to anxiety, which may or may not be related to the obsession.
It is the nurse’s responsibility to help alleviate anxiety.
o Interfering will increase anxiety. These acts should be allowed as long as the client’s acts are free of
violence. The nurse should:
Actively listen to the client’s obsessive themes. Acknowledge the effects that ritualistic acts have on the client.
Demonstrate empathy.
Avoid being judgmental.
o For clients with posttraumatic stress disorder, the nurse should:
Actively listen to client’s stories of experiences surrounding the traumatic event.
Assess suicide risk.
Assist client to develop objectivity about the event and problem-solve regarding possible
means of controlling anxiety related to the event.
Encourage group therapy with other clients who have experienced the same or related
traumatic events.
Somatoform Disorders
o Be aware of your own feelings when dealing with this type of client. It is a challenge to be
nonjudgmental. The pain is real to the person experiencing it. These disorders cannot be explained
medically; they result from internal conflict. The nurse should:
Acknowledge the symptom or complaint.
Reaffirm that diagnostic test results reveal no organic pathology.
Determine the secondary gains acquired by the client.
o The primary gain is a decrease in anxiety that results from some effort made to deal with stress.
The secondary gain is the advantage, other than reduced anxiety, that occurs as a result of the sick
role.
o The term somatization is used to describe a person who has many recurrent complaints with no
organic basis; a person with hypochondriasis has unrealistic or exaggerated physical complaints.
The concerns of those who are experiencing somatization and of those who are hypochondriacal
are so exaggerated that they interfere with social and occupational functioning.
o Types of Somatoform Disorders
Somatization disorder
Recurrent somatic complaints for which frequent medical attention is sought but no
medical pathology is present
Example: a client who complains of chest pains but has a normal ECG and normal
cardiac enzymes
Nursing care: evaluate pain medication use or abuse; document duration and
intensity of pain; assist client to identify precipitating factors related to request for
medication.
Hypochondriasis
The belief in and fear of having a disease, including misinterpretation of physical
signs as “proof” of the presence of the disease
Example: A client has a rash that is quite minor but insists that he has a serious
disease such as lupus.
Nursing care: each relaxation techniques, explore relationship between the
symptoms and past experiences with the disease, focus interactions away from
bodily concerns.
Conversion disorder
A disorder characterized by transferring a mental conflict into a physical symptom
for which there is no organic cause
Examples: blindness, paralysis, seizures, deafness, and pseudocyesis (false
pregnancy)
Nursing care: assist with ADLs, encourage expression of anger, teach relaxation
techniques, and assist with the identification of anxiety related to job security and
performance.
Dissociative Disorders
o The nurse should be aware that all behavior has meaning.
o Avoid giving clients with dissociative disorders too much information about past events at one
time. The various types of amnesia that accompany dissociative disorders provide protection from
pain. Too much, too soon may cause decompensation.
o Psychogenic amnesia is the sudden inability to recall certain events in one’s life. A psychogenicfugue state is characterized by the individual’s leaving home and being unable to recall his or her
identity or past.
o Multiple personality disorder = The presence of two or more distinct personalities within an
individual; the personalities emerge during stress.
o Depersonalization disorder = A temporary loss of one’s reality; a loss of the ability to feel and
express emotions; a sense of “strangeness” in the surrounding environment; individuals with this
disorder express a fear of “going crazy.”
Personality Disorders
o Personality disorders are long-standing behavioral traits that are maladaptive responses to anxiety
and that cause difficulty in relating to and working with other individuals. NCLEX-RN® questions
sometimes test personality disorder content by describing management situations.
o Persons with personality disorders are usually comfortable with their disorders and believe that
they are right and the world is wrong. These individuals usually have very little motivation to
change. Think of them as a challenge!
o Types
Obsessive-compulsive = Orderly, rigid
Antisocial = Unable to conform to social norms
Borderline = Needy, always in a crisis, self-mutilating, unable to sustain relationships,
splitting behavior
Dependent = Unable to make decisions for self, allows others to assume responsibility for
his or her life
Narcissistic = Feelings of self-importance and entitlement; may exploit others to get own
needs met
Histrionic = Dramatic, flamboyant, needs to be the center of attention
Paranoid = Suspicious, mistrusts others, is watchful and secretive
Schizoid = Isolated and introverted, no close friends
Maladaptive = Nothing he or she does is wrong (e.g., authorities are “out to get me”)
Eating Disorders
o People with anorexia gain pleasure from providing others with food and watching them eat. These
behaviors reinforce their perception of self-control. Do not allow these clients to plan or prepare
food for unit-based activities.
o Individuals with bulimia often use syrup of ipecac to induce vomiting. If ipecac is not vomited and is
absorbed, cardiotoxicity may occur and can cause conduction disturbances, cardiac dysrhythmias,
fatal myocarditis, and circulatory failure. Because heart failure is not usually seen in this age group,
it is often overlooked. Assess for edema and listen to breath sounds.
o Physical assessment and nutritional support are a priority; the physiologic implications are great.
Nursing interventions should increase self-esteem and develop a positive body image. Behavior
modification is useful and effective. Family therapy is most effective because issues of control are
common in these disorders. (Therapy is usually long term.)
o Clinical S&S of anorexia = Weight loss of at least 15% of ideal or original body weight; hair loss; dry
skin; irregular heart rate; decreased pulse; decreased BP; amenorrhea; dehydration; electrolyte
imbalance
o Anorexia nervosa deals with issues of control and a struggle between dependence and
independence. Bulimia deals with loss of control (binge eating) and guilt (purging).
o Initial treatment for client admitted with Bulimia Blood work to evaluate electrolyte status;
replenishment of electrolytes and fluids as indicated; careful monitoring for evidence of vomiting
Mood Disorders
o The most important signs and symptoms of depression are a depressed mood with a loss of interest
in the pleasures in life. The client has sustained a loss. Other symptoms include:
Significant change in appetite, often accompanied by a change in weight, either weight loss
or gain
Insomnia or hypersomnia (usually sleeping during the day, often because the client is not
sleeping at night due to anxiety)
Fatigue or lack of energy
Feelings of hopelessness, worthlessness, guilt, or overresponsibility Loss of ability to concentrate or think clearly
Preoccupation with death or suicide
o Depressed clients have difficulty hearing and accepting compliments because of their lowered selfconcept. Comment on signs of improvement by noting the behavior (e.g., “I notice you combed your
hair today” not, “You look nice today”).
o The nurse knows depressed clients are improving when they begin to take an interest in their
appearance or begin to perform self-care activities that were previously of little or no interest to
them.
o MAOIs (antidepressant)
Must not be used with tricyclics (cause hypertensive crisis)
Major concern is need for dietary restrictions—certain drug and food interactions can cause
hypertensive crisis.
Instruct client not to eat foods with high tyramine content: aged cheese, red wine, beer, beef
and chicken, liver, yeast, yogurt, soy sauce, chocolate, bananas.
May not be used with SSRIs
Teach client not to take over-the-counter drugs without physician approval.
Teach the warning signs of hypertensive crisis: headaches, palpitations, increased BP.
o Trycyclics (antidepressant)
Administer at bedtime to minimize sedative effect.
Takes 2-6 weeks to achieve therapeutic effects
1-3 weeks should elapse between discontinuing tricyclics and initiating MAO inhibitors.
Teach client to avoid alcohol.
Avoid concurrent use of antihypertensive drugs.
Carefully evaluate suicide risk.
Lethal in overdose
o SSRIs (antidepressant)
Effective 2-4 weeks after treatment is initiated
Should not be used with MAO inhibitors: cause hypertensive crisis (violent reaction)
Should wait at least 14 days between discontinuing MAO inhibitor and starting Prozac
At least 5 weeks should lapse between discontinuing Prozac and initiating an MAO inhibitor.
May be given in evening if sedation occurs
Monitor for serotonin syndrome (defined by at least 3 symptoms):
Rapid onset of altered mental states
Agitation
Myoclonus
Hyperreflexia
Fever
Shivering
Diaphoresis
Ataxia
Diarrhea
Caution client about OTC use of St. John’s Wort.
Must be tapered slowly if discontinuing or changing from one SSRI to another
o The nurse should suspect an imminent suicide attempt if a depressed client becomes “better” (i.e.,
happy or even elated). Be aware: a happy affect may signify that the client feels relieved that a plan
has been made and is prepared for the suicide attempt.
o When dealing with a depressed client, the nurse should assist with personal hygiene tasks and
encourage the client to initiate grooming activities even when he or she does not feel like doing so.
This helps promote self-esteem and a sense of control.
o An important nursing intervention for the depressed client is to sit quietly with the client. When
answering NCLEX-RN questions, remember that you are working at Utopia General and there is
plenty of time and staff to provide ideal nursing care. Do not let the realities of clinical situations
deter you from choosing the best nursing intervention. The best intervention is to sit quietly with
the client, offering support with your presence.
o There are always questions about drugs on the NCLEX-RN. Here are some tips: Know the common side effects of drug groups.
Antianxiety drugs: sedation, drowsiness
Antidepressant drugs: anticholinergic effects, postural hypotension
MAO inhibitors: hypertensive crisis
Know specific problems and concerns in drug therapy.
Lithium requires renal function assessment and monitoring.
Phenothiazines (antipsychotic) cause extrapyramidal effects (EPS); tardive
dyskinesia can be permanent if client is not assessed regularly for signs of tardive
dyskinesia!
Know specific client teachings about drug therapy.
Phenothiazines cause photosensitivity, so client must wear protective clothing and
sunglasses.
MAO inhibitors require dietary restrictions to prevent hypertensive crisis.
o Monitor serum lithium levels carefully. The therapeutic and toxic levels are very close to each other
on the readings. Signs of toxicity are evident when lithium levels are more than 1.5 mEq/L. Blood
levels should be drawn 12 hours after last dose.
o Manic clients can be very caustic toward authority figures. Be prepared for personal putdowns.
Avoid arguing or becoming defensive.
o What activities are appropriate for a manic client? Noncompetitive physical activities that require
the use of large muscle groups.
o Where should a manic client be placed on the unit?
Make every attempt to reduce stimuli in the environment. Place the client in a quiet part of
the unit.
o What interventions should the nurse use if a client becomes abusive?
Redirect negative behavior or verbal abuse in a calm, firm, nonjudgmental, nondefensive
manner.
Suggest a walk or other physical activity.
Set limits on intrusive behavior. For example, “When you interrupt, I cannot explain the
procedure to the others; please wait your turn.”
If necessary, seclude or administer medication if client becomes totally out of control.
Always remember to use compassion because nurses are “nice” people.
o Lithium (mood stabilizer)
Lithium is excreted by the kidney. Maintain adequate serum levels.
Assess electrolytes, especially sodium.
Baseline studies of renal, cardiac and thyroid status must be obtained before lithium
therapy is begun.
Teach client early symptoms of lithium toxicity. If drug is continued, coma, convulsions, and
death may occur.
Instruct client to keep salt usage consistent.
Use with diuretics is contraindicated. Diuretic-induced sodium depletion can increase
lithium levels, causing toxicity
o Valproic acid/Depakene (anticonvulsant mood stabilizer)
Administer with food.
Monitor blood levels.
Maintain serum levels 50-125 µg/mL.
o Carbamazepine/Tegretol (anticonvulsant mood stabilizer)
Maintain serum levels at 8-12 g/mL.
Stop drug if WBC drops below 3000/mm3 or neutrophil count goes below 1500/mm3.
Monitor hepatic and renal function.
o Lamotrigine/Lamictal (anticonvulsant mood stabilizer
To minimize risk of severe rash, give low dosage, 25-50 mg/day initially, then gradually
increase to maintenance dose of 200 mg/day (used alone) or 100 mg/day (with Valproate)
or 400 mg/day (with Carbamazepine).
o Component of a suicide assessment: Existence of a plan, existence of a method, availability of
method chosen, lethality of method chosen, identified support system, and history of previousattempts
Thought Disorders
o When evaluating client behaviors, consider the medications the client is receiving. Exhibited
behaviors may be manifestations of schizophrenia or a drug reaction.
o There are five types of schizophrenia specified in the DSM-IV-TR, which is a diagnostic manual
prepared by the American Psychiatric Association that provides diagnostic criteria for all
psychiatric disorders.
o Use Bleuler’s four A’s to help remember the important characteristics of schizophrenia:
Autism (preoccupied with self)
Affect (flat)
Associations (loose)
Ambivalence (difficulty making decisions)
o Client is Delusional
Encourage recognition of distorted reality
Divert focus from delusional thought to reality; do not permit rumination on false ideas.
Do not agree with or support delusions.
Avoid arguing about the delusion. Be very matter-of-fact.
Avoid physically touching client, especially if delusions are persecutional.
Administer antipsychotic drugs
Monitor and treat side effects of psychotropic drugs
Administer antiparkinsonian drugs
o Client is Hallucinating
Protect client from injury that might result from responding to commands of the voices; pay
attention to the content.
Avoid denying or arguing with client about the hallucination.
Discuss your observations with client (e.g., “You appear to be listening to something.”)
Make frequent but brief remarks to interrupt the hallucinations.
Administer antipsychotic drugs
Monitor and treat side effects of psychotropic drugs
Administer anticholinergic drugs
o Side effects of Antipsychotics
Blood Dyscrasias
Agranulocytosis: occurs in first weeks of treatment
o Sore throat, fever, chills
o Protect from infections
o Provide comfort measures: gargle for sore throat, use logenzes and
analgesics
Thrombocytopenia: decreased platelets
o Bruises easily, petechial
o Teach client safety measures (r/f bleeding)
Extrapyramidal Effects
Parkinsonism: occurs within 1-4 weeks after initiation of treatment
o Rigidity, shuffling gait, pill-rolling hand movements, tremors, dyskinesia,
masklike face
Akathisia: occurs within 1-6 weeks after initiation of treatment
o Restlessness, agitation, and pacing; sudden difficulty sitting still (can be
confused with tardive dyskinesia)
Dystonia: occurs within 1-2 days after initiation of treatment
o Limb and neck spasms; uncoordinated, jerky movements; difficulty speaking
and swallowing; rigidity and muscle spasms
Tardive dyskinesia: develops late in treatment
o Involuntary tongue and lip movements; blinking, choreiform movements of
limbs and trunk
Photosensitivity
Teach to stay out of sun, wear protective clothing/sunglasses Neuroleptic Malignant Syndrome
Life-threatening emergency: high fever, tachycardia, stupor, increased respirations,
severe muscle rigidity
Anticholinergic Effects
Dry mouth, blurred vision, tachycardia, nasal congestion, constipation, urinary
retention, orthostatic hypotension
o Observe for increased motor activity and/or erratic response to staff and other clients. The client
may be experiencing an increase in command hallucinations. When this occurs, there is an
increased potential for aggressive behavior.
o Do not argue with a client about the delusions. Logic does not work; it only increases the client’s
anxiety. Be matter-of-fact and divert delusional thought to reality. Trust is the basis for all
interactions with these clients. Be supportive and nonjudgmental. Stress increases anxiety and the
need for delusions and hallucinations. Do not agree that you hear voices (you should be the client’s
contact with reality), but acknowledge your observation of the client; for example, “You look like
you’re listening to something.”
Substance Abuse
o What medications can the nurse expect to administer to chemically dependent clients? In treating
alcohol withdrawal, Librium or Ativan are commonly used. Antabuse is often used as a deterrent to
drinking alcohol. Client teaching should include the effects of consuming any alcohol while on
Antabuse. Encourage client to read all labels of over-the-counter medications and food products
that may contain small amounts of alcohol.
o Alcohol Deterrents
Disulfiram (Antabuse)
Treatment of alcoholism; aversion therapy
Interferes with breakdown of alcohol causing an accumulation of acetaldehyde (a
byproduct of alcohol in the body)
Severe side effects occur if alcohol is consumed:
o Nausea and vomiting
o Hypotension, headaches
o Rapid pulse and respirations
o Flushed face and bloodshot eyes
o Confusion
o Chest pain
o Weakness, dizziness
o Teach client what to expect if alcohol is consumed while taking the drug.
Be aware that some alcoholic clients use the side effects as a means of “punishing”
themselves or as a form of masochism, and if a client repeatedly consumes alcohol
while taking the drug, the health care provider should be notified.
Persons with serious heart disease, diabetes, epilepsy, liver impairment, or mental
illness should not take Antabuse.
Use in motivated clients who have shown the ability to stay sober.
o What type of therapy is used with chemically dependent clients? Group therapy is effective, as are
support groups such as Alcoholics Anonymous and Narcotics Anonymous.
o Harm reduction is a community health strategy designed to reduce the harm of substance abuse to
families, individuals, community, and society. Examples: More compassionate drug treatment
options, including abstinence and drug-substitution models; HIV-related interventions such as
needle exchanges; directed drug-use management should the client wish to continue use; changes
in laws concerning possession of paraphernalia and drug use.
o Drug Withdrawal and Overdose Symptoms
Heroin, Morphine, Codeine, Opium, Methadone
Withdrawal
o Watery eyes, runny nose, dilated pupils
o Anxiety
o Diaphoresis, fever
o Nausea, vomiting, and diarrheao Achiness
o Abdominal cramps
o Insomnia
o Tachycardia
Overdose
o Dilated pupils
o Respiratory depression leading to respiratory arrest
o Circulatory depression leading to cardiac arrest
o Unconsciousness leading to coma
o Death
Cocaine
Withdrawal
o Depression
o Fatigue
o Disturbed sleep
o Anxiety
o Psychomotor agitation
Overdose
o Tachycardia
o Pupillary dilatation
o Increased BP
o Cardiac arrhythmias
o Perspiration, chills
o Nausea, vomiting
Amphetamines
Withdrawal
o Depression
o Fatigue
o Disturbed sleep
Overdose
o Restlessness
o Tremors
o Rapid respiration
o Confusion
o Assaultive behavior
o Hallucinations
o Panic
Benzodiazapines (Valium, Serax, Ativan)
Withdrawal
o Tremors
o Agitation
o Anxiety
o Abdominal cramps
o Nausea and vomiting
o Grand mal seizures
Overdose
o Drowsiness
o Confusion
o Hypotension
o Convulsion
o Shock
o Coma → death
o Know what defense mechanisms are used by chemically dependent clients. Denial and
rationalization are the two most common coping styles used. Their use must be confronted so the
client’s accountability for his or her own behavior can be developed.o What basic needs take priority when working with chemically dependent clients? Nutrition is a
priority. Alcohol and drug intake has superseded the intake of food for these clients.
o What behaviors are expected during withdrawal? In the alcoholic, DTs occurs 12 to 36 hours after
the last intake of alcohol. Know the symptoms. In drug abuse, withdrawal symptoms are specific to
the type of drug.
Abuse
o Select only one nurse to care for an abused child. Abused children have difficulty establishing trust.
The child will be less anxious with one consistent caregiver.
o Women who are abused may rationalize the spouse’s behavior and unnecessarily accept blame for
his actions. The woman may or may not choose to press charges. Be sure to give her the number of
a shelter or help line for future occurrences and help her to develop a safety plan.
o It is difficult for an elderly person to admit abuse for fear of being placed in a nursing home or being
abandoned. Therefore, it is imperative to establish a trusting relationship with the elderly client.
o Rape victims are at high risk for posttraumatic stress disorder (PTSD). Immediate intervention to
diminish distress is vital. The nurse should also assess for and intervene for sequelae such as
unwanted pregnancy, sexually transmitted diseases, and HIV risk.
o Questions on the NCLEX-RN exam regarding physical and sexual abuse usually focus on three
aspects:
Physical manifestations of abuse
Client safety
Legal responsibilities of the nurse. For children, the nurse is legally responsible for
reporting all suspected cases of abuse. In intimate-partner abuse, it is the adult’s decision;
the nurse should be supportive of the decision. Remember to document objective factual
assessment data and the client’s exact words in cases of sexual abuse and rape.
o All cases of suspected abuse must be reported to appropriate local and state agencies. Take color
photographs of injuries. Document factual, objective statements of the child’s physical condition,
child–family interactions, and interviews with family. Establish trust, and care for the child’s
physical problems. These are the primary and immediate needs of these children. Recognize own
feelings of disgust and contempt for the parents. Teach basic child development and parenting skills
to family.
o With a rape survivor Communicate nonjudgmental acceptance. Provide physical care to treat
injuries. Give clear, concise explanations of all procedures to be performed. Notify police; encourage
victim to prosecute. Collect and label evidence carefully in the presence of a witness. Document
factual, objective statements about physical condition. Record client’s exact words in describing the
assault. Notify rape crisis team or counselor if available in the community. Allow discussion of
feelings about the assault. Advise of potential for venereal disease, HIV, or pregnancy, and describe
medical care available.
Organic Disorders
o The basic difference between delirium and dementia is that delirium is acute and reversible,
whereas dementia is gradual and permanent.
o Confusion in older adults is often accepted as being part of growing old. However, the confusion
may be due to dehydration with resulting electrolyte imbalance. Think “sudden change” when
obtaining a history. Such changes are usually due to a specific stressor, and treatment of the
causative stressor will usually result in correcting the confusion.
o Confabulation is not lying. It is used by the client to decrease anxiety and protect the ego.
o Nursing interventions for the confused older adult should focus on:
Maintaining the client’s health and safety
Encouraging self-care
Reinforcing reality orientation (e.g., saying, “Today is Monday,” and calling the client by
name)
Providing a consistent, safe environment; engaging client in simple tasks and activities to
build self-esteem
o Providing a consistent caregiver is a priority in planning nursing care for the confused older client.
Change increases anxiety and confusion.
o For client with Alzheimer’s Disease Provide a safe, consistent environment. (Do not makechanges, if possible. Change increases anxiety and confusion.) Stick to routines. If client wanders,
make sure he or she has a name tag. Provide assistance as needed with ADLs. Make sure bathroom
is clearly labeled.
Childhood and Adolescent Disorders
o Children also experience depression, which often presents as headaches, stomachaches, and other
somatic complaints. Be sure to assess suicide risk, especially in the adolescent.
o The client’s lack of remorse or guilt about the antisocial behavior represents a malfunction of the
superego, or conscience. The id functions on the basic instinct level and strives to meet immediate
needs. The ego is in touch with external reality and is the part of the personality that makes
decisions.
o Important points to remember when answering NCLEX-RN questions:
A child in this situation may be involved in a self-fulfilling prophecy (e.g., “Mom says that I’m
a troublemaker; therefore, I must live up to Mom’s expectations”).
Confront the client with his or her behavior (e.g., lying). This gives the client a sense of
security.
Provide consistent interventions; this helps to prevent manipulation. Inconsistency does
not help the client develop self-control.
o Attention-deficit (hyperactivity) disorder (ADD/ADHD) More prevalent in boys; failure to listen
to or follow instructions; difficulty playing quietly; disruptive behavior; impulsive behavior;
difficulty sitting still; distractibility to external stimuli; excessive talking; shifting from one
unfinished task to another; and underachievement in school performance. Methylphenidate
(Ritalin) to treat.
o Conduct disorder
Risk for violence related to …
Disturbed self-esteem related to …
Ineffective family coping related to …
Assess verbal and nonverbal cues for escalating behavior so as to decrease outbursts. Use a
non-authoritarian approach. Avoid asking “why” questions. Initiate a show of force with a
child who is out of control. Initiate suicide precautions when assessment indicates risk. Use
a quiet room when external control is needed. Clarify expressions or jargon if meanings are
unclear. Teach to redirect angry feelings to a safe alternative, such as a pillow or punching
bag. Implement behavior modification therapy if indicated. Role-play new coping strategies.
Gerontology
Aging
o The ability to perform activities of daily living (ADLs) is a more accurate measure of age than
chronologic age. The concept of aging is shifting from frail and dependent to healthy living.
o The majority of those aged 65 and older regard their health as good or excellent.
o Chronologic age may or may not correspond to physical, mental, social, and cultural actions and
feelings.
Physiologic Changes
o Changes in the heart and lungs result in less efficient utilization of O2, which reduces an individual’s
capacity to maintain physical activity for long periods of time. Physical training for older people can
significantly reduce blood pressure (BP) and increase aerobic capacity. NCLEX-RN® questions may
ask about teaching and designing rehabilitation programs for older adults. The answers should
contain something about exercise and nutrition.
o Older people often complain that they cannot get to sleep at night and do not sleep soundly even
after they fall asleep. This is because they have shorter stages of sleep, particularly shorter cycles
between stages 1 and 4 and REM sleep (stage 4 is deep sleep). They are easily awakened by
environmental stimuli. They often compensate by napping during the day, which leads to further
disruptions of night sleep. A common response is the use of prescription sleeping pills, which can
create still further problems of disorientation, etc.
o Peripheral circulation decreases as one ages. Regular assessment of the feet is very important
because it increases the opportunity to discover and treat skin care problems early. These problemscould become more serious because of decreased circulation.
o Differentiation of normal and pathologic causes for skin and hair conditions is essential; for
example, seborrheic keratosis from melanomas.
o Impaired mobility, impaired skin integrity, decreased peripheral circulation, and a lack of physical
activity place older adults at risk for the development of pressure ulcers.
o The following are ways to help prevent or decrease the occurrence of falls:
Install adequate lighting.
Paint the edges of stairs a bright color.
Place a bell on any resident cats; cats move quickly and can get underfoot.
Wear proper footwear that supports the foot and contributes to balance; shoes should be
made of nonslippery materials.
o Both systolic and diastolic blood pressures tend to increase with normal aging, but the elevation of
systolic is greater. Remember the physiology of blood pressure, which is expressed as a ratio of
systolic to diastolic pressure. Systolic refers to the level of BP during the contraction phase,
whereas diastolic refers to the stage when the chambers of the heart are filling with blood.
o Dysrhythmias in older adults are particularly serious because older people cannot tolerate
decreased cardiac output, which can result in syncope, falls, and transient ischemic attacks (TIAs).
Pulse may be rapid, slow, or irregular.
o Angina symptoms may be absent in older adults or they may be confused with gastrointestinal
symptoms (epigastric pain similar to heartburn).
o With aging, the muscles that operate the lungs lose elasticity so that respiratory efficiency is
reduced. Vital capacity (the amount of air brought into the lungs at one time) decreases. Breathing
may become more difficult after strenuous exercise. The rate of decline has been found to be slower
in more active people. The nurse should encourage older people to remain physically active for as
long as possible.
o Declining muscle strength may impair cough efficiency. This fact makes older people more
susceptible to chronic bronchitis, emphysema, and pneumonia.
o Chronic obstructive pulmonary disease (COPD) is the major cause of respiratory disability in older
adults. Aspiration pneumonia is a major cause of death in older adults.
o The following are changes that contribute to chronic constipation with age:
The number of enzymes in the small intestine is reduced, and simple sugars are absorbed
more slowly, resulting in decreased efficiency of the digestive process.
The smooth-muscle content and the muscle tone of the wall of the colon decrease. Anatomic
changes in the large intestine result in decreased intestinal motility.
Psychological factors, as well as abuse of over-the-counter laxatives, are factors.
Decreases in fluid intake and mobility contribute to constipation.
o Tooth loss is not a normal aging process. Good dental hygiene, good nutrition, and dental care can
prevent tooth loss.
o Older people may appear to eat small quantities of food at mealtimes. This is because the digestive
system of older people features a decrease in the contraction time of the muscles, and more time is
needed for the cardiac sphincter to open. Therefore, it takes more time for the food to be
transmitted to the stomach. Thus, the sensation of fullness may occur before the entire meal is
consumed.
o Poor nutrition or malnutrition are significant concerns in the older adult. Some reasons for poor
nutrition include chronic illness, which suppresses appetite, hospitalization and surgery, difficulty
chewing, alcohol use, cognitive changes, depression, grief, loneliness, social isolation, and problems
with food procurement. An early sign of malnutrition may be changes in weight.
o Older people have a higher risk for the development of renal failure because normal age-related
changes result in compromised renal functioning. The nurse should pay careful attention to urinary
output in older clients because it is the first sign of loss of renal integrity.
o Kegel exercises consist of tightening and relaxing the vaginal and urinary meatus muscles. These
exercises have been very successful in reducing the incidence of incontinence. They must be done
consistently, and they can be done unobtrusively at home.
o Older adults with incontinence may seek isolation, thereby predisposing themselves to loneliness.
o From 15% to 30% of community-based older adults and almost 50% of older adults living innursing homes suffer from difficulties with bladder control. Older people may be more sensitive to
alcohol and caffeine because these substances inhibit the production of antidiuretic hormone
(ADH). An assessment of sensitivity to bladder problems is essential when planning nursing care.
o Medication Alert!
As one ages, the total number of functioning glomeruli decreases until renal function has
been reduced by nearly 50%. This decrease in the filtration efficiency of the kidneys has
grave implications for people who are taking medication. Of particular importance are
penicillin, tetracycline, and digoxin, which are cleared from the bloodstream primarily by
the kidneys. These drugs remain active longer in an older person’s system. Therefore, they
may be more potent, indicating a need to adjust the dose and frequency of administration.
o Older adults who are sexually active are at risk for sexually transmitted diseases, especially if they
seek sexual relations with different partners.
o Normal loss of brain cells is compounded by alcohol, smoking, and breathing polluted air. As a
result, cognitive and safety issues can develop in the older adult. To help accommodate such losses,
the nurse should teach older clients to shop during less crowded times in stores that are familiar to
them, slow down well in advance of traffic signals, stay in the slower lane of the freeway, avoid
freeways during rush hours, and leave for appointments well ahead of time.
o Alzheimer’s disease is the most common irreversible dementia of old age. It is characterized by
deficits in attention, learning, memory, and language skills. Discuss the problems family members
have in dealing with clients with Alzheimer’s disease in relation to the following disease
manifestations:
Depression
Night wandering
Aggressiveness or passiveness
Failure to recognize family members
o The most common endocrine disorders in the older adult are thyroid dysfunction and type 2
diabetes.
o Diminished eyesight results in the following:
A loss of independence (driving and the ability to perform ADLs)
A lack of stimulation
The inability to read
The fear of blindness
o Lower the tone of your voice when talking to an older person who is hearing-impaired. Highpitched tones (e.g., women’s voices) are the first to become difficult to hear; therefore, lowering the
pitch of your voice increases the likelihood that an older person with a hearing loss will be able to
hear you speak.
o Presbycusis (age-related hearing loss) can result in decreased socialization, avoidance of friends
and family, decreased sensory stimulation, and hazardous conditions when driving.
o Frequent touch to decrease the sense of isolation and to compensate for visual and auditory
sensory loss.
o Make the older adult aware that you are going to touch them so they are not startled, or can let you
know if they don’t want you to touch them.
o Be cognizant of cultural differences with direct eye contact, touch, and taste.
o There are many conditions that can imitate dementia in the older adult. A key role of the nurse is to
make a complete assessment to rule out other possible causes of particular behavior, for example,
acute infection (UTI), dehydration (electrolyte imbalance), medication, pain, and metabolic
disorder.
o The major task of old age according to Erikson is to redefine self in relation to a changed role. Those
people who had been in charge of situations most of their lives may now find themselves in
dependent positions.
Psychosocial Changes
o Older people undergo a great many changes, which are usually associated with loss (loss of spouse,
friends, career, home, health, etc.). Therefore, older people are extremely vulnerable to emotional
and mental stress, depression, and substance abuse.
o Integrity vs. despair is Erikson’s final stage of growth and development. Reminiscing is a means ofsetting one’s life in order (accepting life and self), which is the task of this stage, according to
Erikson’s development theory. The goal of this stage is to feel a sense of the meaning of one’s life,
rather than to feel despair or bitterness that one’s life has been wasted. The major task of older
adults is to redefine self in relation to a changed role. Role adjustment is a major task of aging.
Diseases and Conditions in Older Adults
o Delirium
Acute confused state with rapid onset, usually the result of systemic illness or medication
Decreased level of consciousness
Establish a meaningful environment.
Help maintain body awareness.
Help client cope with confusion, delusions, and illusions.
o Dementia
Slow onset of symptoms
Level of consciousness may be intact.
o Cardiac dysrhythmias
Incidence increases with age.
More serious in older adults because of lower tolerance of decreased cardiac output (can
result in syncope, falls, TIAs, and confusion).
Symptoms result from compromised circulation and O2 deficit.
Assess, prevent, and manage dysrhythmias.
Advise smoking cessation.
Encourage exercise and weight control.
o Cataracts
Often a result of normal aging changes
Most common pathologic problem affecting the eyesight of older adults
Treatment is surgical removal.
Teach instillation of eye drops.
Reduce glare in environment.
Assistance is required postoperatively because affected eye is covered, and disorientation
may occur.
o Glaucoma
Risk of acquiring increases with age.
Loss of sensory input can result in confusion.
o Macular degeneration
Principal cause of blindness
Loss of sensory input can result in confusion.
Yearly examination important
o Cerebrovascular accident (CVA)
Interruption of cerebral circulation, caused by occlusion or hemorrhage in the brain
Risk increases with age.
Prevent deterioration of client’s condition.
Maximize functional abilities (occupational therapy).
Assist client in accepting physical deficits.
Check gag reflex before client receives food or fluids.
Prevent injuries to paralyzed limbs.
o Pressure ulcer
Immobility puts older adults at risk.
Reposition frequently.
Massage bony prominences.
Provide adequate nutrition.
o Hypothyroidism
Usually occurs after age 50
Symptoms are often similar to normal aging changes and have an insidious onset, making it
difficult to detect in older adults.
Older adults are at greater risk for development of myxedema coma, which is life-threatening.
Often diagnosed as depression; with treatment, signs of depression disappear.
Caution against abruptly discontinuing medication.
o Thyrotoxicosis (Graves disease)
Symptoms may be absent or attributed to other, more common diseases in older adults.
Weight loss and HF may be predominant symptoms.
It is precipitated by stressful events such as trauma, surgery, or infection. Be alert for signs
and symptoms.
Can be fatal if untreated (Thyroid Storm)
o COPD
A major cause of respiratory disability in older adults
Most older people exhibit both chronic bronchitis and chronic emphysema.
Fatigue is a common result because of the increased work required to breathe (dyspnea).
Encourage to stop smoking.
Keep in mind older person’s state of confusion when teaching about treatment regimen.
Plan rest periods to allow patient to maintain oxygen levels.
o Urinary tract infections (UTIs)
Their incidence increases with age.
Older people are often asymptomatic or exhibit vague, ill-defined symptoms.
With infections, older people often become confused.
Suspect UTI when client’s voiding habits change.
Normal Values
Hematologic
o Hgb (Hemoglobin: g/dL)
Male: 14-18
Female: 12-16
Pregnant: >11 (slight Hgb decreases normally occur during pregnancy)
1-6 yr: 9.5-14
6-18 yr: 10-15.5
Newborn: 14-24
Older adult: Values slightly decreased
High altitude increases values
o Hct (Hematocrit: %)
Male: 42-52
Female: 37-47
Pregnant: >33
1-6 yr: 30-40
6-18 yr: 32-44
Newborn: 44-64
Older adult: Values slightly decreased
Abnormalities in RBC size may alter Hct values.
o WBC
Both sexes: 5-10
≤2 yr: 6.2-17
≥2 yr: 5-10
Newborn, term: 9-30
Anesthetics, stress, exercise, and convulsions can cause increased values.
Drug therapy can decrease values for 24-48 hr.
Pregnancy (final month) and labor may cause increased WBC levels.
o Platelet count
Both sexes: 150-400
Premature infant: 100-300
Newborn: 150-300 Infant: 200-475
Values may increase if living at high altitudes, exercising strenuously, or taking oral
contraceptives
Values may decrease due to hemorrhage, DIC, reduced production of platelets, infections,
prosthetic heart valves, and drugs (acetaminophen, aspirin, chemotherapy, H2-blockers,
INH, Levaquin, streptomycin, sulfonamides, thiazide diuretics).
o PT
Both sexes: 11-12.5
Pregnant: Slight ↓
Used in regulating Coumadin therapy.
Therapeutic range is 1.5-2 times normal/control.
o INR
Both sexes 0.8-1.1
Used to monitor anticoagulation therapy. INR must be individualized.
o PTT
Both sexes: 60-70
Pregnant: Slight ↓
It is used in regulating heparin therapy.
Therapeutic range is 1.5-2.5 times normal or control.
Blood Chemistry
o Albumin: g/dL
Both sexes: 3.5 -5
No special preparation is needed.
o Bilirubin total: mg/dL
Adult
o Total: 0.3-1
Newborn: 1-12
Client is to be NPO except for water for 8-12 hr prior to testing.
Prevent hemolysis of blood during venipuncture.
Do not shake tube; it can cause inaccurate values.
Protect blood sample from bright light.
o Total Calcium: mg/dL
Both sexes: 9-10.5
Values tend to decrease with age
No special preparation is needed.
Use of thiazide diuretics can cause increased calcium values.
o Cholesterol: mg/dL
Both Sexes: <200
Instruct client to fast 12-14 hours after eating a low-fat meal.
o High-density lipoprotein [HDL] (alpha lipoproteins), which are predominantly protein with a
small amount of cholesterol
Male: >45
Female: >55
o Low-density lipoprotein [LDL] (beta lipoproteins), which are primarily cholesterol
<130
Target LDL is ≤70 for client with high risk for CHD.
o Creatinine: mg/dL
Male: 0.6-1.2
Female: 0.5-1.1
Decrease in muscle mass may cause decreased values
It is preferred but not necessary to be NPO 8 hr prior to testing.
A ratio of 20:1, BUN to creatine, indicates adequate kidney functioning.
o Glucose: mg/dL
Both sexes: 70-110
≤2 yr: 60-100 >2 yr: 70-110
Premature infant: 20-60
Newborn: 30-60
Infant: 40-90
Increase in normal range after age 50
Client to be NPO except for water 8 hr prior to testing.
Caffeine can cause increased values.
Stress (e.g., MI, infection, general anesthesia) can cause iatrogenic hyperglycemia.
o Potassium: mEq/L
Both sexes: 3.5-5
Hemolysis of specimen can result in falsely elevated values.
Exercise of the forearm with tourniquet in place may cause increased potassium levels.
o Sodium: mEq/L
Both sexes: 136-145
Do not collect from an arm with an infusing IV solution.
o Urea nitrogen: mg/dL
Both sexes: 10-20
o Thyroid-stimulating hormone (TSH, thyrotropin)
Both sexes: 2-10
The TSH test is used to differentiate primary and secondary hypothyroidism. TSH levels are
subject to a diurnal variation.
Some drugs may cause increased levels (antithyroid medications, lithium, potassium iodide,
and TSH injection). Some drugs may cause decreased levels (aspirin, nonsteroidal
antiarthritics, dopamine, heparin, steroids, and T3).
o Triiodothyronine (T3), ng/dL
Both sexes: 70-205
Primarily to diagnose hyperthyroidism
Total T3 values are increased in pregnancy because serum proteins are increased at that
time.
o Total Thyroxine (T4), mcg/dL
Male: 4-12
Female: 5-12
Newborn: 1-3 days: 11-22
o Newborns are screened to detect hypothyroidism, so mental retardation can be
prevented with early diagnosis. A heel stick is used to collect the blood.
Slight increase in T4 levels during pregnancy.
Stop taking exogenous T4 medication 1 month before testing.
Arterial Blood Chemistry
o pH
Both sexes: 7.35-7.45
o PCO2: mm Hg
Both sexes: 35-45
o PO2: mm Hg
Both sexes: 80-100
o Hco3: mEq/L
Both sexes: 21-28
o O2 saturation: %
Both sexes: 95-100
Urinalysis (UA)
o Appearance
Clear
May be a midstream, clean-catch specimen
Cloudy urine may be caused by the presence of pus (necrotic WBCs), RBCs, or bacteria, or
ingestion of certain foods.
Urine that has been refrigerated for longer than 1 hr can become cloudy.o Color
Yellow to amber
Pale yellow to amber color because of the pigment urochrome (product of bilirubin
metabolism)
The color indicates the concentration of the urine (dilute urine: straw-colored; concentrated
urine: deep amber and varies with specific gravity).
Color can change with ingestion of certain foods or medications.
Urine darkens with prolonged standing.
o Odor
Aromatic
Diabetic ketoacidosis has the strong, sweet smell of acetone.
UTI, the urine may have a foul odor.
When urine stands for a long time and starts to decompose, it has an ammonia-like smell.
o pH
4.6-8.0 (average, 6.0)
Bacteria, UTI, or a diet high in citrus fruits or vegetables may cause increased urine pH.
Urine pH becomes alkaline on standing.
The urine pH of an uncovered specimen will become alkaline.
o Protein
0-8 mg/dL 50-80 mg/24 hr (at rest) <250 mg/24 hr (during exercise)
Proteinuria indicator of renal disease
Test the urine of all pregnant women for proteinuria, an indicator of preeclampsia. If
significant protein is noted at urinalysis, a 24-hr urine specimen should be collected so that
the quantity of protein can be measured.
Transient proteinuria may be associated with severe emotional stress, excessive exercise,
and cold baths.
A first-voided specimen is best to test for protein.
o Specific gravity
Adult: 1.005-1.030 (usually, 1.010-1.025)
Older adult: values decrease with age
Newborn: 1.001-1.020
Renal disease tends to diminish concentrating capability.
Specific gravity is a measurement of hydration status, with overhydration the urine is more
dilute, with dehydration the urine is more concentrated.
Drugs that may cause increased specific gravity include dextran and sucrose.
o Leukocyte esterase
Negative
Positive results indicate UTI.
False-positive results may occur in specimens contaminated by vaginal secretions (heavy
menstrual discharge, trichomonas infection, parasites) that contain WBCs.
False-negative results may occur in specimens containing high levels of protein or ascorbic
acid.
o Nitrites
None
Chemical testing is done with a dipstick containing a reagent that reacts with nitrites to
produce a pink color.
A positive test result indicates the need for a urine culture.
o Ketones
None
Ketones spill over into the urine when blood glucose levels in diabetic patients are elevated.
Ketonuria is associated with poorly controlled diabetes.
Ketonuria may occur with acute febrile illnesses, especially in infants and children.
Special diets (carbohydrate-free, high-protein, high-fat) and some drugs may cause
ketonuria.
Testing for ketones can be performed immediately after urine collection. Dip a reagent stick(Ketostix) into the urine specimen. Read the strip in 15 seconds by comparing it with the
color chart.
o Bilirubin
None
Obstruction of the bile duct by a gallstone causes conjugated hyperbilirubinemia, and unlike
the unconjugated form, conjugated bilirubin is water-soluble and can be excreted into the
urine.
Bilirubin is not stable in urine, especially when exposed to light.
o Crystals
None
Crystals found on microscopic examination indicate that renal stone formation is imminent,
if not already present.
Radiographic contrast media may cause precipitation of urinary crystals.
o Casts
None
For casts to form, the pH must be acidic and the urine concentrated.
Two types of casts: Hyaline casts are conglomerations of protein, and cellular casts are
conglomerations of degenerated cells.
o Glucose
Fresh specimen: none
24-hr specimen: 50-300 mg/24 hr
The kidney does not excrete glucose unless blood levels exceed approximately 180 mg/dL,
so can reflect the degree of glucose elevation in the blood.
Collect a fresh double-voided specimen.
In pregnancy glycosuria is common, but persistent and significantly high levels may indicate
gestational diabetes.
o White blood cells (WBCs)
0-4 per low-power field
The presence of five or more WBCs in the urine indicates a UTI involving the bladder or
kidneys, or both. A clean-catch urine culture should be done for further evaluation.
Vaginal discharge may contaminate the urine specimen and factitiously cause WBCs in the
urine.
o WBC casts
None
WBC casts are most frequently found in infections of the kidney, poststreptococcal
glomerulonephritis, or inflammatory nephritis.
o Red blood cells (RBCs)
≤2
Hematuria can be microscopic or gross.
Bladder, ureteral, and urethral diseases are the most common causes of RBCs in the urine.
The most common cause of RBCs in the urine is from contamination of menses, so before
collection of the sample, determine whether the patient is having a period.
Traumatic urethral catheterization may cause RBCs in the urine.
o RBC casts
None
RBC casts suggest glomerulonephritis interstitial nephritis, acute necrosis, pyelonephritis,
renal trauma, or renal tumor.
Strenuous physical exercise may cause RBC casts.
o Volume
24-hr specimen is required.
If a 24-hr urine collection is needed, refrigerate urine during the collection period.
Recommended Daily Requirements and Food Sources
Fat-Soluble Vitamins ADEKo A
Liver
Egg yolks, fortified margarine, and butter
Dark green and deep orange fruits and vegetables (e.g., apricots, broccoli, cantaloupe,
carrots, pumpkin, winter squash, sweet potatoes, and spinach)
o D
Fortified and full-fat dairy products
Fish oil
Can be synthesized in the skin when exposed to sunlight
o E
Vegetable oils and their products such as salad oils, margarine, nuts, seeds, avocado, and
mango
o K
Green leafy vegetables (e.g., lettuce, cabbage, spinach), peas, asparagus, meat, milk, and
soybean oil
Water-Soluble Vitamins C, the B’s, and Folic Acid
o C
Citrus fruits, cantaloupes, strawberries, tomatoes, potatoes, broccoli, green peppers, and
spinach
o B1 (thiamine)
Pork, beef, liver, whole grains, legumes, and wheat germ
o B2 (riboflavin)
Liver, milk, milk products, soybeans, and enriched cereals
o B3 (nicotinic acid)
Meat, poultry, fish, peanuts, and enriched grains
o B6 (pyridoxine)
Meat, poultry, grains, seeds, and seafood
o Folic acid
Liver, beans, peas, spinach, and yeast
o B12
Shellfish, liver, fish, and lean meat
Minerals
o Calcium
Milk, cheese, dark green vegetables, dried figs, soy, and legumes
o Phosphorus
Milk, liver, legumes, fish, and soy
o Magnesium
Whole grains, green leafy vegetables, tea, nuts, and fruit
o Iron
Meats, eggs, legumes, whole grains, green leafy vegetables, and dried fruits
o Iodine
Marine fish, shellfish, dairy products, iodized salt, and some breads
o Potassium
Citrus fruits and dried fruits, bananas, watermelon, potatoes, legumes, tea, and peanut
butter
o Zinc
Meats, seafood, and whole grains
Foods High in Sodium
o Vegetables
Canned vegetables
Carrots, particularly canned
Tomatoes, particularly canned
Tomato catsup
Tomato juice
o Condiments Bouillon cubes
Mustard, prepared
Olives, pickled, canned or bottled
Pickles, cucumber, dill
Salad dressings, commercially prepared
Soy sauce
o Miscellaneous
Bacon
Cheeses
Ready-to-eat breakfast cereals
Peanut butter
Soups, commercially prepared, canned
Corned beef
[Show More]
Last updated: 3 years ago
Preview 1 out of 67 pages
Buy Now
Instant download

Buy this document to get the full access instantly
Instant Download Access after purchase
Buy NowInstant download
We Accept:

Reviews( 0 )
$13.50
Can't find what you want? Try our AI powered Search
57
0
Document information
Connected school, study & course
About the document
Uploaded On
Mar 16, 2021
Number of pages
67
Written in
All
Additional information
This document has been written for:
Uploaded
Mar 16, 2021
Downloads
0
Views
57