OSTEOMYELITIS/SURGERY
Unfolding Reasoning
Gene Potts, 78 years old
Primary Concept
Infection
Interrelated Concepts (In order of emphasis)
• Tissue Integrity
• Perfusion
• Gas Exchange
• Pain
• Clinical
...
OSTEOMYELITIS/SURGERY
Unfolding Reasoning
Gene Potts, 78 years old
Primary Concept
Infection
Interrelated Concepts (In order of emphasis)
• Tissue Integrity
• Perfusion
• Gas Exchange
• Pain
• Clinical Judgment
• Patient Education
• Communication
• Collaboration
NCLEX Client Need Categories Percentage of Items from Each Category/Subcategory Covered in Case Study
Safe and Effective Care Environment
Management of Care 17-23%
Safety and Infection Control 9-15%
Health Promotion and Maintenance 6-12%
Psychosocial Integrity 6-12%
Physiological Integrity
Basic Care and Comfort 6-12%
Pharmacological and Parenteral Therapies 12-18%
Reduction of Risk Potential 9-15%
Physiological Adaptation 11-17%
History of Present Problem:
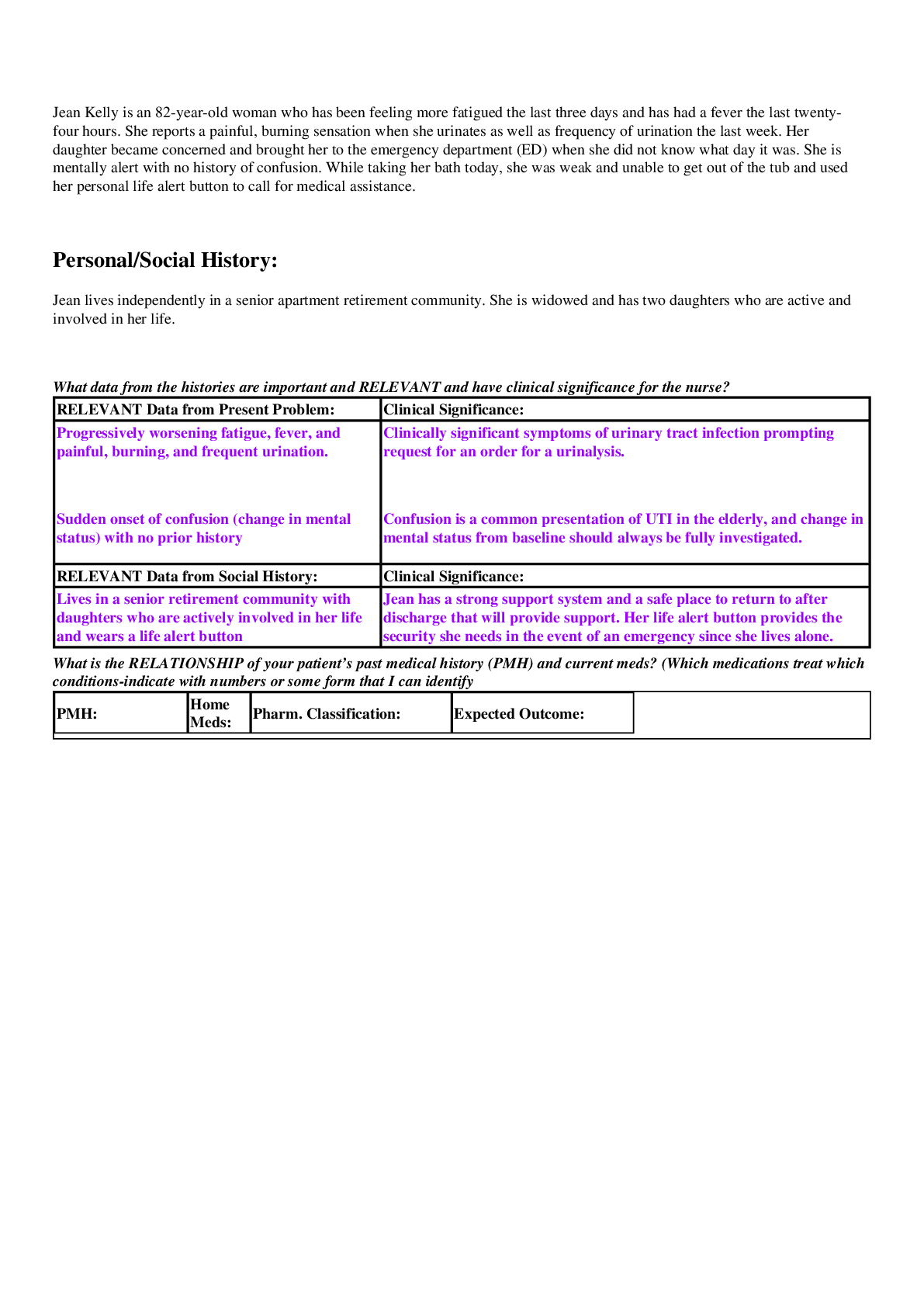
Gene Potts is a 78-year-old Caucasian male with diabetes type 2, MRSA cultured in left foot ulcer and dementia who came to the emergency department because he had increased pain in left foot, chills, fever and feeling weaker the past two days. His wife noticed an increase in redness and swelling of his chronic left foot ulcer. Initial vital signs: T: 101.5 F/38.6 C P: 98 R: 22 BP: 148/90. O2 sat: 94% room air.
His left great toe is black with an open stage III ulcer 1x1 cm on the top of his left foot. Surrounding tissue is bright red and extends from his left foot to his lower left leg. His initial WBC: 18.5, lactate: 1.8, and creatinine: 1.7. A CT of his left foot confirmed osteomyelitis in the left great toe. He is admitted to the med/surg floor and started on piperacillin/tazobactam IVPB and vancomycin IVPB. He is scheduled to have his left great toe amputated in surgery tomorrow.
Personal/Social History:
Gene has been married for 55 years and is cared for by his wife, Ruth, who is a retired nurse. They have no children. His dementia has progressed, and Gene no longer recognizes his wife. He has become more difficult for his wife to manage at home. Gene is DNR/DNI. Palliative care was consulted to clarify goals of care and communicated that Gene is at high risk for decline after surgery and may require skilled care after discharge. Ruth is stern and communicates that she knows her husband best and insistent that he will come home after surgery no matter what.
What data from the histories are RELEVANT and must be interpreted as clinically significant by the nurse?
(Reduction of Risk Potential)
RELEVANT Data from Present Problem: Clinical Significance:
RELEVANT Data from Social History: Clinical Significance:
What is the RELATIONSHIP of your patient’s past medical history (PMH) and current meds?
(Which medications treat which conditions? Draw lines to connect)
PMH: Home Meds: Pharm. Classification: Expected Outcome:
• Ischemic cardiomyopathy with EF of 35-40%
• Atrial fibrillation/flutter
• CVA
• Obstructive sleep apnea
• Coronary artery disease
• Type 2 diabetes-diet controlled
• Chronic kidney disease
• Gout • Allopurinol 100 mg PO daily
• Atorvastatin 10 mg PO at HS
• Docusate 100 mg PO daily
• Fluoxetine 20 mg PO daily
• Furosemide 40 mg PO daily
• Losartan 50 mg PO daily
• Metoprolol XL 50 mg PO daily
• Warfarin 5 mg PO daily
One disease process often influences the development of other illnesses. Based on your knowledge of pathophysiology (if applicable), which disease likely developed FIRST that created a “domino effect” in her life?
• Circle what PMH problem likely started FIRST
• Underline what PMH problem(s) FOLLOWED as domino(s):
Patient Care Begins: Post-Op-Day of Surgery
........................................................Continued.....................................
[Show More]
.png)