SOAP Note Template
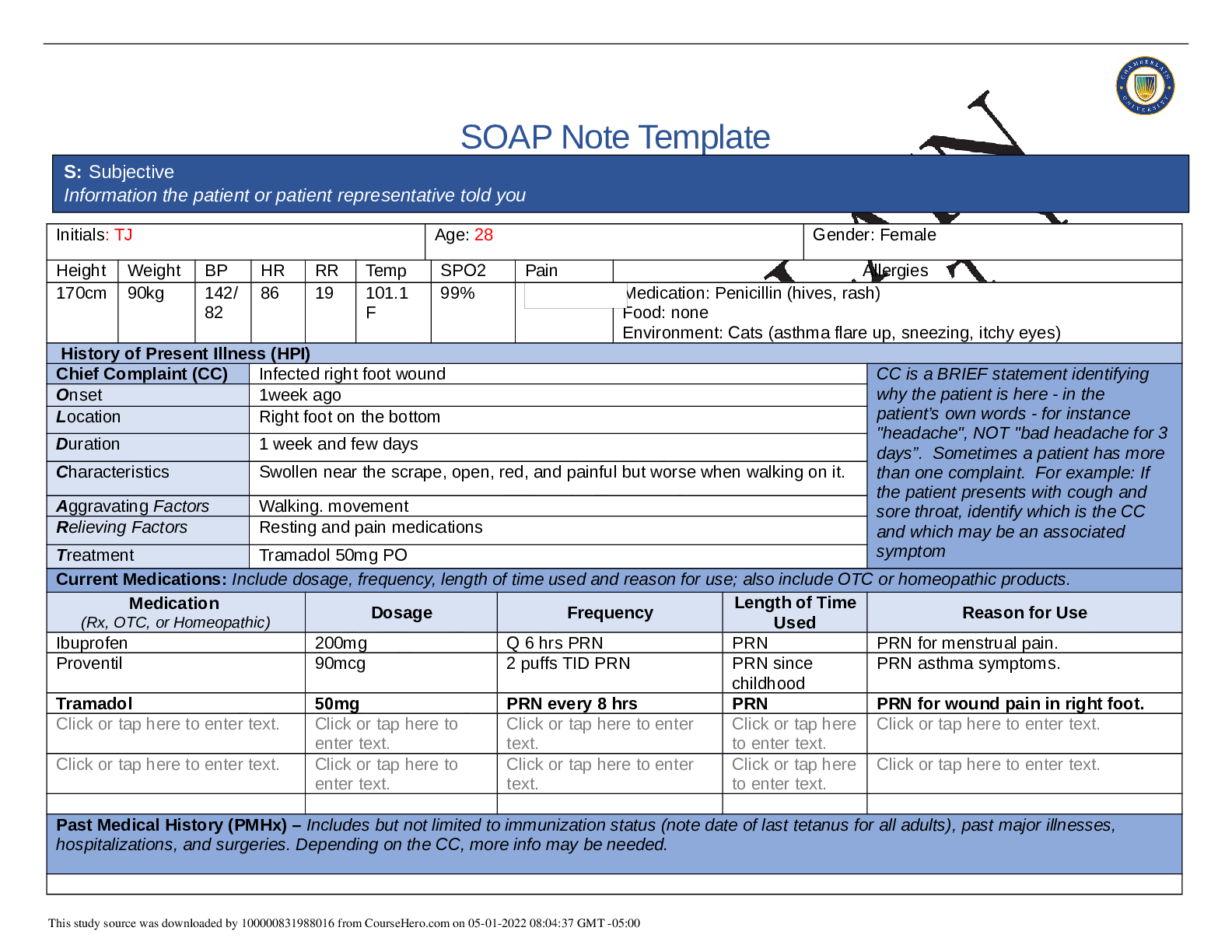
Initials: TJ Age: 28 Gender: Female
Height Weight BP HR RR Temp SPO2 Pain Allergies
170cm 88kg 139/
87
82 16 98.9F 99% Medication: Penicillin (rash/ hives)
Food: none
Environment: Cats, dust (as
...
SOAP Note Template
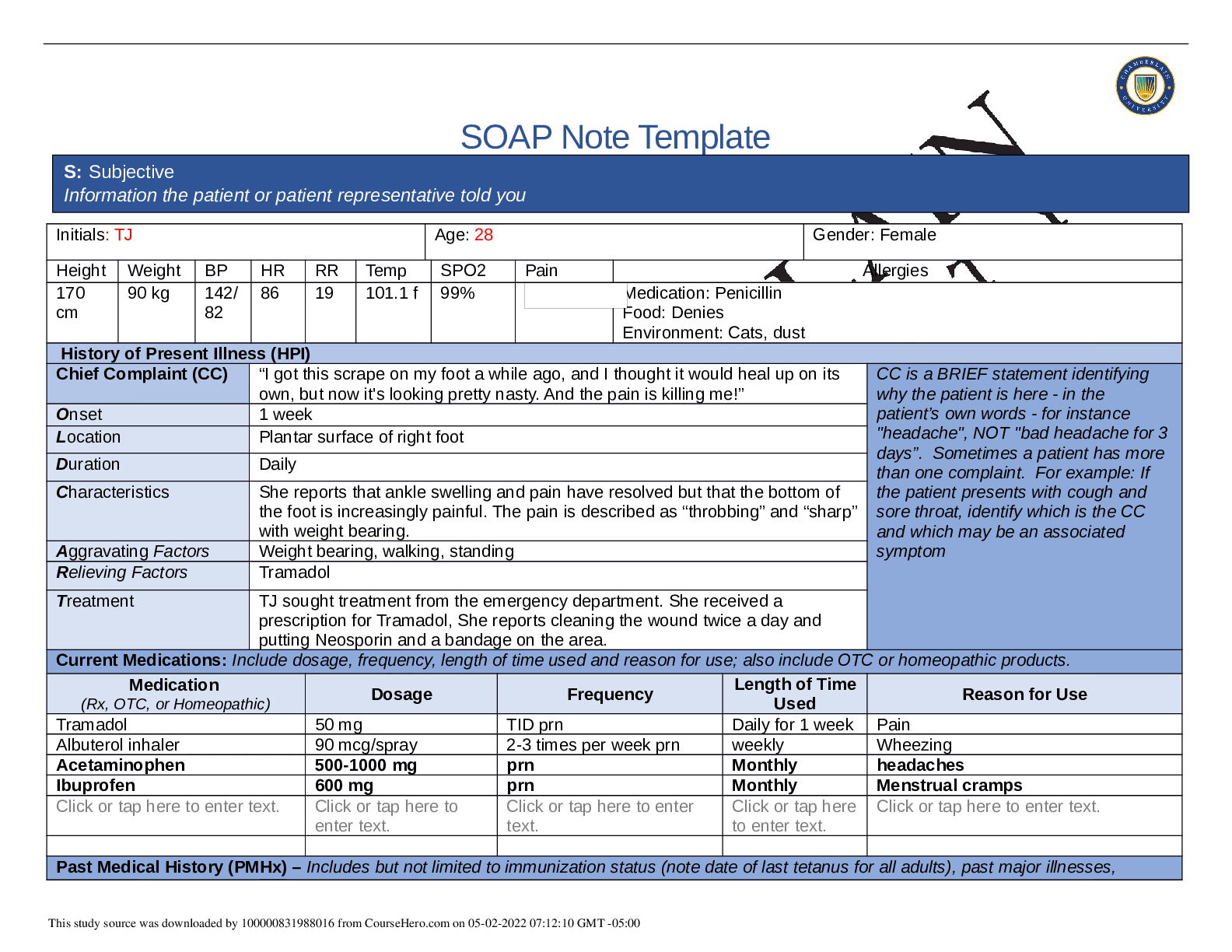
Initials: TJ Age: 28 Gender: Female
Height Weight BP HR RR Temp SPO2 Pain Allergies
170cm 88kg 139/
87
82 16 98.9F 99% Medication: Penicillin (rash/ hives)
Food: none
Environment: Cats, dust (asthma flares up, itchy, watery eyes, sneezing)
History of Present Illness (HPI)
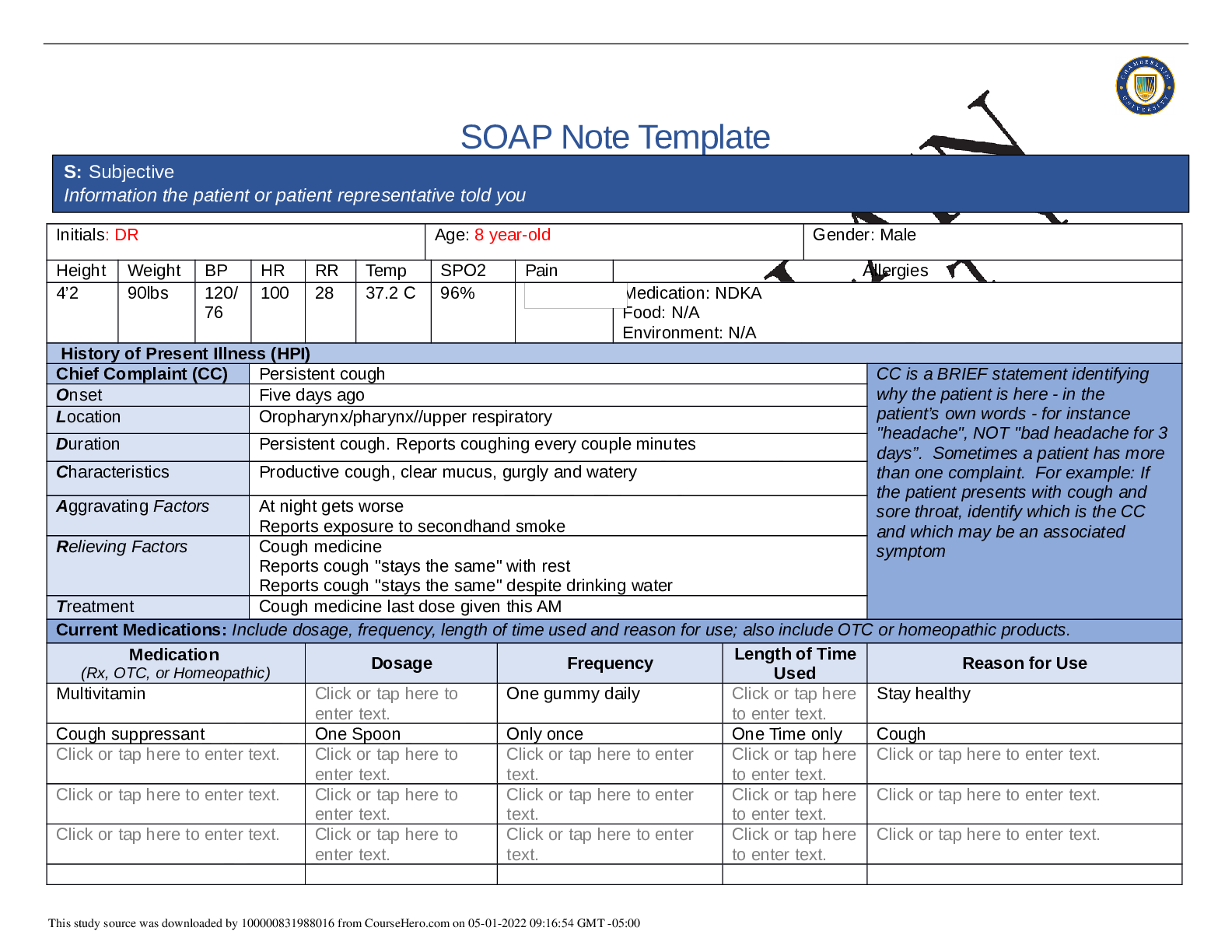
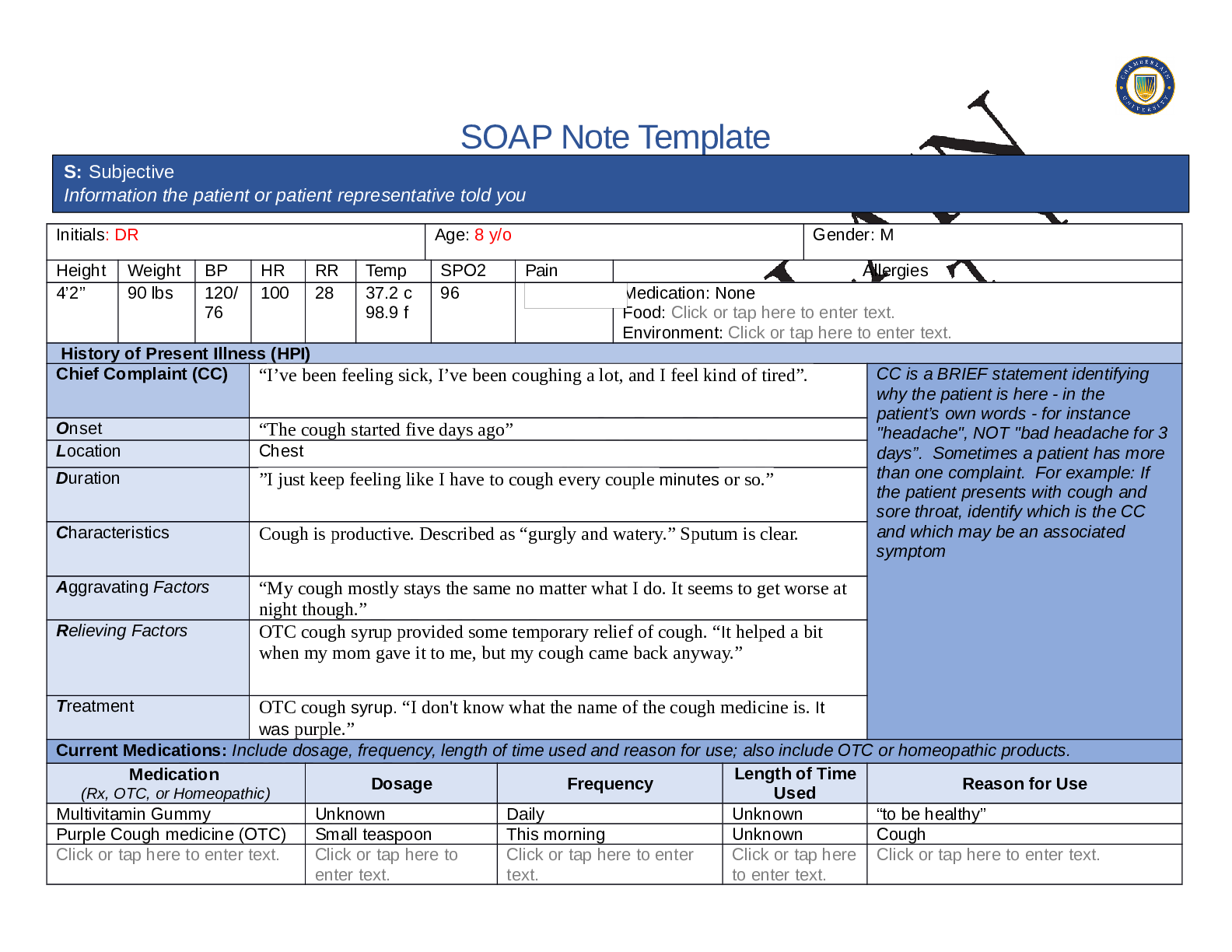
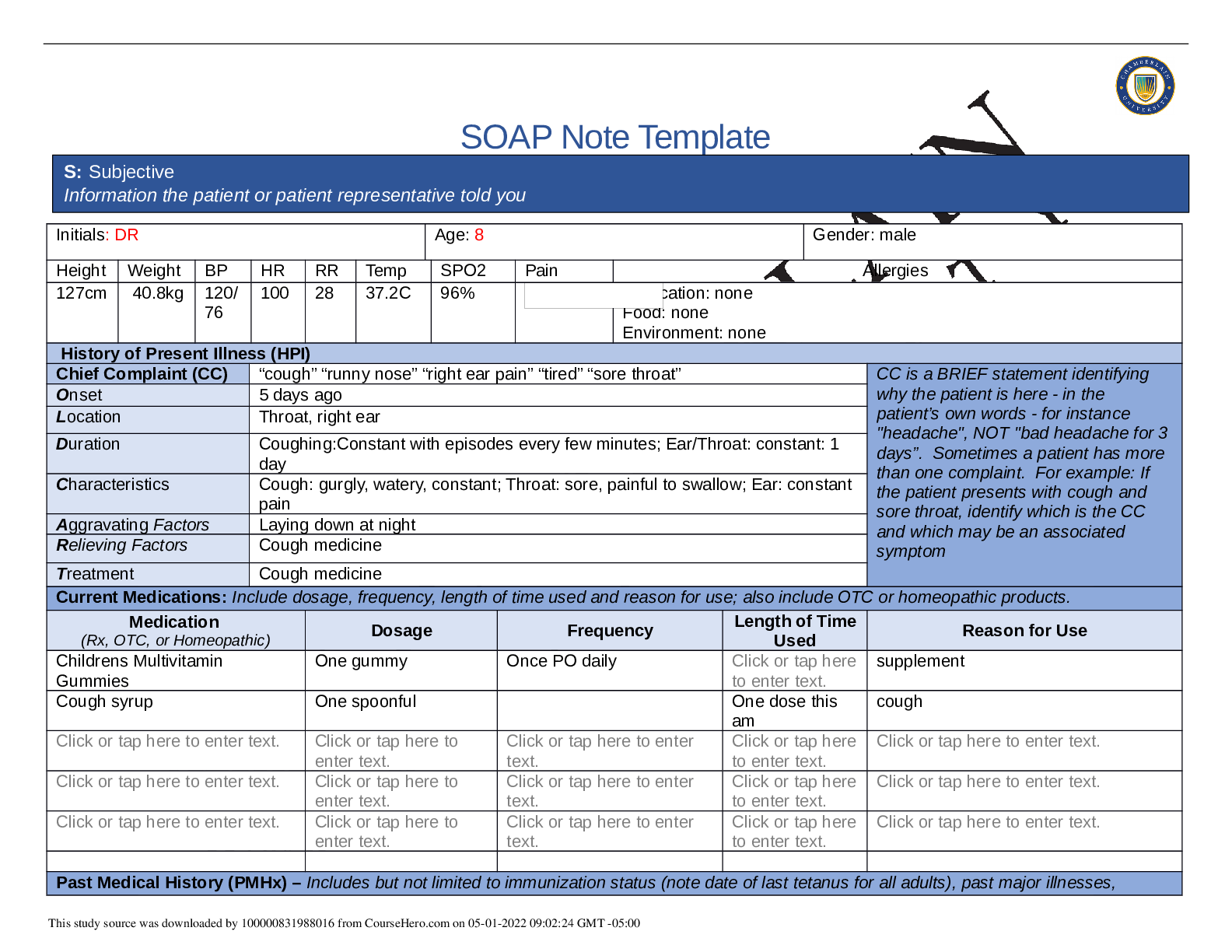
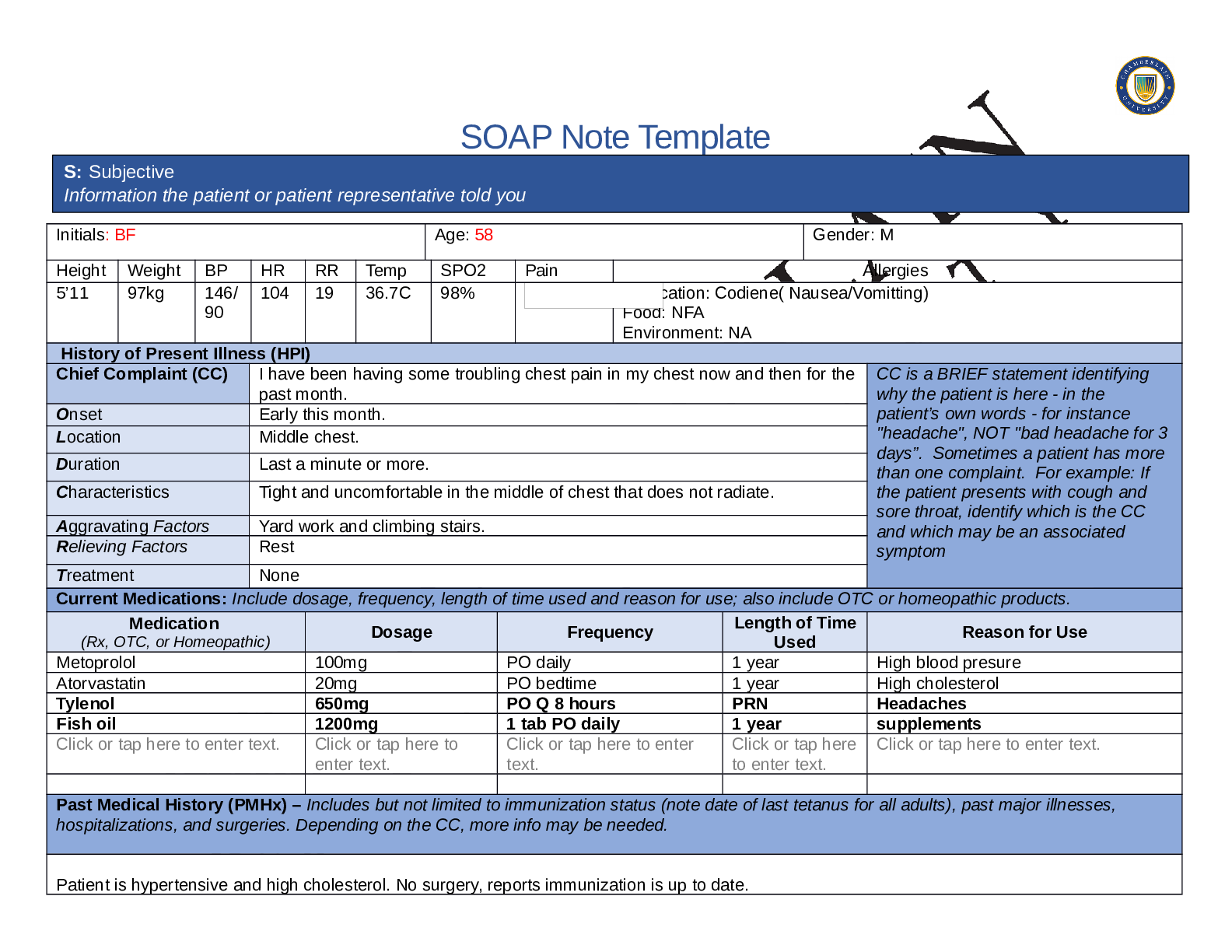
Chief Complaint (CC) Headache CC is a BRIEF statement identifying
why the patient is here - in the
patient’s own words - for instance
"headache", NOT "bad headache for 3
days”. Sometimes a patient has more
than one complaint. For example: If
the patient presents with cough and
sore throat, identify which is the CC
and which may be an associated
symptom
Onset 5 days ago
Location Pain is located at the crown and back of head.
Duration Intermittent- daily-lasts for 1-2hrs per episode.
Characteristics Dull headache, non- radiating, associated with neck pain
Aggravating Factors Movement of head
Relieving Factors Tylenol- improved pain to 3/10 ,rest
Treatment No other treatment
Current Medications: Include dosage, frequency, length of time used and reason for use; also include OTC or homeopathic products.
Medication
(Rx, OTC, or Homeopathic) Dosage Frequency Length of Time
Used Reason for Use
Proventil 2 puffs PRN for asthma PRN Rescue inhaler for asthma
exacerbation
Flovent Patient unaware of
exact dosage
BID Daily Mainenence for Asthma
Tylenol 2- regular strength
tabs
Once a day Once a day for
5 days
For headache
Advil 200mg PRN PRN For menstrual cramps
N/A Click or tap here to
enter text.
Click or tap here to enter
text.
Click or tap here
to enter text.
Click or tap here to enter text.
Past Medical History (PMHx) – Includes but not limited to immunization status (note date of last tetanus for all adults), past major illnesses,
hospitalizations, and surgeries. Depending on the CC, more info may be needed.
S: Subjective
Information the patient or patient representative told you
This study source was downloaded by 100000831988016 from CourseHero.com on 05-01-2022 07:59:44 GMT -05:00
Should include: the accident MVA, should pertain to the Chief complaint, 15mile accident in parking lot, wearing seat belt, rear end fender bender.
Was not drinking alcohol. (Asthma dx age 2.5 yrs old, Diabetes dx at 24yrs old, Denies surgical history, last hospital admission at 16 yrs old for
asthma exacerbation. Reports all Immunization are current at this visit, Last Flu vaccine: 5 or 6 years ago per patient, declines at this time Last
Tetanus booster: two years ago Reports Meningitis Vaccine at 19yrs old.
Social History (Soc Hx) - Includes but not limited to occupation and major hobbies, family status, tobacco and alcohol use, and any other pertinent
data. Include health promotion such as use seat belts all the time or working smoke detectors in the house.
Supervisor at Mid-American Copy & Ship, Bachelor’s accounting student, Hobbies:Reading, watchingTV, hanging with friends and going to church.
Close with mother and sister (living together), Brother lives with fiancee, father deceased from car accident. Denies tobacco use. Alcohol use
socially with friends ( rum and diet coke drink of choice). Drives and always uses a seatbelt, working smoke detector in house.
Family History (Fam Hx) - Includes but not limited to illnesses with possible genetic predisposition, contagious or chronic illnesses. Reason for
death of any deceased first degree relatives should be included. Include parents, grandparents, siblings, and children. Include grandchildren if
pertinent.
Mother- high cholesterol and hypertension
Father (deceased at 58 car accident 2 years ago)- Hx of Diabetes, high cholesterol and hypertension
Brother 25 y.o.- Obesity
Sister 14 yrs old- dx age 2 or 3 with asthma.
maternal grandma- HTN and high cholesterol
maternal grandpa-HTN and high cholesterol.
paternal grandma-HTN and high cholesterol
paternal grandpa- (deceased) colon cancer, HTN, diabetes.
Review of Systems (ROS): Address all body systems that may help rule in or out a differential diagnosis Check the box next to each positive
symptom and provide additional details.
Constitutional Skin HEENT
☐Fatigue Denies
☐Weakness Denies
☐Fever/Chills Denies
☐Weight Gain Denies
☐Weight Loss Denies
☐Trouble Sleeping Denies
☐Night Sweats Denies
☐Other:
☐Itching Denies
☐Rashes Denies
☐Nail Changes Denies
☐Skin Color Changes
Denies
☐Other:
Click or tap here to
enter text.
☐Diplopia Denies
☐Eye Pain Denies
☐Eye redness Denies
☒Vision changes blurry
when does a lot of
reading
☐Photophobia Denies
☐Eye discharge Denies
☐Earache Denies
☐Tinnitus Denies
☐Epistaxis Denies
☐Vertigo Denies
☐Hearing Changes Denies
☐Hoarseness Denies
☐Oral Ulcers Denies
☐Sore Throat Denies
☐Congestion Denies
☐Rhinorrhea Denies
☐Other:
Click or tap here to enter text.
This study source was downloaded by 100000831988016 from CourseHero.com on 05-01-2022 07:59:44 GMT -05:00
Click or tap here to enter
text.
Respiratory Neuro Cardiovascular
☐Cough denies
☐Hemoptysis denies
☐Dyspnea denies
☐Wheezing denies
☐Pain on Inspiration denies
☐Sputum Production
☐Other: Click or tap here to enter
text.
☐Syncope or
Lightheadedness denies
☒Headache reports tension
☐Numbness denies
☐Tingling denies
☒Sensation Changes
☐Speech Deficits denies
☒Other: denies sensation
changes
☐Chest pain denies
☐SOB denies
☐Exercise Intolerance denies
☐Orthopnea denies
☐Edema unable to assess
☐Murmurs unable to assess
☐Palpitations unable to
assess
☐Faintness unable to assess
☐OC Changes denies
☐Claudications denies
☐PND denies
☐Other: Click or tap here to
enter text.
MSK GI GU PSYCH
☐Pain denies
☒Stiffness reports neck stiffness
☐Crepitus unable to assess
☐Swelling denies
☐Limited ROM
☐Redness denies
☐Misalignment denies
☐Other: Click or tap here to enter
text.
☐Nausea/Vomiting denies
☐Dysphasia denies
☐Diarrhea denies
☐Appetite Change denies
☐Heartburn denies
☐Blood in Stool denies
☐Abdominal Pain denies
☐Excessive Flatus denies
☐Food Intolerance denies
☐Rectal Bleeding denies
☐Other:
Click or tap here to enter text.
☐Urgency denies
☐Dysuria denies
☐Burning denies
☐Hematuria denies
☐Polyuria denies
☐Nocturia denies
☐Incontinence denies
☐Other: Click or tap here to
enter text.
☐Stress denies
☐Anxiety denies
☐Depression denies
☐Suicidal/Homicidal Ideation
denies
☐Memory Deficits denies
☐Mood Changes denies
☐Trouble Concentrating
denies
☐Other: Click or tap here to
enter text.
GYN
☐Rash denies
☐Discharge denies
☐Itching denies
☒Irregular Menses reports almost two months
between periods
☐Dysmenorrhea denies
☐Foul Odor denies
☐Amenorrhea denies
☒LMP: started a few days ago
☐Contraception Denies taking for 3 yrs now
☐Other:Click or tap here to enter text.
This study source was downloaded by 100000831988016 from CourseHero.com on 05-01-2022 07:59:44 GMT -05:00
O: Objective
Information gathered during the physical examination by inspection, palpation, auscultation, and palpation. If unable to assess a body
system, write “Unable to assess”. Document pertinent positive and negative assessment findings.
This study source was downloaded by 100000831988016 from CourseHero.com on 05-01-2022 07:59:44 GMT -05:00
Body System Positive Findings Negative Findings
General
Click or tap here to enter text. Patient is alert and oriented, pleasant. normal stature while
sitting on the exam table, dressed appropriately, and well
groomed. In no acute distress and maintains eye contact during
examination.
Skin
Decreased sensation of bilateral feet and inspected skin darkening
on the neck.
Neg inspection for wounds, rash, or lesions
HEENT
Visual acuity: Right eye is 20/40 and Left eye is 20/20. Needed to add, the fundoscopic exam- positive for cotton wool
bodies. Neg for Papilledema.
Head: no trauma, round, and normocephalic. Ears- intact no
hearing issues. Pupils are equal, round, and reactive to light.
Nose: sense of smell intact, sense of taste: intact,
Respiratory
Click or tap here to enter text. Respirations are 16, patient chest rise symmetrical, no
respiratory distress noted, patient spo2 =99% on room air.
Neuro
Decreased sensation in bilateral feet (bottom soles)
Abstract thinking, attention span, comprehension,general
knowledge, judgment, memory, vocabulary, articulation, 12
cranial nerves, optic and oculomotor nerves, extraocular eye
movements, weber test, Rinne test, gait, graphesthesia,
stereognosis all within normal limits.
Cardiovascular
Click or tap here to enter text. Click or tap here to enter text.
Musculoskeletal
Click or tap here to enter text. Gait is balanced and normal.
Gastrointestinal
Click or tap here to enter text. Click or tap here to enter text.
Genitourinary
Click or tap here to enter text. Click or tap here to enter text.
This study source was downloaded by 100000831988016 from CourseHero.com on 05-01-2022 07:59:44 GMT -05:00
Problem List
1. Headache 6 Click or tap here to enter text. 11 Click or tap here to enter text.
2 Neck sore 7 Click or tap here to enter text. 12 Click or tap here to enter text.
3 Neck stiffness 8 Click or tap here to enter text. 13 Click or tap here to enter text.
4 blurry vision 9 Click or tap here to enter text. 14 Click or tap here to enter text.
5 diabetes 10 Click or tap here to enter text. 15 Click or tap here to enter text.
Diagnosis ICD-10 Code Pertinent Findings
Headache
Correct one: post-traumatic
headache is the correct
diagnosis
R 51 Patient complains of 3 out of 10 headache pain at the crown
and back of head
Correct: pos MVA,
Neck pain M54.2 Patient c/o neck soreness after a car accidnet
Neck strain S16.1XXA Patient c/o neck stiffness after a car accident.
Diagnostics: List tests you will order this visit
Test Rationale/Citation
N/A unless symptoms unresolved by
follow up appointment.
According to Wang & Yeh (2019), CT is used if <72hrs of trauma, for suspected intracranial bleed. No
fever associated, headache pain reported is not severe and does not escalate.
N/A
Click or tap here to enter text.
N/A Click or tap here to enter text.
N/A Click or tap here to enter text.
N/A Click or tap here to enter text.
Medications: List medications/treatments including OTC drugs you will order and “continue previous meds” if pertinent.
Drug Dosage Length of Treatment Rationale/Citation
A: Assessment
Medical Diagnoses. Provide 3 differential diagnoses which may provide an etiology for the CC. The first diagnosis (presumptive
diagnosis) is the diagnosis with the highest priority. Provide the ICD-10 code and pertinent findings to support each diagnosis.
P: Plan
Address all 5 parts of the comprehensive treatment plan. If you do not wish to order an intervention for any part of the treatment plan, write
“None at this time” but do not leave any heading blank. No intervention is self-evident. Provide a rationale and evidence-based in-text citation for
each intervention.
This study source was downloaded by 100000831988016 from CourseHero.com on 05-01-2022 07:59:44 GMT -05:00
Acetaminophen
Don’t give muscle relaxer
(dangerous)
650mg Every 6hrs PRN Headache Is the lowest cost recommended
treatment for acute headache
(Papadakis, McPhee, & Bernstein,
2019).
Continue home meds Click or tap here to enter text. Click or tap here to enter text. Click or tap here to enter text.
N/A Click or tap here to enter text. Click or tap here to enter text. Click or tap here to enter text.
N/A Click or tap here to enter text. Click or tap here to enter text. Click or tap here to enter text.
N/A Click or tap here to enter text. Click or tap here to enter text. Click or tap here to enter text.
Referral/Consults:
Refer to an opthamologist Rationale/Citation Patient complains of blurry vision
and headaches when reading or
studying. Snellen eye chart results
show that right and left eye visual
acuity differs (Goadsby et al,
2019).
Education:
Due to a normal neurological exam, and a dull headache pain that
does not escalate and relieved by OTC Tylenol, I will educate patient to
continue headache treatment with Tylenol and to follow up if symptoms
worsen.
Rationale/Citation Tylenol for treatment for acute
headache (Papadakis, McPhee, &
Bernstein, 2019).
Follow Up: Indicate when patient should return to clinic and provide detailed instructions indicating if the patient should return sooner than
scheduled or seek attention elsewhere.
Follow up at the clinic in 1 week if not better. If symptoms of headache
worsen or sever headache, call 911 in case of an emergency and seek
medical attention.
Rationale/Citation According to Goadsby, et al.,
(2019), after treatment has been
initiated, follow-up care is
essential to identify whether
progress has been made against
the headache complaint.
References
Include at least one evidence-based peer-reviewed journal article which relates to this case. Use the correct APA 6th edition formatting.
Goadsby PJ, Jameson J, Fauci AS, Kasper DL, Hauser SL, Longo DL, Loscalzo J. (2019). Harrison's principles of internal medicine: Headache,
20ed. New York, NY: McGraw-Hill. Retrieved from: http://accessmedicine.mhmedical.com.chamberlainuniversity.idm.oclc.org/content.aspx?
bookid=2129§ionid=192011003.
Maxine A. Papadakis, Stephen J. McPhee, Jennifer Bernstein. (2019). Quick Medical Diagnosis & Treatment: Headache, acute New York, NY:
McGraw-Hill. Retrieved from: http://accessmedicine.mhmedical.com.chamberlainuniversity.idm.oclc.org/content.aspx?
bookid=2566§ionid=206884926. Accessed September 21, 2019.
This study source was downloaded by 100000831988016 from CourseHero.com on 05-01-2022 07:59:44 G
[Show More]